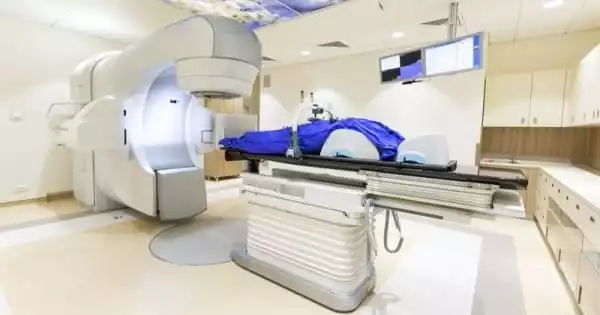
Radiotherapy is a highly complex, multi-step process that necessitates the participation of many different staff groups in the treatment’s planning and delivery. Such complication creates a plethora of opportunities for errors to occur. Though major incidents are rare, the consequences can be severe, as evidenced by the few but disturbing high-profile incidents reported recently.
The amount of data that goes into treatment machines has increased in tandem with the complexity of radiation therapy. More data means more opportunities for data transfer errors. A medical physics researcher is working to reduce the likelihood of such errors.
In the same way, that helicopter traffic reporters use their “bird’s eye view” to safely route drivers around roadblocks, radiation oncologists treating a variety of cancers can use new guidelines developed by a West Virginia University researcher to reduce data transfer errors and treat their patients more safely.
The most common error in radiation oncology is the transfer of information from one system to another. This report provides you with a good, bird’s-eye view of how data moves around in your department.
Ramon Alfredo Siochi
WVU’s director of medical physics, Ramon Alfredo Siochi, led a task group to help ensure the accuracy of data that dictates a cancer patient’s radiation therapy. The measures he and his colleagues advocated in their new report protect against medical errors in a treatment that is administered to more than half of all cancer patients.
“The most common error in radiation oncology is the transfer of information from one system to another,” said Siochi, associate chair of the School of Medicine’s Department of Radiation Oncology. “This report provides you with a good, bird’s-eye view of how data moves around in your department.”
“How often do these mishaps occur?” According to one estimate, three out of every hundred patients may have an error, but it does not necessarily harm them. I’m not sure what the rate of errors that are quote-unquote “near misses” (when an error occurs before it affects the patient) is, but I’m guessing it’s much higher.
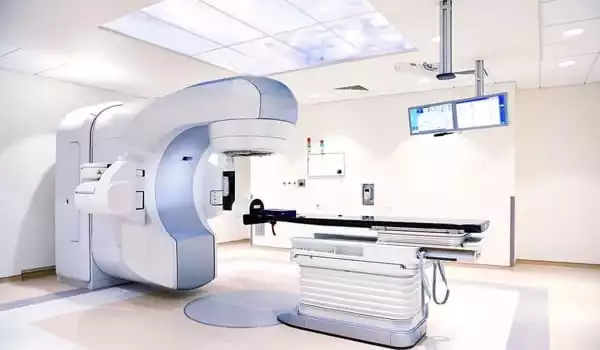
Siochi recently chaired the American Association of Physicists in Medicine’s Task Group of Quality Assurance on External Beam Treatment Data Transfer. The organization was founded in response to media coverage of radiation overdoses caused by faulty data transfer.
“In 2010, the New York Times reported that a patient [in a New York City hospital] has overdosed with radiation because data didn’t transfer properly from one system to another,” Siochi said. “To cut a long story short, the patient received a lethal dose of radiation to his head that went undetected for three days. That now falls into the broad category of many things happening that were not standard practice. However, it could have been avoided.”
Radiation therapy is used to treat a wide range of cancers, including lung, pancreas, prostate, breast, brain, and bladder cancers. Depending on the type or stage of cancer, radiation may cure, shrink, or prevent it from returning. However, as the complexity of radiation therapy has increased, allowing cancers that were previously too difficult to treat to be targeted, so has the amount of data that goes into treatment machines. More data means more opportunities for errors.
When Siochi began practicing radiation oncology physics in the 1990s, this data conjured up images of a tree-lined residential street rather than a six-lane highway. “It was very analog,” he commented. “We’re talking about maybe 20 parameters that you’d need to check on a plan, and you’d put it all on paper. But I once calculated order of magnitude, and now we’re talking about 100,000 parameters. It’s simply not possible for a human to check.”
The group’s report, which was approved by the AAPM and the Science Council, reduces the number of parameters. It explains how data is transferred between various systems used in radiation therapy and suggests methods for medical physicists to test the data’s integrity throughout the process, resulting in safer treatments.