According to a recent study that was just published in the journal Stroke of the American Stroke Association, tenecteplase, a newer generation clot-busting medication, outperforms the conventional treatment for ischemic strokes in a number of crucial ways, including better health outcomes and lower costs.
The trial, which began in September 2019 at 10 Ascension Seton hospitals in Central Texas under the direction of a group of neurologists from Dell Medical School at The University of Texas at Austin, lasted 15 months.
“The Dell Med Neurology Stroke Program was one of the first in the United States to make this change,” said Steven Warach, M.D., lead author of the study and director of the Stroke Program for Dell Med and Ascension Texas.
“Based on even the earliest results from this study, other experts across the country were convinced and made the switch from alteplase to tenecteplase at their own stroke centers, including at Ascension hospitals nationwide.”
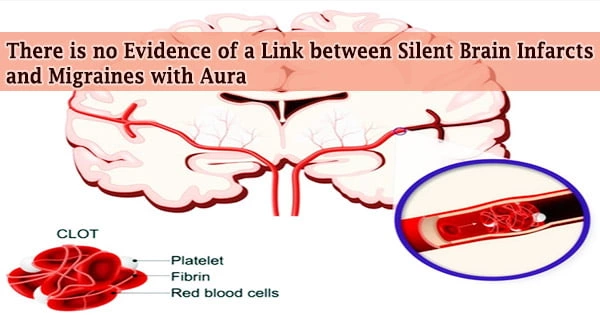
Every year, there are close to 800,000 strokes in the US. About 87 percent of such strokes are ischemic, meaning they happen when a blood clot obstructs a channel providing blood to the brain.
A comparable loss of neurologic function may follow from this. The use of tenecteplase and alteplase to dissolve clots in obstructed cardiac arteries has received governmental approval.
However, as it is more convenient to use and may be at least as effective as alteplase in treating ischemic strokes, the more recent medication tenecteplase is also being used off-label by doctors to treat these conditions.
The Dell Med Neurology Stroke Program was one of the first in the United States to make this change. Based on even the earliest results from this study, other experts across the country were convinced and made the switch from alteplase to tenecteplase at their own stroke centers, including at Ascension hospitals nationwide.
Steven Warach
Tenecteplase is injected intravenously once, lasting five to ten seconds. The conventional treatment for stroke, alteplase, which is administered slowly over 60 minutes, was compared to see how well it performed by the researchers.
“When it comes to treating patients with a stroke, every second matters,” said Warach, who is also a professor of neurology at Dell Med.
“The shorter preparation and injection time with tenecteplase not only eliminates a lot of dosing errors related to alteplase, but it’s also more efficient. We were able to deliver the clot-busting medicine more quickly after patients arrived in the emergency department, and for patients who needed to be transferred to another hospital for more advanced care after receiving the clot buster, we were able to initiate the transfer sooner in those treated with tenecteplase.”
According to Warach’s research, tenecteplase reduced the “door-to-needle” time for stroke patients who visit the emergency room by an average of six minutes from the time they arrive until they receive treatment.
The process of transferring patients to a stroke center equipped for thrombectomy was speed up by 25 minutes for patients who also needed a thrombectomy, which is the surgical removal of a blood clot that is the cause of the stroke.
Researchers also saw improvements in clinical outcomes for patients given tenecteplase, including:
- A 5% increase in patients who were able to walk independently at time of hospital discharge to home.
- A 4% decrease in occurrences of bad events such as brain hemorrhages, discharge to hospice care or death.
The third major improvement: cost. Tenecteplase treatment was discovered to be roughly $2,500 less expensive for the hospitals per patient than alteplase.
“If this price differential continues, the magnitude of savings could equate to in excess of $150 million every year in the U.S.,” said David Paydarfar, M.D., co-author of the study and chair of the Department of Neurology at Dell Med. “This is a great example of value-based care better care for less money.”
In order to spread the results of its study throughout the state and encourage more stroke centers to convert to tenecteplase, the Dell Med Neurology Stroke Program is currently collaborating with colleagues in the state-funded Lone Star Stroke Research Consortium.
Together with Lone Star Stroke partners, Warach is also creating a state-wide database to support their findings and address any unanswered problems.
“For example, we have such a large Latinx population in Texas. I’d like to know if we’re seeing the same advantages from tenecteplase in that community as we are in the larger population,” said Warach. “The more data we have, the more questions we can answer.”