The use of laser light to treat cancer and other disorders is not now considered standard, but emerging approaches based on nanoparticles show promise in improving established techniques. Researchers examine the state of the field and discover that by combining photothermal therapy or photodynamic therapy with nanomaterials, they have been able to administer these types of phototherapies while also delivering medications to previously inaccessible areas in the body. PTT and PDT can also be combined as a single treatment to create an even more potent therapy approach.
Near-infrared (NIR) light has gained intense study attention in nanomedicine in recent years due to its exceptional tissue penetration capacity for either direct photothermal death of malignancies or finely regulated medication release.
The use of laser light to treat cancer and other disorders is not yet considered conventional in the clinical context, but emerging approaches based on nanoparticles show promise in improving established techniques.
Photothermal therapy (PTT) is a technology that turns laser light into heat that can target and kill tumor cells. Photodynamic treatment (PDT) is another technique that uses laser light to generate reactive oxygen species (ROS) such as hydroxyl radicals, singlet oxygen, superoxide radicals, and hydrogen peroxide, which can destroy tumor cells.
“The penetration depth of laser light into tissues is crucial in determining therapeutic efficiency in cancer therapies utilizing this technique. The form of the beam, the wavelength of the light, the strength of the laser, and the radius of the beam are all factors that influence the penetration depth.
Masoud Mozafari
An international team of researchers evaluates the present state of the field of nanoparticle-enhanced PDT and PTT in Applied Physics Reviews, published by AIP Publishing, and focuses on combining the two approaches to obtain the highest level of treatment efficiency.
Researchers have been able to apply these types of phototherapies while simultaneously delivering medications to locations in the body that would normally be inaccessible by combining PTT or PDT with nanomaterials. PTT and PDT can also be combined as a single treatment to create an even more potent therapy approach.
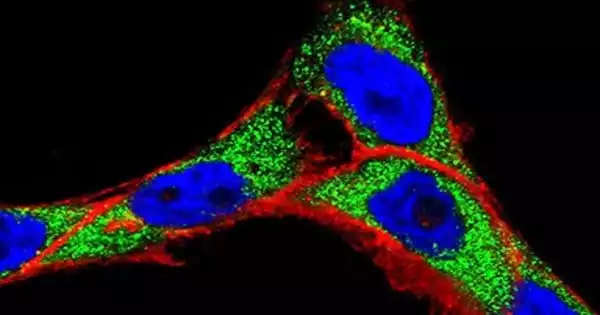
The surface of the nanoparticle can be changed in order to bind a photosensitive molecule to it. This enables the absorption of light at a certain wavelength. This light is turned to heat using the PTT method. The light in PDT generates ROS. For PDT to be effective, there must be enough ambient oxygen present to generate enough ROS to kill tumor cells.
Nanocarriers (NCs) have recently received a lot of interest due to their structural capabilities, good biocompatibility, and biodegradability. Scientists are very interested in the development of effective NCs with stimuli-responsive characteristics. The primary purpose of creating drug delivery NCs is to address the delivery-related issues associated with traditional chemotherapy and to transport medications to the intended locations of action while minimizing unpleasant side effects.
“The penetration depth of laser light into tissues is crucial in determining therapeutic efficiency in cancer therapies utilizing this technique,” said author Masoud Mozafari of Iran University of Medical Sciences.
The form of the beam, the wavelength of the light, the strength of the laser, and the radius of the beam are all factors that influence the penetration depth. Combining PDT with established medical therapies, such as chemotherapy, to develop photodynamic antibacterial chemotherapy, is a strong method.
Chemotherapeutic drugs or antibiotics can be delivered to the tumor location using nanoparticles. Antibiotics can be released to prevent infection in the treated area when light is delivered, creating ROS molecules in the tumor and destroying both tumor cells and bacteria. Other tweaks to the nanoparticle surface may allow it to traverse the blood-brain barrier, allowing it to treat brain cancers.
Nanoscale biomaterials are gaining popularity due to their limitless potential to improve human health as hard tissue engineering materials. Tissue engineering is a field that blends materials science and engineering with biology and involves the use of materials to stimulate tissue regeneration. Tissue engineering’s overarching goal is to manage the cellular interaction with synthetic designed materials for the therapy of structurally deteriorated organs in the human body.
One set of tests examined in this article used gold nanorods with a glycoprotein from the rabies virus attached to their surface. Because this virus normally infects the brain, the gold nanorods were able to cross the blood-brain barrier and target the brain tumor. Using a laser to generate targeted heat, the nanorods were able to kill the tumor cells. These techniques can also be utilized to treat various medical concerns such as atherosclerosis, scar removal, abscesses, nonhealing ulcers, and tooth infections.