CHAPTER: 1 1.1 Introduction: Sports can sometimes cause injuries. Sports injuries can happen as results of-
Not warming up properly before exercising more vigorously.
Pushing too hard for their current level of fitness, Before starting or taking up a new sport, it is also a good idea to visit your GP for a check-up & fitness assessment.
Some common sports injuries include: Sprains, Strains, Cuts & bruises, Bone fractures & breaks, Tendonitis, blisters & Head injury1.
Injuries to the knee are the most common reason people see an orthopedic physician. The structure and stress placed upon the knee make it vulnerable to a variety of injuries. The largest joint in the body is the knee. It is comprised of the lower end of the femur and the upper end of the tibia. The patella (kneecap) slides in a groove on the end of the femur, and covers the joint. Several large ligaments support the knee on either side. The meniscus and cartilage cushion the knee and act as a shock absorber during motion2.
There were no injury data available for community-based contact football in Canada. Literature review revealed an absence of prospective methodologies for evaluating risk factors & crafting prevention plans for pediatric sports injury. This report summarizes key aspects of injuries among the National Capital Amateur Football Association (NCAFA) players during the 2005 season & tests the feasibility of a conceptual framework for creating an injury surveillance program aimed at tracking incidence & prevalence of injuries in amateur-community sport. The salient finding of this prospective study points to an increased risk of potentially catastrophic injuries among the youngest players in the league. Though the relative incidence of injuries among these players was substantially lower, they were more serious (cervical spine & back)3.
1.2 Justification of the Study:
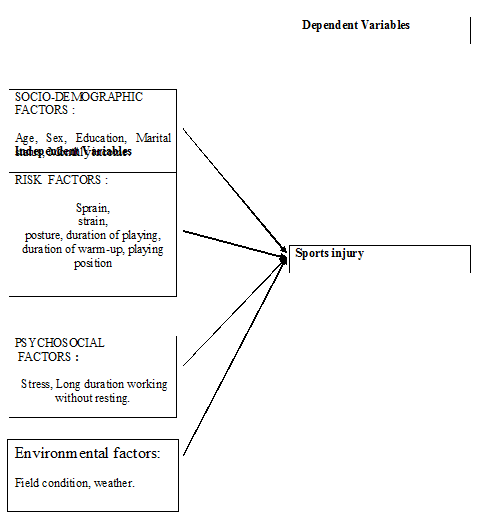
Football players associated with different injury which involves illness and affects good playing. It is the concern of study because the nature, type and severity of different injury increases due to faulty posture, action & over stretched which ultimately expense money, lost days from play & reduce. This study will be expected to determine prevalence & risk factors associated with different injury as to examine the magnitude of this problem. This study also expects to disseminate the findings of this study to take necessary steps to minimize the injury & reduces the cost.
1.3 Operational Definition:
Knee Injuries
Patellofemoral Syndrome Also called “Runner’s Knee,” problems associated with the patella, or kneecap, are common in runners. The term runner’s knee may refer to several common injuries such as chondromalacia, patellar tendonitis, or generalized knee pain.
Dislocating Kneecap A dislocating kneecap causes acute symptoms during the dislocation, but can also lead to chronic knee pain. Patients who have a dislocating kneecap may improve with some specific physical therapy strengthening exercises.
Plica Syndrome Plica syndrome occurs when there is irritation of the lining of the knee joint. Part of the lining of the knee joint is more prominent in some individuals, and can form a so-called plica shelf. If this tissue becomes inflamed, it can cause knee pain.
Leg Injuries
Shin Splints Shin splints, like runner’s knee, is a term that describes a set of symptoms, not an actual diagnosis. Shin splint pain can be due to problems with the muscles, bone, or the attachment of the muscle to the bone.
Stress Fractures Stress fractures of the hip are usually seen in long distance runners, and much more commonly in women than in men. These injuries are usually seen in endurance athletes with deficient nutrition or eating disorders.
Exercise Induced Compartment Syndrome Exercise induced compartment syndrome is a condition that causes pain over the front of the leg with activity. Patients with exercise induced compartment syndrome may require surgery, call a fasciotomy, to relieve their symptoms.
Ankle Injuries
Ankle Sprain Ankle sprains are common injuries that runners experience. Early recognition and treatment of this problem will help speed your recovery from ankle ligament injuries.
Achilles Tendonitis Achilles tendonitis is a painful condition of the tendon in the back of the ankle. Left untreated, Achilles tendonitis can lead to an increased risk of Achilles tendon rupture.
Foot Injuries
Plantar Fasciitis Plantar fasciitis is a syndrome of heel pain due to inflammation of the thick ligament of the base of the foot. A tight, inflamed plantar fascia can cause pain when walking or running, and lead to the formation of a heel spur.
Overpronation Pronation is a normal movement of the foot through the gait cycle. When this motion becomes excessive, overpronation can cause a variety by altering the normal mechanics of the gait cycle. Shoes to control excess foot motion can be helpful for overpronators.
Arch Pain Arch pain is a common foot complaint. Arch pain, also sometimes called a strain, often causes inflammation and a burning sensation under the arch of the foot. Treatment of arch pain often consists of adaptive footwear and inserts4.
1. Abdominal Strain
Although abdominal injuries aren’t as common in football as injuries to the joints, bones and muscles in the groin area and legs, players can still suffer from strains in the stomach region from overstretching when jumping and reaching for the ball.
2. Strained Hamstrings
Football is the most popular sport in the world, with 240 million players registered worldwide. Footballers tend to suffer more from injuries in the lower half of their bodies, particularly around the groin, knee and ankle joints and leg muscles.
3. Torn Anterior Cruciate Ligament
Footballers tend to sustain more injuries than other sportsmen and women, although most of them aren’t serious injuries. Two thirds of injuries on the football pitch are sustained through bad collisions with opponents and from sudden awkward movements, overstretching muscles or landing badly from a jump. Older or female players are more prone to injury than younger male players5.
1.4 Research Question
1. What is the Proportion of various Sports injury among the Football player?
CHAPTER: 2
2.1 Literature review:
Baby Boomer Sports Injuries, U.S. Consumer Product Safety Commission, April 2000. A total of 173 injuries occurred over the two seasons, with 55% of players affected; The overall injury incidence was 1.93 injuries per 1,000 player hours. However, the game incidence, at 12.63 per 1,000 hours, was much higher than the practice incidence, at 1.17;
Most injuries (60%) were located in the lower extremities, with strains (30.7%), sprains (19.1%), contusions (16.2%) and fractures (11.6%) the most common diagnoses and the knee (31.8%) and head (10.9%) the most common sites of injury. Anterior cruciate ligament (ACL) injuries accounted for 4.6% of all injuries and the incidence of ACL tears was 0.09 per 1,000 player hours;
Midfielders suffered the most injuries (34.1%); Injuries were most likely to occur in the latter portion of the competitive season and were least common during the post season. The overall injury rate of 1.93 per 1,000 player hours was significantly lower than that observed in the corresponding male professional league (Major League Soccer) of 6.2 per thousand hours.
We are all urged to exercise in order to keep fit and to avoid getting fat. Sports seem like a fun way of burning extra calories to lose weight, but according to a U.S. Consumer Product Safety Commission report, sports injuries among baby boomers increased by 33 percent from 1991 to 1998[6] There were about 276,000 hospital emergency room-treated injuries to persons 35 to 54 in 1991 compared to more than 365,000 sports injuries to persons of these ages in 1998. The number of injuries keeps increasing every year. In 2006, the National Electronic Injury Surveillance System (NEISS) reported over half a million injuries just for basketball. Another two million injuries were associated with bicycling, football, other sports7.
The injury data from the first two seasons of the Women’s United Soccer Association (WUSA) were analysed to determine the injury incidence, anatomic location of injuries, and relation of player position.
A total of 173 injuries occurred in 110 players with an overall injury incidence rate of 1.93 injuries per 1000 player hours. The incidence of injury during practice and games was 1.17 and 12.63 per 1000 player hours, respectively. Of the injuries 82% were acute and 16% were chronic. Most of the injuries (60%) were located in the lower extremities. Strains (30.7%), sprains (19.1%), contusions (16.2%), and fractures (11.6%) were the most common diagnoses and the knee (31.8%) and head (10.9%) were the most common sites of injury. Anterior cruciate ligament (ACL) injuries accounted for 4.6% of all injuries and the incidence of ACL tears was 0.09 per 1000 player hours (practice 0.04, game 0.90). Midfielders suffered the most injuries (p<0.007).
Soccer is the world’s most popular organised sport with over 200 million males and 21 million females registered with the Fèdèration Internationale de Football Association (FIFA). Epidemiological studies of male soccer players have identified an incidence of 10–35 injuries per 1000 game hours, equivalent to every player incurring one performance limiting injury per year. A review of the English professional male soccer leagues revealed that muscle strains (37%), ligament sprains (19%), and contusions (13%) were the most common types of injury, and that the thigh (23%), knee (17%), and ankle (17%) were the most common sites of injury. Studies on professional and amateur female soccer players in Sweden have demonstrated an incidence of up to 24 injuries per 1000 game hours and up to seven injuries per 1000 practice hours.
Several studies have identified female soccer players as having a higher incidence of knee injury and anterior cruciate ligament (ACL) injury than males. In a prospective study of female soccer players, Östenberg and colleagues determined that general joint laxity and age over 25 are risk factors for knee injury; however, no study has proven that a single etiology is responsible for female ACL injury patterns.
In the United States 12.5–18.5 million people play soccer, with an estimated annual increase in participation of up to 21.8%. The growing popularity of soccer in the United States has led to the recent formation of professional male (1996) and female soccer leagues (2001). The first women’s World Cup soccer tournament was held in 1991 and the Women’s United Soccer Association (WUSA) was the premier female soccer league in the world from 2001 to 2003. The interest of female athletes in soccer necessitates continued investigation of injuries in order to identify injury patterns and effective means of prevention. The injury data from the first two seasons of the WUSA were analysed to determine the injury incidence, anatomic location of injuries, and relation of player position.
Injuries in this study were defined as those conditions which were reported to and evaluated by the team physician or athletic trainer. Each injury was subsequently reported to the league insurance company via a standardised “first report of injury” form which is completed by the team trainer. All injury reports were verified by an examination by the team physician. A detailed account of each injury is recorded in a general computer database and includes the date of injury, injury location, diagnosis, injury description, and reimbursement cost.
For this investigation, the information in the database from all eight teams during the 2001 and 2002 pre-season, season, and post-season was carefully reviewed and each team trainer was contacted for further injury detail. Each player signed a release of medical records form as part of their WUSA contract. A numerical code was assigned to each player to protect confidentiality and permission for the use of the information was granted by the WUSA administration (Atlanta, GA) and American Specialty Insurance Services, Inc. (Roanoke, IN).
Injury onset was determined by the detailed injury description, if available. An acute injury was defined as any injury or condition which had not existed prior to the date of injury occurrence. A chronic injury was any injury with insidious progression that existed prior to the date of injury occurrence or an exacerbation of a previously existing condition.
The average number of practices per season (125 sessions, average time 100 min) as recorded by team trainers and the average number of games per season (21 games, average time 90 min) for all teams was used to calculate the injury incidence using the method described by Hawkins and Fuller. The season runs from mid-February until August with additional post-season play. The season was divided into pre-season (mid-February through March), early season (April through May 15th), midseason (May 16th through June), late season (July through end of season games in mid-August), and post-season. All calculations were performed using Microsoft Excel (Microsoft, Seattle, WA) and Statistica (Statsoft, Tulsa, OK). χ2 Statistical tests were used to analyse the data, with significance accepted at p<0.05 unless otherwise indicated.
A total of 173 injuries occurred over two seasons: 93 injuries occurred during 2001 and 80 occurred during 2002. Of 202 players participating in the WUSA during the two seasons, 110 suffered injuries; therefore 55% of players were injured. The overall injury incidence rate was 1.93 injuries per 1000 player hours. Game versus practice information was available for 168 injuries, and the game and practice injury incidences per 1000 player hours were 12.63 and 1.17, respectively.
Strains (30.7%), sprains (19.1%), contusions (16.2%), and fractures (11.6%) were the most common diagnoses. The most common location was the knee (31.8%), followed by the head (10.4%), ankle (9.3%), and foot (9.3%); 60% of the injuries occurred in the lower extremities. Of the injuries 82% were acute (142), 16% were chronic (28), 0.6% were acute on chronic (one), and 1.4% were undetermined (two).
Of 18 head injuries, fractures of the nose and facial bones (five, 27.8%) and concussions (five, 27.8%) occurred most frequently. The remainder of the head injuries were lacerations and contusions. The incidence of concussions was 0.06 per 1000 player hours.
Ankle sprains accounted for 86.7% of ankle injuries and 7.51% (13) of all injuries. Eight of 13 ankle sprains involved a plantarflexion/inversion mechanism.
Of 20 fractures, the face and teeth (six, 30%) and the foot (five, 25%) were the most frequent sites of injury. Stress fractures (one tibia, one first metatarsal) accounted for two fractures (10%) and the remaining 18 were the result of acute situations.
A total of 55 knee injuries occurred. Strains were the most common injury (15, 27.3%) followed by contusions (nine, 16.4%), ACL injury (eight, 14.6%), sprains not involving the ACL (seven, 12.7%), inflammation (seven, 12.7%), and meniscal tear (five, 9.1%). Follow up investigation on the diagnosis of knee ligament sprain was performed to determine if an ACL injury had occurred. There were eight acute ACL tears during the two seasons, five from games and three from practices. Six of the eight were the result of non-contact situations, two were from collisions, and one was associated with a meniscal tear. The incidence of ACL tear was 0.09 per 1000 player hours. ACL tear rates during games and practice were 0.90 and 0.04, respectively, per 1000 player hours.
Player position at the time of injury was recorded for 168 players. Midfielders sustained the most injuries (57, 34.1%) followed by defenders (47, 28.1%), strikers (38, 22.8%), and goalkeepers (26, 15.0%). Compared to all players, midfielders suffered a significantly higher number of injuries (p<0.007); however, compared to other field players, midfielder injuries did not reach a significant value.
The overall incidence of injury in this study was 1.93 injuries per 1000 player hours. The game incidence was 12.63 and the practice incidence was 1.17. Our findings are consistent with both the practice injury rates (range 1.5–7 per 1000 player hours) and the game injury incidence (range 9.1–24 per 1000 player hours) found in other female soccer studies.Higher game injury rates have also been found in male soccer and have been attributed to greater intensity of play during games.
Morgan and Oberlander investigated the injuries of the inaugural season of Major League Soccer (MLS) and found an overall injury rate of 6.2 injuries per 1000 player hours. In accordance with their method study, we included all injuries, such as upper extremity and facial injuries, and not just those which resulted in time lost from play. Our finding of 1.93 injuries per 1000 h in the WUSA is important as it may indicate that professional female soccer players in the United States suffer less injuries than their male counterparts.
Although soccer epidemiology studies in the 1970s and early 1980s. showed that females had a higher injury rate, age and skill level may have more of an influence on injury incidence than gender alone. In a 5 day invitational tournament in 1985 with over 6000 players, Schmidt-Olsen found that females aged 17–19 had a much higher injury rate (47.1 per 1000 h) compared to males in the same age group (20.6 per 1000 h). In 1984, Maehlum studied injuries at the Norway Cup, one of the world’s largest youth club tournaments, and found the injury rate to be twice as high in females as in males. In 1999, Maehlum compared values from the 1984 tournament to the 1993 and 1997 tournaments, and found a 35% total decrease in total injuries with a 50% reduction in female injuries. Elias identified a gradual decrease in the incidence of injuries in female soccer players from 1987 to 1997 in a recent study in which injuries from a youth soccer tournament were recorded prospectively over 10 years. Data from the 1999–2000 NCAA injury surveillance system revealed a nearly equal game injury rate in males (20.75 per 1000 player exposures) and females (18.75 per 1000 player exposures); therefore, improved training, fitness, and skills may contribute to the low incidence found in this investigation.
Five concussions occurred during the two seasons (approximately one concussion every 15.3 weeks) and all five situations involved player to player collisions. Boden determined the incidence of concussion in female collegiate soccer players to be 0.44 per 1000 athlete exposures, that is approximately one concussion every 13.5 weeks or one concussion per team per year. Boden also found that 76% of concussions resulted from player to player or player to object (goal post, elbow, sideline advertisement) contact and only 24% resulted from head to ball contact from a ball kicked at full force at a close range. The relationship of chronic traumatic brain injury and soccer remains a controversial topic, as Tysvaer and Matser have shown in separate studies that soccer players exhibit deficiencies in memory and planning compared to controls. In contrast, a recent study used similar neuropsychological tests to those used by Matser and showed that soccer related concussions were not associated with impaired neurocognitive function. Jordan and colleagues compared 20 national soccer team members to controls and found no differences in brain MRI findings.
The finding of an increased number of injuries during the late season is consistent with other studies of both male and female soccer injuries. The increase in injuries during the end of the season could be due to deconditioning or an increase in play intensity for play-off or tournament positions. The lower incidence in post-season play is expected as fewer players participate.
Information on professional female players is limited, and studies on amateur and youth females have identified practice and game injury rates of 1.5–7 and 9.1–24 per 1000 player hours, respectively. Female soccer players have a four times higher risk of knee and ACL injury than males.
The knee was the most common injury site in our study (31.8%), and this finding is consistent with the study of female soccer players by Östenberg .An awareness of the propensity of knee injuries in female soccer players is particularly important for the team physician and team trainer, as it has been shown that 12 years post-injury, 34% of previous female soccer players in Sweden who suffered an ACL injury have radiographic changes consistent with osteoarthritis.
An overall incidence of 0.09 ACL injuries per 1000 player hours was found in this study. Five of the eight ACL injuries occurred during games (0.90 ACL injures per 1000 game hours). Bjordal and colleagues found an incidence of 0.10 per 1000 h, and other investigators found 0.31 ACL injuries per 1000 h Only two of eight ACL injuries involved contact situations, and although the number of ACL injures is too small to reach statistical significance, these results are consistent with published data that a majority of ACL injuries occur in non-contact situations.
Some authors have shown that pre-season neuromuscular training and plyometrics can decrease knee injury rates in females. Junge and Chomiak have shown a lower injury rate in elite players compared to less skilled players, and others have shown that pre-season conditioning and fitness can reduce overall injury rates. The elite soccer players in this study have achieved the highest level of play possible in female soccer; therefore, our findings of a low injury rate could reflect the high level of fitness needed to participate in the WUSA and the impact of proper pre-season strengthening and training. Additionally, our results could represent a “pre-selection” phenomenon in which players who are at risk for an ACL injury may have had an injury earlier in their career and not reached the WUSA or have had an ACL reconstruction procedure prior to their participation in the WUSA.
The use of an insurance database has the limitation of selecting only for those injuries which resulted in an insurance claim. Although all injuries were reviewed by the team trainers and physicians, it is likely that some minor abrasions and contusions were not recorded and may have lowered the injury incidence in this study. Also, the use of a database can not always provide the level of detail for each injury desired for a more comprehensive study. Moreover, the high proportion of fractures and other severe injuries could be due to the selection bias from the type of database utilised.
A preliminary study of the injuries among 202 elite female soccer players has shown that the incidence of injury in the WUSA is similar to that found in the existing literature on female soccer injuries, and that rates during game play are much higher than during practice. Injures about the knee are most common and continue to predominate even in these high-level athletes. The results of this study accentuate the importance of a more comprehensive analysis of the injury patterns in these elite athletes to enable the creation of prevention protocols for professional, amateur, and youth female soccer players8.
To investigate the influence of playing multiple games on multiple days on youth soccer medical encounter rates.
211 players surveyed with 195 eligible and completed questionnaires. There were 4.06, 5.14 and 3.92 medical encounters/1000 MH on 11, 12 and 13 July, respectively, with no significant difference in injury incidence. There was no difference in medical encounter rates of second games compared with first games of the day (p=0.126). Daily medical encounter rates were 5.65, 8.95, 7.83, 6.94 and 4.62/1000 MH on 15, 16, 17, 18 and 19 July, respectively, with statistically significant differences on 16 July (p<0.001) and 17 July (p=0.022) compared with 15 July. Encounter rates of second games compared with first games of the day showed no difference (p=0.385). A linear test for trend from 15 to 19 July was not significant (p=0.092).
The USA Cup format did not show either increased medical encounter rates from the cumulative total of games played or a consistently increased rate in the second game of the day compared with the first. Players, coaches, parents and administrators can feel confident that this tournament format does not pose an additional risk of injury.
The epidemiology and mechanisms of soccer injuries have been studied on numerous occasions, and some are specific to youth soccer. Several studies focus on specific soccer-related injuries, others distinguish between injuries that occurred during game play from those that occurred in practice, and some attempted to break down the game into individual halves or even smaller time periods to look for differences in injury rates. Most of the articles that discuss injury rates in the first half of the game compared with the second addressed professional soccer tournaments such as the World Cup, with a very different scheduling format from the usual youth soccer tournament.
One potential risk factor is the rigor of playing several games within the tight timespan of a youth soccer tournament. There is little known about the effect of playing multiple games on successive days during youth soccer tournaments on the injury rate. There is a need for research into the effect of tournament scheduling on medical encounter rates in youth players to understand the effect of various tournament formats.
This study tested the following hypothesis: there is an increase in medical encounter rates on successive days of the tournament or during the second game of the day compared with the first in this tournament format.
This study was a prospective cohort study of participants in two separate tournaments of the 2008 USA Cup (Blaine, Minnesota, USA). The first was the 11–13 July USA Cup Weekend (approximately 450 teams) with round robin play on 11 July and the morning of 12 July and single elimination games starting on the afternoon of 12 July and completed on 13 July. The second was the 15–17 July USA Cup (approximately 500 teams) with round robin play on 15–17 July and single elimination games played on 18 and 19 July. Each team played a minimum of three games in either the USA Cup Weekend or the USA Cup, or six games if entered in both. Players on teams that advanced during the elimination rounds potentially played six games in 3 days in the USA Cup Weekend and seven games in 5 days in the USA Cup. The first games of the day started at 07:50 hours, and the last games started at 19:10 hours. The minimum time interval between games played on the same day was 3 h, except in four games that had just over 1 h recovery time.
The tournament included both boys and girls teams from under 13 years to under 19 years brackets. The teams were of varied skill levels in each of the age brackets, and unlimited substitution was allowed in the younger age groups. The games were different lengths based on age, and all were shorter than the age group regulation game length until the final age group championship game Unlimited substitutions were permissible in all games for under 13 years to under 16 years teams and Fédération Internationale de Football Association Substitutions Rules were observed in the under 17 years to under 19 years age groups. When the weather (eg, heat) dictated, the games were further shortened, additional water breaks were instituted and unlimited substitution was allowed for all age groups.
USA Cup Weekend and USA Cup game durations
The following inclusion criteria were used to determine medical encounters: participants of either tournament who received medical attention at the central medical facility for injuries sustained or medical issues arising during match play. Medical encounters included: both acute and acute on chronic musculoskeletal injury; skin laceration or abrasion; heat injury, heat exhaustion or heat stroke; and concussion or head injury.
The following exclusion criteria were used: participants injured outside of match play; participants with exercise asthma or asthma, infectious disease, colds, sore throats and medical problems not related to match participation; and non-participants of the tournaments.
All players and a parent/guardian signed a medical liability waiver before entering in the tournament. As a parent/guardian was not always present when an injured participant presented for evaluation, additional consent was waived, and the research team volunteers explained to the participants the study purpose and content, emphasising that participation was voluntary. Each participant was also provided an ‘information sheet’ describing the project and its goals.
The survey data were summarised by means of descriptive statistics using medical encounters per 1000 MH. MH (also known as player game hours) were chosen for the denominator because the total MH for the tournament, each day, and the first and second games, can easily be calculated, and the MH calculation does not require access to the roster and individual game records necessary to assess athlete exposures. For example, a match with 1 h of playing time and 11 players on each side would have 22 MH independent of the roster size and individual player time. Although the playing time of individuals on each team varied, the total playing time and the total MH for each game were constant. Total and daily MH were calculated from the summation of the maximum allowable game time obtained from game schedules for each age level and the maximum number of players allowed on the field. The MH for each game were calculated for each day, the first and second game for each day, and for the tournament to obtain the exposure data. Measuring the incidence per 1000 MH allows a comparison of medical encounter rates as the number of games and players decreased in the elimination arm of each tournament.
Poisson regression was used to model the incidence densities of soccer medical encounters comparing the second game of the day with the first game of the day and comparing sequential days of the tournament with the first day of the tournament. In addition for the USA Cup, the last day of the tournament was compared with the day before. Medical encounters in the second half of game play were compared with the first half for the first and second games of each day. Separate analyses were performed for games on 11–13 and 15—19 July. A linear test of trend from the Poisson regression model was performed to see if there was a day trend. p Values less than 0.05 were considered statistically significant. The GENMOD procedure from SAS version 9.1.3 was used for the analyses.
The combined medical encounter rate for the USA Cup Weekend was 4.44/1000 MH and the daily encounter rates are shown in. There was no significant between-day difference in the medical encounter incidence for the games (12 July compared with 11 July (p=0.718; incidence density ratio (IDR) 1.26, 95% CI 0.36 to 4.33) or 13 July compared with 11 July (p=0.982; IDR 0.98, 95% CI 0.14 to 6.83)). The daily medical encounter rates for first and second games are shown in. There was no significant difference in the medical encounter incidence between the second and first game on any of the tournament days (p=0.126; IDR 0.45, 95% CI 0.16 to 1.25). Medical encounter rates for the second half compared with the first of each game are shown in with no significant between-half differences seen for the first (p=0.265; IDR 0.69, 95% CI 0.36 to 1.33) or second (p=0.829; IDR 1.25, 95% CI 0.17 to 9.43) game of the day.
The combined encounter rate for the USA Cup was 6.95/1000 MH and the daily medical encounter rates are also shown in There were statistically significant differences in the medical encounter incidence comparing 16 July with 15 July (p<0.001; IDR 1.58, 95% CI 1.21 to 2.06) and 17 July with 15 July (p=0.022; IDR 1.38, 95% CI 1.05 to 1.82). There was no significant difference seen on either 18 July (p=0.169; IDR 1.21, 95% CI 0.92 to 1.60) or 19 July (p=0.282; IDR 0.82, 95% CI 0.57 to 1.18) compared with 15 July. A linear test for trend from 15 to 19 July was not significant (p=0.092). There was no difference in the medical encounter rates of the second compared with the first games of each day (p=0.385; IDR 0.79, 95% CI 0.47 to 1.34) as shown in.
The encounter rate comparisons for the first and second half of each game are illustrated in. The second half of the first games played from 15 to 19 July had higher medical encounter rates compared with the first half (p=0.039; IDR 1.62, 95% CI 1.03 to 2.56). No difference was found in the half comparisons of the second game of the day (p=0.766; IDR 1.17, 95% CI 0.42 to 3.22).
In the course of each tournament, 46 players sought medical attention related to the first game, 45 in the second game, 33 in the third game, 40 in the fourth game, 22 in the fifth game and six in the sixth game.
The results of this study do not indicate a clear relationship between medical encounter rates and either the total number of games played or the number of games played per day in this tournament. In a previous study of the USA Cup soccer tournaments from 1988 to 1997, the mean injury rate for both boys and girls playing in the tournaments was 13.23 injuries per 1000 MH, and a downward trend in injury rates was noted across the decade, with the lowest injury rate of 8.57/1000 MH in 1996, but the game-to-game and day-to-day injury rates were not addressed. The combined girls and boys mean injury rate in the 2008 tournaments was lower than previously identified injury rates. Beyond that, comparison with the previous USA Cup and other tournament studies is difficult as the injury rates are not segregated by game.
The frequency of injuries increased slightly after the first day in both tournaments, but began to trend down in successive days as each tournament progressed to the final day and the number of teams involved in play decreased. There was no significant difference in injury rates between the first and second games of the day in either tournament. This suggests that participation in up to two games a day or in several games in successive days did not increase medical encounter rates, and cumulative fatigue may not be a significant injury risk factor in this tournament format. In the USA Cup, medical encounter rates were significantly increased on the 16 and 17 July compared with 15 July (first day of the tournament), but this difference was not carried through to 18 and 19 July (fourth and fifth days of the tournament). The games on the 15–17 July were in round robin format, in which club teams with lesser skill levels may be paired against select teams that train more vigorously; pitting less evenly matched teams against each other might explain the increase in injury rates. In the single elimination portion of the tournament on 18 and 19 July, opponents were more evenly matched based on performance in the round robin portion of the tournament, which may account for the baseline injury rates.
In the USA Cup Weekend, there was no significant difference between injury rates in the first and second half in either the first or second game of the day. The same was not true for the USA Cup in which there was a greater rate of injury in the second half compared with the first half of the first game, with no significant difference shown in the second game. One potential reason for increased injury in the second half of the game is fatigue, but it would stand to reason that fatigue would be greater in the second game and second game data do not support this explanation. However, players may pace their effort to avoid excessive fatigue, as hypothesised in elite soccer, and play less aggressively in the second game of the day. A recent study investigated thermal and cardiovascular strain associated with two identical 80 min bouts of strenuous exercise in the heat separated only by 1 h rest. The investigators wanted to see if this group of young athletes could recover adequately with 1 h of rest. The 1 h of cool-down, rest and rehydration was found to be adequate to eliminate the apparent carry-over effects from the first bout of strenuous exercise. Each USA Cup player had 3 h rest between same-day games except for four games that had just over 1 h rest, which should have provided adequate time to recover from the previous game. Most teams in the USA Cup only play one game on each of the first 3 days of the tournament. As the majority of soccer-related injuries occurring in a game are caused by contact, it is conceivable that these injuries are caused by rough play occurring later in the game.
The data addressing the total games played when an injury occurred were not normalised to MH as a result of insufficient information to calculate the rates; therefore, the effect of cumulative games could look different when normalised, but it is doubtful that the difference would change the conclusions drawn based on the other data presented in this study9.
3.2 Objectives of the Study
3.2.1 General Objective:
To determine the Proportion of various Sports injury and factors associated with sports injury among the football player.
3.2.2 Specific Objective:
To determine the Proportion of various Sports injury among the Football player
To find out the factors associated with sports injury among the football player.
To assess the specific type of treatment seeking due to sports injury among the football player
To determine the socio-demographic factors associated with sports injury among the football player.
To find out the environmental factors of sports injuries among the football player.
3.3 Study Design
Descriptive Cross-section Study was conducted to determine the Proportion and factors related to sports injury among the football player.
3.4 Study population:
The study population were consist of male player with age of 15-35 years playing in different clubs, leagues etc.
3.5 Study area:
This study was conducted in Bangladesh Krira Shikkha Protisthan Kendra (BKSP) and clubs in Bangladesh.
3.6 Study Period:
The duration of the study were 3 months. The study was conduct from April, 2010 to July, 2010. The entire period divided into different activities.
3.7 Sample Size:
Formula of one- sample population were used for calculating sample size.
Z2 pq
n= ——————-
d2
Here
n= the desired sample size.
z= the standard normal deviate usually set at 1.96 which correspondents to 95% confidence level.
p= the proportion of the target population estimated to have a particular characteristics.
q= 1-p
d= degree of accuracy desired, usually set at 0.05%.
Now, required sample size was:
n= 384 n = z2pq/d2
= (1.96)2 X 0.5 X 0.5.
(0.05)2
= 384.16
Where
z= confidence level = 95% for this study.
p= estimated prevalence rate of sports injury among the football player = 50%
q= 1-p=50%
d= desired decision level = 0.05
n= desired sample size.
n= 384
3.8 Inclusion & exclusion criteria:
Inclusion criteria:
Those who were give consent and participate for interview.
Only male football player of age 18-35 years playing football.
Duration of playing football 2 months & above.
Exclusion Criteria:
The person who were not voluntarily interests.
Female footballer.
Others players.
3.9 Sampling Technique:
Sample was selected purposively to interviewed the study population considering the inclusion and exclusion criteria.
3.10 Data collection Instrument/ Tools
An interviewer administered structured questionnaire were designed to collect information on related sports injury associated with the football player, that was prepared in advance and evaluated by the principal supervisor before data collection. The questionnaire were consist of 2 sections of items. The first section was include items on socio-demographic characteristics and background information of the football player like sex, age, occupation, years of playing football, and hours on play per day & week.
3.11 Data collection procedure:
Data collection procedure was involve face to face interview and computer workstation check list with help of interviewer administered structured questionnaire.
3.12 Data management and analysis
After collection of data, all interviewed questionnaire were checked for its completeness and internal consistency to exclude missing or inconsistent data and those were discarded. Corrected data was enter into the computer. The data was analyze by using the statistical software namely SPSS (Statistical Package for Social Science).
3.13 Ethical issues
Before data collection, permission from the Ethical Committee of State College of health Science (SCHS) was taken and a request letter was hand over, to the appropriate authority of study area for taking permission and seeking assistance foe smooth access to data collection. All ethical issues related to research involving human subjects were address according to the guidelines of Medical Research Council (BMRC) and the Ethical Review Committee of WHO. Prior to data collection, the objectives of the study were explained in understandable language to the study participants and their written informed consent was taken. The prospective participants were given free opportunity to receive summary of the study in writing before give consent and take part of the interview of the study. Participant’s right to refuse and withdraw from the study was accepted. All questionnaire and ethical documents were translate into Bengali before interview.
3.14 Expected outcomes of the study:
The study was expected to determine the proportion of sports injury among the football player.
The study was also be expected to development of sports injury among the football player and find out psychosocial factors in the development of sports injury among the football player.
CHAPTER 5
5.1 Conclusion
This study concludes that football players suffer from different types of injuries due to age, monthly income, playing position, playing time, field condition and weather. The result showed that the most complained injuries are minor muscle strain 18.5%, fracture
17.5%,muscular pain 17%, ligament sprain 13.5%, contusion 10.5% and muscle soreness7%, blister 8.5%, dislocation 7.5% are the least complained injuries when playing or done playing related activities. Among these highest rate of injury was occurs in ankle 29.5%, knee 23%, elbow 24.5%, and neck 28% . Practically, the result of this study would help in preventing injury associated with playing football.
5.2 Recommendation
Based on the study findings, the following recommendations are made with view to prevent and minimize the sports injury among football players.
1. a systemic evaluation can provide crucial guidance and corrective feedback for current and future good health and safety efforts.
2. In concept of preventive rehabilitation, the role and scope of expertise of the physiotherapist should be enlarged in providing advice and education towards proper ergonomics. Counseling and working with authorities will further assist in reduction of injuries that can lead to different injuries among the football players.
3. The following precautions should be followed during playing football:
Must should be take water or fluid before playing or training.
Complete injury related training before started play in every players.
All players should receive pre-season physical exams, and those with a history of prior brain or spinal injuries, including concussions, should be identified.
Football players should receive adequate preconditioning, and strengthening of the head and neck muscles.
Every players should regular stretching to relax their body before playing or training.
Using comfort equipment such as- kneecap, sports shoe, shocks, aglet etc.
Protective eyewear and mouth guards may help reduce the numberof some nonfatal head and facial injuries.
Coaches, and soccer organizationsshouldwork to promote enforcement of all safety rules and stronglyencourage sportsmanship, fair play, and maximum enjoyment forthe athletes.
Coaches must be prepared for a possible catastrophic spinal cord injury. The entire staff must know what to do in such a case; being prepared and well informed might make all the difference in preventing permanent disability.