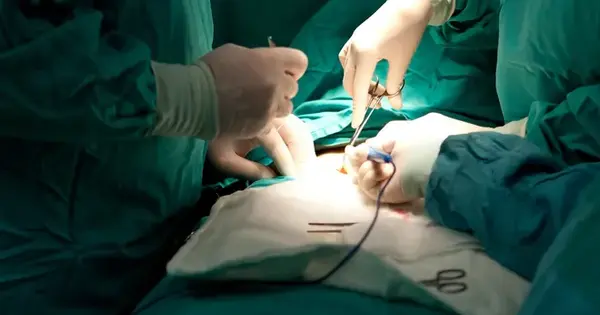
Obesity is a chronic disease that can lead to a variety of health issues such as diabetes, high blood pressure, and obstructive sleep apnea. Obesity may be difficult to treat because it affects so many organs. Weight-loss surgery can be an effective way to lose weight and keep it off when other medically supervised methods have failed.
Authorities on bariatric and metabolic surgery have issued new evidence-based clinical guidelines that, among other things, expand patient eligibility for weight-loss surgery and endorse metabolic surgery for patients with type 2 diabetes starting at a body mass index (BMI) of 30, a measure of body fat based on a person’s height and weight and one of several important screening criteria for surgery.
Two of the world’s foremost authorities on bariatric and metabolic surgery have issued new evidence-based clinical guidelines that, among other things, expand patient eligibility for weight-loss surgery and support metabolic surgery for patients with type 2 diabetes starting at a BMI of 30, a measure of body fat based on a person’s height and weight and one of several important screening criteria for surgery.
The ASMBS/IFSO Guidelines on Indications for Metabolic and Bariatric Surgery – 2022, published online in the journals Surgery for Obesity and Related Diseases (SOARD) and Obesity Surgery, are intended to replace a consensus statement developed more than 30 years ago by the National Institutes of Health (NIH) that set standards most insurers and doctors still rely on to make decisions about who should get weight-loss surgery, what kind, and when.
The ASMBS/IFSO Guidelines provide an important reset when it comes to the treatment of obesity. Insurers, policymakers, healthcare providers, and patients should pay close attention and work to remove the barriers and outdated thinking that prevent access to one of the safest, effective, and most studied operations in medicine.
Scott Shikora
The American Society for Metabolic and Bariatric Surgery (ASMBS) is the largest group of bariatric surgeons and integrated health professionals in the United States, and the International Federation for the Surgery of Obesity and Metabolic Disorders (IFSO) represents 72 national associations and societies worldwide.
“The 1991 NIH Consensus Statement on Bariatric Surgery served a valuable purpose for a time, but after more than three decades and hundreds of high-quality studies, including randomized clinical trials, it no longer reflects best practices and lacks relevance to today’s modern-day procedures and patient population,” said Teresa LaMasters, MD, President, ASMBS. “For the sake of patients, a shift in thinking and practice is required. It is long overdue.”
In the 1991 consensus statement, bariatric surgery was confined to patients with a BMI of at least 40 or a BMI of 35 or more and at least one obesity-related condition such as hypertension or heart disease. There were no references to metabolic surgery for diabetes or references to the emerging laparoscopic techniques and procedures that would become mainstay and make weight-loss surgery as safe or safer than common operations including gallbladder surgery, appendectomy, and knee replacement. The statement also recommended against surgery in children and adolescents even with BMIs over 40 because it had not been sufficiently studied.

New Patient Selection Standards – Times Have Changed
The ASMBS/IFSO Guidelinesnow recommend metabolic and bariatric surgery for individuals with a BMI of 35 or more “regardless of presence, absence, or severity of obesity-related conditions” and that it be considered for people with a BMI 30-34.9 and metabolic disease and in “appropriately selected children and adolescents.”
But even without metabolic disease, the guidelines say weight-loss surgery should be considered starting at BMI 30 for people who do not achieve substantial or durable weight loss or obesity disease-related improvement using nonsurgical methods. It was also recommended that obesity definitions using standard BMI thresholds be adjusted by population and that Asian individuals consider weight-loss surgery beginning at BMI 27.5.
Higher Levels of Safety and Effectiveness for Modern-Day Weight-Loss Surgery
The new guidelines further state “metabolic and bariatric surgery is currently the most effective evidence-based treatment for obesity across all BMI classes” and that “studies with long-term follow up, published in the decades following the 1991 NIH Consensus Statement, have consistently demonstrated that metabolic and bariatric surgery produces superior weight loss outcomes compared with non-operative treatments.”
It is also noted that multiple studies have shown significant improvement of metabolic disease and a decrease in overall mortality after surgery and that “older surgical operations have been replaced with safer and more effective operations.” Two laparoscopic procedures, sleeve gastrectomy and Roux-en-Y Gastric Bypass (RYGB), now account for about 90% of all operations performed worldwide.
Roughly 1 to 2% of the world’s eligible patient population get weight-loss surgery in any given year. Experts say the overly restrictive consensus statement from 1991 has contributed to the limited use of such a proven safe and effective treatment. Globally, more than 650 million adults had obesity in 2016, which is about 13% of the world’s adult population. CDC reports over 42% of Americans have obesity, the highest rate ever in the U.S.
“The ASMBS/IFSO Guidelines provide an important reset when it comes to the treatment of obesity,” said Scott Shikora, MD, President, IFSO. “Insurers, policymakers, healthcare providers, and patients should pay close attention and work to remove the barriers and outdated thinking that prevent access to one of the safest, effective, and most studied operations in medicine.”