MECHANISM OF BLADDER CONTROL:
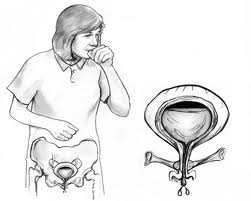
Three sets of muscles control urine. One set is the bladder muscle itself. The second set is sphincter muscles that open and close the urethra and the third set is the pelvic floor muscles. They support the uterus, rectum and the bladder. The bladder is the muscle that sits just under your pubic bone and is connected to the kidneys. The two tubes (ureters) bring urine made by the kidneys down to the bladder. The bladder has two main jobs:
- To store urine. Every time you eat or drink, your body absorbs liquids. The kidneys filter out waste products from the blood and make urine.
- To empty the urine out that it has stored or “to void”.
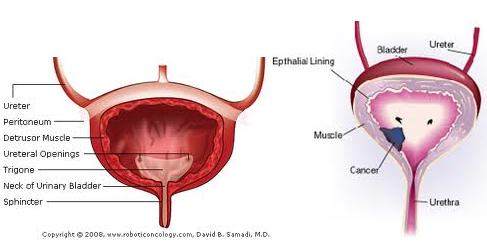
When the bladder is trying to store urine its job is to relax. The bladder is helped out with its storage function by two muscles, the internal sphincter and the external sphincter. These sphincters are muscles too and their job is to squeeze down tight to prevent loss of urine during storage. Pelvic floor muscles under the bladder also help keep the urethra closed. Urine stays inside the bladder when the sphincter and the pelvic floor muscles are tight. When the bladder is trying to empty urine its job is to contract and the sphincters help out here too by relaxing, allowing urine to pass through. Bladder control means you urinate only when you intend. For good bladder control, all parts of your system must work together. The pelvic muscles must hold up the bladder and the urethra. The sphincter muscles must open and shut the urethra and the nerves must control the muscles of the bladder and the pelvic floor.
The slight need to urinate is sensed when urine volume reaches about one half of the bladder’s capacity. When your bladder is full, nerves in your bladder signal the brain that it is full and you get the urge to go to the bathroom. Your brain sends signals through nerves in your spinal cord that tell the large bladder muscle called the detrusor (layered smooth muscle that surround the bladder) when to relax and when to contract. Once stimulated, the detrusor contracts into a funnel shape ready to expel the urine. The brain also helps to co-ordinate the bladder, the sphincters and pelvic floor muscles so that they are working together to relax and to let the urine through. So, conditions that affect brain function and spinal cord function often affect a person’s ability to control urination.
PSYCHOPATHOLOGY:
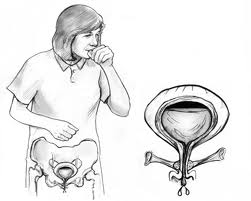
Stress incontinence is leakage with increases in intra-abdominal pressure that occur with coughing, sneezing, exercise or physical activity. Stress incontinence occurs when the urethra stops functioning as a sphincter maintaining urine in the bladder. The etiology of stress incontinence is multifactorial and poorly understood. It may be due to poor urethral support (Photo 1), neuromuscular damage to the urethra (Photo 2), or a combination of both (2).
Urge incontinence is defined as leakage when there is an urgent desire to void. Patients with urge incontinence free. The function of the lower urinary tract is storage and evacuation of urine. Incontinence is a disorder of the storage phase.Quently complains of leakage while running to the bathroom. This is usually caused by Detrusor Instability, which is the occurrence of involuntary, uninhibited bladder contractions. Urge incontinence is a part of the overactive bladder syndrome, which also includes patients with frequency, urgency (without leakage) and nocturia. This condition is most often idiopathic and probably due to the loss of normal neurologic inhibitory reflexes which suppress bladder muscle contraction during bladder filling. The prevalence of urge incontinence increases with aging. When uninhibited bladder contractions are caused by neurologic disease such as spinal cord tumors, multiple sclerosis or stroke, the diagnosis is Reflex Incontinence or Detrusor Hyperreflexia.
Mixed incontinence is a combination of stress and urge symptoms. Often, one symptom is much more bothersome to the patient than the other. An example would be the patient who has urge incontinence ten times per day and stress incontinence one time per month when her asthma flares up. In the initial evaluation it is important to identify which symptom is predominant and direct therapy towards treating that symptom.
Overflow incontinence is leakage associated with overdistention of the bladder. In this condition the detrusor muscle may be hypotonic or atonic. The bladder fills until it is unable to hold more urine and then leakage occurs “off the top”. This condition is relatively uncommon. It may be associated with diabetes, obstruction or neurologic conditions (neurogenic bladder). It is also associated with chronic bladder overdistention, the so-called “school-teacher’s bladder”.
Functional incontinence is leakage that occurs because of the physical inability to reach the toilet in a timely fashion. This often occurs at night in elderly people with severe musculoskeletal or vision deficits. There is no specific genitourinary pathophysiology associated with this condition. It is often cured with a bedside commode
- Mortality/Morbidity:
Urinary incontinence is not associated with increased mortality. The medical morbidity includes perineal candidal infection, cellulitis, pressure sores, constant skin irritation and moisture, urosepsis from indwelling catheters, falls and fractures from slipping on urine, and sleep deprivation from nocturia. Psychological morbidity includes poor self-esteem, social withdrawal, depression, sexual dysfunction from embarrassment, and curtailed social and recreational activities.
- Race:
Stress incontinence is more prevalent in Caucasian women than in African American or Hispanic women (41% vs 31% vs 30%, respectively). The incidence of urge incontinence is similar in all 3 groups (19% vs 16% vs 16%, respectively). Mixed incontinence occurs more often in African American and Caucasian women compared with Hispanic women (14% vs 15% vs 0.9%, respectively).
- Sex:
Overall, rates in men are approximately one third of those in women until age 80 years when the rates converge.
- Age:
Age is a risk factor for UI. Older individuals may have medical conditions that impair continence. This may include diabetes, medications, mental status change, declining lower urinary tract function, alteration in volume status and urine excretion, and functional impairment of toileting ability.
Urinary incontinence is caused by disturbance in the storage function, and occasionally in the emptying function, of the lower urinary tract. Urethral sphincter dysfunction and bladder dysfunction could coexist in some individuals, and insistence that patients fit into only one category might compromise their clinical care. For example, a woman might be unaware of detrusor contractions, as long as these can be easily suppressed and do not result in incontinence. However, after damage to the urethral sphincter (such as during vaginal delivery), the same amount of detrusor overactivity could become symptomatic with urge incontinence.
Another important concept is that women may undergo an anatomical or neuromuscular injury during childbirth but remain clinically asymptomatic as long as there is compensation by other components of the continence mechanism. After childbirth trauma and loss of the pelvic floor muscles, a woman might not have incontinence until she loses a small percentage of muscle strength and innervation to the urethral sphincter because of aging or other injuries, and that small loss could alter the balance in favour of urinary incontinence instead of continence. Much of what is known about the incontinent state derives from the study of patients in the late (decompensated) stages of the condition.
CLINICAL FEATURES
Symptoms include:
- leakage of urine during exercise, laughing, coughing, sneezing, or lifting.
- urine leaks in frequent dribbles.
- inability to hold urine long enough to get to the toilet.
- urine continues to dribble after urinating.
- smell of urine on clothes and in the house.
The following are the most common symptoms of urinary incontinence. However, each individual may experience symptoms differently. Symptoms may include:
- Inability to urinate.
- Pain related to filling the bladder and/or pain related to urination without a proven bladder infection.
- Progressive weakness of the urinary stream with or without a feeling of incomplete bladder emptying.
- An increased rate of urination without a proven bladder infection.
- Needing to rush to the restroom and/or losing urine if you do not get to restroom in time.
- Abnormal urination or changes in urination related to a nervous system.
- Abnormality such as stroke, spinal cord injury, multiple sclerosis.
- Leakage of urine that prevents activities.
- Leakage of urine that began or continued after surgery.
- Leakage of urine that causes embarrassment.
- Frequent bladder infections.
The symptoms of urinary incontinence may resemble other conditions or medical problems. Always consult your physician for a diagnosis.Other symptoms of a kidney infection include pain in the back or side below the ribs, nausea, or vomiting.
| Symptom | Sign | Urodynamic diagnosis | |
| Stress urinary incontinence | Involuntary loss of urine, with effort or exertion, or on sneezing or with exertion or effort, or on sneezing or coughing. | Involuntary leakage from the urethra with exertion or effort, or on sneezing or coughing. | Involuntary leakage of urine shown during raised abdominal pressure, in the absence of acoughing or coughing detrusor contraction is referred to as urodynamic stress incontinence. |
| Bladder neck hypermobility | Involuntary loss of urine, with effortor exertion, or on sneezing or coughing. | Hypermobile bladder neck on Q-tip*or other objective measure. | High valsalva leak point pressure or high maximum urethral closure pressures |
| Intrinsic sphincter deficiency | Involuntary loss of urine, with effort or exertion, or on sneezing or coughing. | Bladder neck could be raised orHypermobile. | Low valsalva leak point pressure or low maximum urethral closure pressure. |
| Urge urinary incontinence | Involuntary leakage accompanied by or immediately preceded by urgency. | Urine leakage seen during examination frboym the urethra associated with urgency. | Incontinence due to an involuntary detrusor contraction usually with a sensation urgue, is known as detrusor overactivity incontinence. |
PREVENTION:
One may not be able to prevent urinary incontinence because it is a symptom of several other problems, rather than a condition with a single cause. This is why it is important to discuss incontinence with your health care provider.
Many people may benefit from exercises known as Kegel exercises that strengthen the pelvic floor muscles. You can feel the muscles to use by squeezing the muscles in your genital area. You might find that it helps to pretend you are stopping a flow of urine or trying to stop from passing gas.
- Tighten these muscles and hold the contraction for 4 seconds. Do this 10 to 20 times. Allow the muscles to relax completely between contractions.
- Do these sets of contractions 10 times a day. Doing fewer repetitions than this will make the exercises less effective.
- You can do Kegel exercises anywhere: while sitting at a desk, waiting for a bus, washing dishes, driving a car, waiting in line, or watching television. No one will know you are doing them.
- Do not do these exercises while you are urinating.
One may see a change for the better after doing the Kegels for just a few weeks. However, you may not notice a lot of improvement until after 3 to 6 months of daily exercises. You should continue doing Kegels every day to keep the pelvic muscles strong.
If you have urge incontinence, bladder training can make a big difference. Instead of waiting for your bladder to signal the need to urinate (which is too late for many people), set a schedule for emptying your bladder. Use the toilet 20 to 30 minutes after each meal, at least twice between meals, and before you go to bed. You can set a timer to remind you. Adjust the schedule as you learn the frequency that best meets your needs.
Overflow incontinence is caused by an enlarged prostate, which is common in older men. It can sometimes be prevented by medicine when early symptoms of prostate enlargement, such as frequent urination, appear.
One stay within easy reach of a bathroom. Have a night-light in your bathroom. Don’t try to hold your urine, and be willing to ask where the toilet is when you are away from home.
Drink plenty of fluids. Don’t try to control urinary incontinence by cutting back on fluids. It won’t help and may even be harmful to her.
Prevention for urinary incontinence can include:
- Kegel exercises to strengthen weak pelvic muscles. The muscles can also be tightened by surgery.
- Medicine that tightens the urethral muscle, stimulates the bladder to empty, relaxes an irritable bladder, or treats infection.
- Medication. Estrogen hormone replacement therapy can help improve pelvic muscle tone in postmenopausal women. Anticholinergics (i.e., propantheline, or Pro-Banthine) and antispasmodics (i.e., oxybutynin, or Ditropan) are sometimes prescribed to relax the bladder muscles. Other over-the-counter medications such as pseudoephedrine (i.e., Actifed, Benadryl, Dimetapp) and phenylpropanolamine (i.e., Dexatrim, Acutrim) may be prescribed to tighten the urethral sphincter.
- Bladder training, which teaches you to empty the bladder on schedule rather than waiting until you feel the urge.
- A pessary, which is similar to the outer ring of a diaphragm. This is inserted up around a woman’s cervix, where it gives support to the pelvic muscles and helps prevent stress incontinence. Your health care provider may advise a pessary to support lax pelvic muscles if this is contributing to the incontinence.
- Incontinence pads, available in all sizes and degrees of absorbency, to decrease chances of accidents.
- A collecting device fitted over the male penis to hold urine.
- Catheters inserted into the bladder so that it can be mechanically drained on schedule. This is usually done only as a last resort.
- Intermittent urinary catheterization. The periodic insertion of a catheter into a patient’s bladder to drain urine from the bladder into an attached bag or container.
- Permanent catheterization. A permanent, or indwelling, catheter may be prescribed for chronic incontinence that doesn’t respond to other treatments. A Foley catheter is usually used for urinary catheterization. One end is inserted through the urethra and into the bladder, and the external end is attached to a plastic reservoir bag that the patient may wear on the leg. A second alternative is a permanent catheter, called a suprapubic tube, surgically inserted into the bladder. The tube exits the body through the abdomen near the pubic bone, where it is attached to a drainage bag. As infection may result, this treatment should be reevaluated periodically, and the possibility of alternative treatment addressed.
- Surgery. Bladder neck suspension surgery is used to correct female urinary stress incontinence. Surgical techniques such as the Marshall-Marchetti-Krantz and Burch procedures use sutures to raise and support the bladder neck and urethra. A sling procedure, which uses a strip of biocompatible material or the patient’s own muscle or tissue as a supportive sling under the urethra and bladder neck, may also be used to treat stress incontinence. Bladder enlargement surgery may be recommended to treat incontinent men and women with unusually small bladders.
- Bladder training. Used to treat urge incontinence, bladder training involves placing a patient on a toileting schedule. The time interval between urination is then gradually increased until an acceptable time period between bathroom breaks is consistently achieved.
- Pelvic toning exercises. Exercises to tone the pelvic muscle can help alleviate stress incontinence in both men and women. These exercises involve tightening the muscles of the pelvic floor, and are also known as Kegel or PC muscle exercises.
- Biofeedback. The use of sensors to monitor temperature and muscle contractions in the vagina to help incontinent patients learn to control their pelvic muscles.
- Collagen injections. Collagen injected in the tissue surrounding the urethra can provide urethral support for women suffering from stress incontinence.
- Inflatable urethral insert. Sold under the tradename Reliance, this disposable incontinence balloon for women is inserted into the urethra and inflated to prevent urine leakage.
- Perineal stimulation. Perineal stimulation is used to treat stress incontinence. The treatment uses a probe to deliver a painless electrical current to the perineal area muscles. The current tones the muscle by contracting it.
- Urinary sphincter implant. An artificial urinary sphincter may be used to treat incontinence in men and women with urinary sphincter impairment.
- Vaginal inserts. Devices constructed of silicone or other pliable materials that can be inserted into a woman’s vagina to support the urethra.
Kegel or PC muscle exercises. Women who arvve pregnant or who have gone through childbirth can reduce their risk for stress incontinence by strengthening their perineal area muscles with Kegel exercises. Men who have undergone prostate surgery may also benefit from pelvic muscle exercises. Men and women should consult with their doctor before initiating any type of exercise program.
EVALUATION
The basic evaluation of women with incontinence should include a detailed history, physical exam, pelvic exam, post void residual (PVR), UA, C&S, and voiding diary.
Because urinary incontinence is a quality of life issue rather than a life-threatening problem, the history should focus on impact on quality of life and severity of symptoms. The patient should be questioned regarding age of onset, number of pads or diapers per day, number of leaks per day and the need to alter daily activities. Stress and urge incontinence symptoms are differentiated by asking whether the leakage occurs with cough, sneeze or laugh versus leakage with urgency. Transient causes of incontinence should be ruled out .Incontinence tends to be a chronic problem so transient causes such as urinary tract infection should be suspected if the patient describes a recent onset of symptoms.
Other important factors to assess are daytime urinary frequency, nocturia, voiding difficulties, fluid intake and diet, mobility, history of recurrent urinary tract infection, constipation, and chronic cough.
The physical exam includes an evaluation for systemic disease and causes of increased intra-abdominal pressure such as obesity and COPD. Pelvic examination is performed initially with a full bladder. The patient is asked to cough or valsalva and the presence of stress incontinence is documented. PVR is checked by catheterization or bladder ultrasound. The PVR measurement at the initial evaluation is important, as this may be the only way to rule out overflow incontinence. Urethral hypermobility is assessed by examining the movement of the urethra with cough .A split vaginal speculum is used to assess concurrent prolapse of the anterior and posterior vaginal walls. The examiner then performs a digital vaginal exam to assess the strength of the pelvic floor muscles. A finger is placed at 4 and then 8 o’clock inside the vaginal opening along the pelvic sidewall. The patient is asked to contract the pelvic floor muscles. Patients who are unable to contract these muscles may not be good candidates for routine pelvic floor exercises (Kegel’s). Finally, a rectal exam is performed to rule out fecal impaction and to assess sphincter tone.
Further evaluation:
- Uncertain diagnosis
- Failure to respond to prior treatment
- Surgical candidate
- Hematuria without infection
- Recurrent UTI
- Voiding disorder
- Prior surgery
- Symptomatic and severe pelvic organ prolapse
- Abnormal PVR
- Neurologic abnormality
PHYSIOTHERAPY MANAGEMENT
TRANSVERSE ABDOMINIS EXERCISES
Transverse Abdominal Exercise – Plank Pose
This abdominal exercise is a simple move but really works the transverse abdominal muscle. It is all about holding your position in order to strengthen this muscle. These types of exercises where you hold the position are called isometric exercises and are great for strengthening and toning.
How to do the Plank Pose
- Place the elbows on the floor underneath the shoulders.
- Now place toes on the floor with legs hip width apart.

- With back straight, lift body off the floor and pull in belly button towards spine
- Hold this position for a count of 30 to 60 seconds.
- Relax placing body back on the floor and then repeat for 3 to 5 repetitions.
Transverse Abdominal Exercise – Plank Pose Leg Lift
This is a variation of the plank pose but adds additional challenge with the leg lift. Although the plank pose is isometric, this move is a combination of isometric exercise and a moving exercise as you are lifting and then holding the position.
How to do the Plank Pose Leg Lift
- Start in plank position as described above.
- Lift right leg off the ground about 6 to 8 inches while pulling belly button towards spine and hold for a count of 30 seconds.

- For more body toning, squeeze glutes, the butt, while doing this move.
- Return to plank position and repeat lifting the left leg this time.
- Repeat this on each side for 3 to 5 repetitions
Transverse Abdominal Exercise – Plank Pose Leg Lift
This is a variation of the plank pose but adds additional challenge with the leg lift. Although the plank pose is isometric, this move is a combination of isometric exercise and a moving exercise as you are lifting and then holding the position.
How to do the Plank Pose Leg Lift
- Start in plank position as described above.
- Lift right leg off the ground about 6 to 8 inches while pulling in belly button towards spine and hold for a count of 30 seconds.
For more body toning, squeeze glutes, the butt, while doing this move.

- Return to plank position and repeat lifting the left leg this time.
- Repeat this on each side for 3 to 5 repetitions.
Transverse Abdominal Exercise – Plank Pose Twist
This is one of the few abdominal exercises that work not only your transverse abdominis muscle but also the oblique muscles. It is of course a slight variation, a twist on the typical plank pose.
How to do the Plank Pose Twist
- Start in plank pose position.
- Lifting right leg and bending at the knee, twist slightly at the trunk and reach knee towards your hip.
- Return to plank pose position and repeat with other leg.
- Repeat this move on left side for 8 to 15 repetitions.

Transverse Abdominal Exercise – Transverse Pull Ins
This abdominal exercise is very difficult to illustrate as the movement is so small it is hard to tell the difference from start to finish position. Although the move is small it reaches deep down to the transverse abdominal muscle.
How to do the Transverse Pull Ins
- Lie on the floor with back flat, knees bent and feet on the floor.
- Place hands on lower abs, about where the bikini would cover, and place thumbs touching the naval.

- Now pretend like have to zip up a really tight pair of jeans and pull belly button towards the back of spine.
- Hold for 30 to 60 seconds then relax and repeat for several more times.
Note: To do this exercise in a standing position, just repeat the steps above while standing, being sure to keep the rest of the body relaxed and focus on the transverse abdominis to do the work.
Transverse Abdominal Exercise – Back Extensions
This is not really an abdominal exercise as much as it is a back stretching exercise. However after any ab exercise routine you should stretch not only abdominal muscles but also opposing back muscles.
How to do the Back Extensions
- Lie on stomach with arms straight out in front of palms facing down.
- Now lift upper body stretching transverse abdominis muscle and back muscles.

- For additional stretching, lift up upper and lower body at the same time for this exercise.
- Hold for 30 seconds, relax and then repeat several times.
SWISS BALL EXERCISES
(ABDOMINALS)

KEGELS EXERCISE
- To locate the right muscles, try stopping or slowing your urine flow without using your stomach, leg or buttock muscles. When you’re able to slow or stop the stream of urine, you’ve located the right muscles.
- Squeeze your muscles. Hold for a count of 10. Relax for a count of 10.
- Do this 20 times, 3 to 4 times a day.
- You may need to start slower, perhaps squeezing and relaxing your muscles for 4 seconds each and doing this 10 times, 3 or 4 times a day. Work your way up from there.

As a Physiotherapy & Yoga instructor knows a great deal about pelvic floor muscles and found that she was able to control her urge to urinate through a unique technique she developed that works those muscles. Today, Nett is proud to say she’s no longer has to worry about dashing to the nearest bathroom and worrying about every little cough and giggle.
Enhancing Sex & Kegel Exercises:
The Kegelmaster offers women a way to rapidly improve vaginal muscle strength and tone. By doing so, women have experienced great sexual benefits by adding resistance to simple kegel exercises. Some women have reported being able to have an orgasm after having years of difficulties. Other women have stated that after the first use of the Kegelmaster they were able to have more intense orgasms. Although women have said they are having stronger more satisfying orgasms, they are also saying they are easily having multiple orgasms.
By adding progressive dynamic resistance to Kegel exercises, women have used the Kegelmaster to strengthen the vaginal walls and tone the muscles responsible for such orgasms.
Exercises of pelvic muscle :
Kegel exercises to strengthen or retrain pelvic floor muscles and sphincter muscles can reduce or cure bladder leakage. Men and Women of all ages can learn and practice these exercises as effective urinary incontinence treatment, which are taught by a health care professional. Most Kegel exercises do not require equipment. However, one technique involves the use of weighted cones. For this exercise, the patient stands and holds a cone-shaped object within her vagina. As the patient becomes accustomed to the weight, cones of increasing weight are substituted to strengthen the muscles that help keep the urethra closed.
Electrical stimulation:
Brief doses of electrical stimulation can strengthen muscles in the lower pelvis in a way similar to exercising the muscles. Electrodes are temporarily placed in the vagina or rectum to stimulate nearby muscles. This will stabilize overactive muscles and stimulate contraction of urethral muscles. Electrical stimulation can be used to reduce both stress and urge urinary incontinence. Neuromuscular Electrical Stimulation (NMES) treatments retrain and strengthen urinary muscles and improve bladder control used with men and women. Electrical stimulation if the nerve in the pelvic floor is performed causing the urethral sphincter muscles to contract.
Biofeedback:
Biofeedback uses measuring devices to help you become aware of your body’s functioning. By using electronic devices or diaries to track when your bladder and urethral muscles contract, you can gain control over these muscles. Biofeedback can be used with pelvic muscle exercises and electrical stimulation as an effective urinary incontinence treatment.
Timed voiding or bladder training:
Timed voiding (urinating) and bladder training are techniques that use biofeedback. In timed voiding, you fill in a chart of voiding and leaking. From the patterns that appear in your chart, you can plan to empty your bladder before you would otherwise leak. Biofeedback and muscle conditioning–known as bladder training–can alter the bladder’s schedule for storing and emptying urine. These techniques are effective for urge and overflow urinary incontinence.
Bladder training:
Some people with urge incontinence can learn to lengthen the time between urges to go to the bathroom. You start by urinating at set intervals, such as every 30 minutes to 2 hours–whether you feel the need to go or not. Then gradually lengthen the time between when you urinate–say by 30 minutes–until you’re urinating every 3 to 4 hours.
One can practice relaxation techniques when you feel the urge to urinate before your time is up. Breathe slowly and deeply. Think about your breathing until the urge goes away. You can also do Kegel exercises if they help control your urge.
After the urge passes, wait 5 minutes and then go to the bathroom even if you don’t feel you need to go. If you don’t go, you might not be able to control your next urge. When it’s easy to wait 5 minutes after an urge, begin waiting 10 minutes. Bladder training may take 3 to 12 weeks.
NeoControl therapy:
It is beneficial for women with stress, urge or mixed urinary incontinence caused by weak pelvic floor muscles. The treatment is delivered through pulsating magnetic fields in a chair.
Urge Incontinence/Overactive Bladder:
Bladder training is a behavioral treatment that aims to lengthen the voiding interval such that bladder control is reestablished and the voiding reflex can be suppressed. The patient is given a voiding diary and the voiding habits are analyzed. Based on the diary she is begun on a voiding schedule. For instance, if she is currently suffering from frequency and urgency every 30 minutes she is placed on a schedule where she is to void every hour on the hour. She is not allowed to void at other times and is taught urge suppression techniques. When she is able to maintain her initial schedule with no leakage between voids, the interval is increased until she is voiding every 3 to 4 hours. The program may take several months and only works with a motivated patient. The patient must return to the office on a regular basis at which time the diary is reviewed, suppression techniques are retaught and the patient is given positive reinforcement. In one study, bladder training was 44-97% successful in the treatment of overactive bladder.
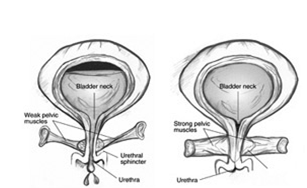
FRONT VIEW OF BLADDER. WEAK PELVIC MUSCLES ALLOW URINE LEAKAGE (LEFT). STRONG PELVIC MUSCLES KEEP THE URETHRA CLOSED (RIGHT).
Pelvic floor muscle exercise (Kegel’s) and biofeedback are behavioral techniques used for overactive bladder. Contraction of the pelvic floor muscles is known to reflexively cause relaxation of the bladder. In fact, the normal mechanism used to suppress urinary urgency is the initiation of a voluntary pelvic floor contraction. With pelvic floor exercise the patient can be taught to voluntarily contract the pelvic floor muscles thereby suppressing the micturition reflex and bladder contractions. Thirty per cent of women are unable to voluntarily contract the pelvic floor muscles and in these women biofeedback is used.
Biofeedback is a behavioral technique in which information about a normally unconscious physiologic process is presented to the patient as a visual, auditory or tactile signal. A vaginal probe sensor is placed and the patient is able to observe pelvic floor muscle activity on a computer screen. She is then taught how to initiate and control muscle contraction. Biofeedback is a very successful technique, which requires a committed patient. The program takes 6 to 8 weeks.
Urge incontinence/Overactive bladder is most successfully treatment through a combination of behavioral techniques and medications. Frequently, after a successful program of behavioral modification, the medications can be stopped.
Stress Incontinence:
Pelvic floor exercises (Kegel’s) can be very effective therapy for stress incontinence. The pelvic floor is composed of skeletal muscle which hypertrophies with use and atrophies with disuse. Therefore, exercise is only effective if done on a regular, continual basis. The patient is taught to contract the pelvic floor muscles and then placed on a regular schedule of 30 – 100 contractions per day. In general, the success of this technique depends on patient motivation, compliance, and long-term commitment.
Historically, the educational effort in teaching pelvic floor exercises has been poor. Often the patient is simply handed a sheet of directions. Simple written or verbal instruction have been shown to be inadequate and even with intensive individual instruction 30% of patients are unable to do Kegel exercises. A successful program includes hands-on instruction, supervision, monitoring and feedback. It often involves nurses, physical therapists and other health care providers. In the setting of an organized program many studies have shown significant improvement in stress incontinence symptoms.
Biofeedback and functional electrical stimulation may be used in conjunction with the pelvic floor exercise training program. These are particularly effective for those patients who are unable to voluntarily initiate a pelvic floor contraction.
Mechanical devices such as pessaries, urethral plugs, and urethral patches have also been occasionally used for stress incontinence however there is little data to support their efficacy.
- Talk with your health care provider if you begin to have problems with bladder control. Follow his or her advice for correcting or managing your incontinence.
- Limit drinking of carbonated, caffeinated, or alcoholic beverages.
- Decrease the amounts of tomatoes, fruit juices, dairy products, spicy foods, sugar, and artificial sweeteners in your diet. These foods in larger quantities can irritate the bladder.
- Drink plenty of fluids. Don’t try to control urinary incontinence by cutting back on fluids. It won’t help and may even be harmful to you.
- Drink liquids throughout waking hours, but limit fluids 3 hours before usual bedtime. Be sure to empty your bladder every 2 to 4 hours and before going to bed.
- If you have stress incontinence, do Kegel exercises regularly.
- Train your bladder as far as possible to empty on a regular schedule.
- Use incontinence pads to prevent wetting of clothing. Be sure to change the pads regularly.
- Keep your groin area as clean and as dry as possible.
Behavioral techniques sometimes include the following:
- Scheduling Toileting – The caregiver prompts the incontinent patient to go to the bathroom every two to four hours. This puts the patient on a regular voiding schedule. The goal is simply to keep the patient dry and is a frequently recommended therapy for frail, elderly, bedridden or Alzheimer’s patients.
- Bladder Re-training – Bladder retraining involves scheduled toileting but the length of time between bathroom trips is gradually increased. This therapy trains the bladder to delay voiding for larger time intervals and has been proven effective in treating urge and mixed incontinence.
- Pelvic Muscle Rehabilitation – This technique involves pelvic muscle exercises (PME). PME may be used alone or in conjunction with biofeedback therapy, vaginal weight training, pelvic floor stimulation, and magnetic therapy.
Other measures include:
- Regulate your bowels to avoid constipation. Try increasing fiber in your diet.
- Quit smoking to reduce coughing and bladder irritation. Smoking also increases your risk of bladder cancer.
- Avoid alcohol and caffeinated beverages, particularly coffee, which can overstimulate your bladder.
- Lose weight if you need to.
- Avoid foods and drinks that may irritate your bladder like spicy foods, carbonated beverages, and citrus fruits and juices.
- Keep blood sugars under good control if you have diabetes.
PT is effective:
It is effective because the focus is hands on treatment of a condition most commonly caused by muscle weakness and it addresses the pelvic floor muscles which are prone to be forgotten in exercise training in general.
Women should think of these exercises as a lifelong endeavor but not something that is overwhelming. They can be performed in multiple positions, lying down, sitting, or standing. They can even be done with others around without them realizing that one is exercising. It is recommended that patients contract for at least 3 seconds and relax the muscles for the same period of time in sets of 10-15 several times per day, ideally at least 3 times in different body positions reflecting how these muscles need to function in the real world. Patients are instructed to think of these exercises as a daily activity similar to brushing their teeth.
Patients are the best candidates for physical therapy:
Physical therapy has been found to be effective in all types of incontinence, stress, urge, mixed, and in fecal incontinence as well.
Patients who have had complete nerve injury to the muscles such as in the case of spinal cord injury may not be good candidates, however, physical therapy can sometimes even help those with incomplete neural injury.
REHABILITATION
Pelvic Floor Rehabilitation:
The Pelvic Floor Rehabilitation Program is designed for children who continue to have episodes of daytime urinary leaks beyond the typical age of potty training. After a thorough work up by a pediatric urologist, your child would be referred to an All Children’s Hospital Outpatient Physical/Occupational Therapy Department for pelvic floor rehabilitation.
The Physical and Occupational Therapists are thoroughly educated in the anatomy and physiology of the urinary tract system and the musculoskeletal system as well as child development. They are trained in the use of the computer system and the process for pelvic floor rehabilitation to best assist your child.
The pediatric physical therapists and occupational therapists work closely with you, your child and the physicians to progress your child towards success.
Pelvic Floor Rehabilitation:
Pelvic Floor Rehabilitation works to strengthen and coordinate the muscles that control the bladder. This program also educates you and your child on anatomy of the urinary tract system and strategies to avoid urinary leaks.
During treatment sessions:
At each of the appointments, homework will be reviewed and practiced, education will be given regarding that week’s activities and your child will be connected to the computer as they were during the evaluation. Your child will perform a variety of pelvic floor muscle exercises while the computer gives visual feedback, which helps to motivate your child to work these muscles.
Treatment and evaluation may be painfull:
The pelvic floor rehabilitation program is not painful. The electrodes are gel based and go on and off easily.
The goal of the pelvic floor program is for each child to improve and/or achieve independent bladder control. Your child will gain knowledge of their urinary tract system and diet related issues. They will also gain improved self-esteem, confidence and the increased ability to participate in social activities such as sleep-overs.
The following methods are used to strengthen the muscles of pelvic floor:
- Bladder retraining — this involves urinating on a schedule, whether you feel a need to go or not. In between those times, you try to wait to the next scheduled time. At first, you may need to schedule 1 hour intervals. Gradually, you can increase by 1/2 hour intervals until you are only urinating every 3-4 hours without leakage.
- Kegel exercises — contract the pelvic floor muscles for 10 seconds, then relax them for 10 seconds. Repeat 10 times. Do these exercises 3 times per day. You can do Kegel exercises any time, any place.

To find the pelvic muscles when you first start Kegel exercises, stop urine flow midstream. The muscles needed to do this are your pelvic floor muscles. DO NOT contract abdominal, thigh, or buttocks muscles. And DO NOT overdo the exercises. This may tire the muscles out and actually worsen incontinence.
Two methods called biofeedback and electrical stimulation can help to learn how to perform Kegel exercises. Biofeedback uses electrodes placed on the pelvic floor muscles, giving you feedback about when they are contracted and when they are not. Electrical stimulation uses low-voltage electric current to stimulate the pelvic floor muscles. It can be done at home or at a clinic for 20 minutes every 1 to 4 days.
Biofeedback and electrical stimulation will no longer be necessary once you have identified the pelvic floor muscles and mastered the exercises on your own.
Vaginal cones enhance the performance of Kegel exercises for women. Other devices for incontinence are also available.
For leakage, wear absorbent pads or undergarments. There are many well-designed products that go completely unnoticed by anyone but you.
- Diet:
Proper nutrition is important to controlling your incontinence and maintaining good health. It’s important to remember that many foods and beverages can irritate the bladder including alcohol, caffeine, acidic fruits or fruit juices, tomato or tomato-based products, milk products, artificial sweeteners and spicy foods.
Monitor Fluids:
Do not restrict fluids as a means to control your incontinence. Restricting fluids may be dangerous and could aggravate the problem. Decreased fluids can lead to constipation, which could contribute to incontinence, cause dehydration or make the urine concentrated, which can irritate the bladder.
It is recommended that you drink at least 50 ounces (six to seven 8-ounce glasses) of fluids spread throughout the day, as large volumes at one time can fill the bladder too quickly and lead to urgency. Fluid intake can be reduced after dinner to prevent nighttime accidents.
Weight Loss:
Excessive weight can also contribute to incontinence by adding pressure to the abdominal area. Research indicates a five to 10 percent weight loss in individuals who are overweight may decrease urine leakage.
Absorbent Products:
Millions of people use absorbent products to help maintain a normal lifestyle. There is a wide variety of absorbent products available for both short-term and long-term use. To help select a product that’s right for you, visit the “Our Products” section at depend.
Other measures include:
- Regulate your bowels to avoid constipation. Try increasing fiber in your diet.
- Quit smoking to reduce coughing and bladder irritation. Smoking also increases your risk of bladder cancer.
- Avoid alcohol and caffeinated beverages, particularly coffee, which can overstimulate your bladder.
- Avoid foods and drinks that may irritate your bladder like spicy foods, carbonated beverages, and citrus fruits and juices.
Electrical stimulation therapy, which targets involved muscles with low-current electricity, can be used to treat either urinary or fecal incontinence. Biofeedback uses electronic or mechanical devices to improve bladder or bowel control by teaching an individual how to recognize and respond to certain body signals.
Embarrassment may lead some people to manage the symptoms of incontinence themselves by wearing absorbent pads to prevent the soiling of their clothes. However, many treatments exist to successfully restore or improve control of bowel and bladder function, so individuals experiencing incontinence should speak to a doctor or nurse.
CONCLUSION
Female urinary incontinence continues to be a major healthcare problem. The prevalence of incontinence increases with aging; however, incontinence should not be considered a normal part of aging. Most patients can be cured or significantly improved with non-surgical or surgical therapy. All patients deserve a complete evaluation and discussion of the many treatment options.
Some men must contend with urinary incontinence following surgery. This problem can greatly interfere with ones quality of life and can be a tremendous inconvenience for those who are working, traveling or engaging in social activities.
Therapists are trained to treat urinary incontinence using a combination of biofeedback and kegel exercise that specifically targets the muscles of the pelvic floor which may be affected during surgery.
BIBLIOGRAPHY
http://www.gmail.com
http://www.tue.com
http://www.asahi-net.or.jp/~uy7t-wtnb/help/trouble/
http://www.yahoo.com
http://www.google.com
http://www.opera.com http://www.pis.or.jp/medical.htm
http://www.pis.or.jp/iryou/index.htm
http://www.healthnetworkamerica.com/
http://www.patientadvocatesllc.com
http://www.Healthcare.com
http://www.Medical Marketing Tips.com
http://www.Medical Copywriting.com
http://www.Medical Clients Served.com
http://www.lopnor.gr.jp/data/tobu_f_organization/.
REFERENCES:
1. Corcos J, Beaulieu S, Donovan J, Naughton M, Gotoh M. Quality of life assessment in men and women with urinary incontinence. J Urol 2002; 168: 896–905.
2. Wilson L, Brown JS, Shin GP, Luc KO, Subak LL. Annual direct cost of urinary incontinence. Obstet Gynecol 2001; 98: 398–406.
3. Andersson KE. Detrusor contraction—focus on muscarinic receptors. Scand J Urol Nephrol Suppl 2004; 215: 54–57.
4. Luxem M, Christophersen E. Behavioral toilet training in early childhood: research, practice, and implications. J Dev Behav Pediatr
1994; 15: 370–78.
5. DeLancey JO. Structural support of the urethra as it relates to stress urinary incontinence: the hammock hypothesis. Am J Obstet Gynecol 1994; 170: 1713–20.
6. Blok BF, Holstege G. The central control of micturition and
continence: implications for urology. BJU Int 1999; 83 (suppl 2): 1–6.64 www.thelancet.com Vol 367.
7. Cockayne DA, Hamilton SG, Zhu QM, et al. Urinary bladder hyporeflexia and reduced pain-related behaviour in P2X3-deficientmice. Nature 2000; 407: 1011–15.
8. Chai TC, Steers WD. Neurophysiology of micturition and continence in women. Int Urogynecol J Pelvic Floor Dysfunct 1997;8: 85–97.
9. Thor KB, Katofiasc MA. Effects of duloxetine, a combined serotonin and norepinephrine reuptake inhibitor, on central neural control of lower urinary tract function in the chloraloseanesthetized female cat. J Pharmacol Exp Ther 1995; 274: 1014–24.
10. Chaliha C, Kalia V, Stanton SL, Monga A, Sultan AH. Antenatalprediction of postpartum urinary and fecal incontinence. Obstet Gynecol 1999; 94: 689–94.
11. Bump RC, Norton PA. Epidemiology and natural history of pelvic floor dysfunction. Obstet Gynecol Clin North Am 1998; 25:723–46.
Some are parts:
Training Isolated Kegels Exercise in Stress Urinary Incontinence (Part 1)
Training Isolated Kegels Exercise in Stress Urinary Incontinence (Part 2)