Normal aging progression Control in humans refers to changes in muscles, motor neurons, nerves, sensory functions, gait, fatigue, visual and manual responses in men and women who do not have a neurological, muscular (atrophy, dystrophy…), or neuromuscular disorder as they age. Neuromuscular movements become impaired with age, though some aspects can be avoided with training or practice.
One of the most distinguishing characteristics of humanity is the ability to communicate. The act of speaking is a highly complex cognitive and sensorimotor behavior. It starts with the desire to communicate and progresses to the conversion of the message into words, which are then converted into syllables, which must be ordered serially (i.e., sequenced) before articulation can begin.
Aging is a natural process of gradual change that begins in early adulthood. Many bodily functions begin to decline gradually in early middle age. People do not become old or elderly at a predetermined age. Traditionally, the age of 65 has been designated as the start of old age. But the reason was historical, not biological. Many years ago, the age of 65 was chosen as the retirement age in Germany, the first country to establish a retirement program. In the United States, the age of 65 was established as the eligibility age for Medicare insurance in 1965. This age is close to the average retirement age in economically advanced societies.
Force production
Action potentials occur in the cortex during voluntary force production. They spread throughout the spinal cord, motor neurons, and the muscle fibers they innervate. This causes a twitch, the properties of which are controlled by two mechanisms: motor unit recruitment and rate coding. Aging has an effect on both mechanisms. For example, the number of motor units may decrease, their size, i.e. the number of muscle fibers they innervate, may increase, and the frequency with which action potentials are triggered may decrease. As a result, force production in older adults is generally impaired.
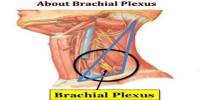
Muscle mass and strength loss are common as people age. These decreases could be attributed in part to the loss of alpha motor neurons. These losses occur in both proximal and distal muscles by the age of 70. In the biceps brachii and brachialis, old adults have a 1/3 decrease in strength, which correlates with a 1/2 decrease in the number of motor units. As motor units innervate collateral muscle fibers, remaining motor units in elderly people may grow larger.
In first dorsal interosseus, almost all motor units are recruited at moderate rate coding, leading to 30-40% of maximal voluntary contraction (MVC). Motor unit discharge rates measured at 50% MVC are not significantly different in the young subjects from those observed in the old adults. However, for the maximal effort contractions, there is an appreciable difference in discharge rates between the two age groups. Discharge rates obtained at 100% of MVC are 64% smaller in the old adults than in the young subjects: 31.1 ± 11.8 impulses/s in the old subjects, 50.9 ± 19.5 impulses/s in the young subjects.
When comparing old men to young men, isometric strength and physical cross-sectional area of the elbow flexors and extensors are reduced. The normalized force of the elbow extensors (maximal voluntary force to the size of the muscle producing the force) is the same in old and young people. The normalized force for the elbow flexors is lower in old men than in young men. The decrease in normalized elbow flexor force may be due to an increase in agonist-antagonist muscle coactivation.
In comparison to the young group, the elderly have lower dorsiflexor isometric torque at all angles and lower knee extensor isometric torque at angles greater than >90°. Muscle-specific force production impairment exists. During dynamic exercise, the old group requires more time to reach a target velocity and is less able to attain high velocities. The slowing of voluntary contractile speed with age seems to play a role in the loss of dynamic torque.