Arsenic Poisoning
Arsenic poisoning, happens when a person takes in dangerous levels of arsenic. Arsenic is a natural semi-metallic chemical that is found all over the world in groundwater. It also exists in compounds that may be inorganic or organic.
Arsenic poisoning can cause major health complications and death if it is not treated, so precautions exist to protect those who are at risk. Arsenic is often implicated in deliberate poisoning attempts, but an individual can be exposed to arsenic through contaminated groundwater, infected soil and rock, and arsenic-preserved wood. However, arsenic in the environment is not immediately dangerous, and it is rare to find toxic amounts of arsenic in nature.
Sources: Sources of arsenic include:
- Pesticides
- Herbicides
- Fungicides
- Wood preservatives
- Ceramic enamels
- Paints
- Tobacco (there may be as much as 6 micrograms per pack)
- Burning of fossil fuels as arsenic is a contaminant
- From the diet, as organic arsenic from fish and seafood
- Illicit whiskey (moonshine) is a possible source of arsenic poisoning.
Occupational exposure can occur in:
- The smelting industry (arsenic is a by-product of ores containing lead, gold, zinc, cobalt and nickel)
- The microelectronics industry (as gallium arsenide)
- Coal power plants
- Jobs involving the manufacturing of glass and fireworks
- Jobs with contact with pesticides
- Jobs with contact with wood treated with arsenic as a preservative
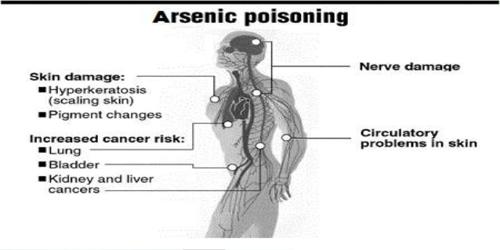
Symptoms and signs
- Arsenic exposure is usually occupational but can result from deliberate poisoning.
- Take a work history when a patient presents with painful peripheral neuropathy.
- Exposure to arsine gas is usually the result of an industrial accident and the worker presents rapidly with the fact.
- Unusual cases require a careful history regarding dietary and nutritional habits, hobbies, and alcohol abuse.
Causes
- Children may encounter arsenic trioxide as a rodenticide or herbicide. Examine for both arsenic and cholinesterase-inhibitor exposure. Possible transdermal absorption from exposure to pressure-treated wood, now banned for use by the US EPA, has been reported.
- Adults may be exposed through work in a metal foundry, mining, glass production, or the semiconductor industry.
- Arsenic has been found to contaminate such common items as wine, glues, and pigments.
Acute Poisoning
- Within 30 minutes of exposure there is a metallic taste in the mouth and slight odor of garlic in the breath along with dry mouth and dysphasia.
- This is followed abruptly by severe nausea and vomiting, colicky abdominal pain and profuse diarrhea, sometimes bloody with rice water stools.
- If a large amount has been ingested, cyanosis, cold clammy extremities, hypoxic encephalopathy, convulsions and acute tubular necrosis may occur following shock. Hyperpyrexia, pulmonary edema and acute hemolytic may also occur.
- With a smaller amount the patient will have severe headache, vertigo, periorbital edema, skeletal muscle cramping and evidence of renal damage manifested as oliguria, proteinuria, and haematuria.
- If death does not occur in the first few hours from shock, the patient may die a few days later from acute liver failure or renal failure.
- Cardiac manifestations include acute cardiomyopathy, subendocardial hemorrhages, and ECG changes of prolonged QT interval and non-specific ST and T wave changes. There is risk of ventricular fibrillation.
Chronic poisoning:
This is much more insidious and difficult to diagnose.
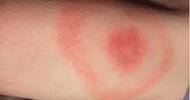
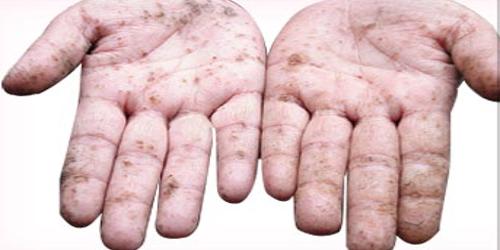
- The earliest skin lesions are persistent erythematous flushing. Hyperkeratosis follows with desquamation of the palms and soles, pigmentation changes, brittle nails with Mee’s lines, patchy or diffuse alopecia and edema of the face, periorbital region or ankles.
- Bowen’s disease is a long-term complication of chronic arsenic poisoning and is pre-malignant.
- Neuropathy is characteristic. It is usually a symmetrical sensory-motor polyneuropathy with paraesthesia, numbness, and pain, particularly of the soles of the feet. Eventually, muscular atrophy and ataxia are seen.
- Encephalopathy may occasionally occur, with severe headache, personality disturbance, convulsions or coma.
- Other features of chronic arsenic poisoning are nausea, vomiting, diarrhoea and irritability.
- There can be hepatic and renal damage.
Management
Non-Drug
- Once arsenic is in the tissues treatment may be to no avail, so efforts should be made to remove arsenic from the body before it reaches the tissues. Gastric lavage is used.
- Haemodialysis at an early stage can clear a substantial amount of arsenic.
- In the acute condition, blood and fluid loss will need replacement. Chelation therapy and haemodialysis should be implemented as soon as possible.
Drugs
- Dimercaprol is the first-line agent for treating arsenic poisoning. Other chelating agents are sometimes used.
- The results of treatment with vitamin E and selenium are unimpressive.5
- Pain may require strong analgesics.
Prevention
It is estimated that 29-77 million Bangladeshis i.e. 23 – 62 % of the 125 million populations are at risk of arsenic poisoning. According to some estimates, arsenic in drinking water will cause 5 million deaths in Bangladesh. The World Health Organization (WHO) has called it the “largest mass poisoning of a population in history”. Other countries including the USA, Mexico, China and Chile have discovered arsenic in their water supplies. Chronic arsenic poisoning is likely to become an international health issue and requires research and awareness worldwide. Exactly how arsenic gets into water-soluble form in groundwater remains controversial but some plants have the ability to remove arsenic from the environment.
Treatment:
Further Inpatient Care
- Many patients will develop profound peripheral motor palsies requiring extensive rehabilitation. Rehabilitation should be started as promptly as the clinical picture allows.
Further Outpatient Care
- Perform a careful neurological evaluation in follow-up of all patients because the peripheral neuropathy, which may develop after an acute exposure, may not appear for 2-3 weeks.
Information Source: