Forensic Medicine and Toxicology
Medical Ethics
Definition:
Medical ethics may be defined as the moral principles, which guide the members of medical profession in course of their practice of medicine & their dealings with their patient, other members of the profession & with the state.
Medical etiquette:
It is the laws of conventional courtesy observed between the members of medical profession.
Declaration of World Medical Association:
Date | Name | Subject |
| 1970 | The declaration of Oslo | Therapeutic abortion |
| 1973 | The declaration of Munich | Racial, political discrimination etc. in medicine |
| 1975 | The declaration of Tokyo | Torture & other cruel & degrading treatment or punishment |
| 1975 | The declaration of Helsinki | Human experimentation & clinical trails |
| 1981 | The declaration of Lisbon | Rights of the patient |
| 1983 | The declaration of Venice | Terminal illness |
| 1983 | The declaration of Oslo | Therapeutic abortion |
| 1984 | The declaration of Sao Paulo | Pollution |
| 1987 | The declaration of Madrid | Professional autonomy & self regulation |
| 1987 | The declaration of Rancho Mirage | Medical education |
| 1989 | The declaration of Hong Kong | The abuse of the elderly |
| 1995 | The declaration of Lisbon | The rights of the patient |
| 1996 | The declaration of Helsinki | Biomedical research involving human subjects |
| 1997 | The declaration of Hamburg | Support for doctors refusing to participate in torture or other forms of cruel in human or degrading treatment |
| 1998 | The declaration of Ottawa | The right of the child to health care |
Geneva Declaration of 1948:
- I solemnly pledge myself to consecrate my life to the service of humanity
- I will give to my teachers the respect and gratitude which is their due
- I will practice my profession with conscience and dignity
- The health of my patient will be my first consideration
- I will respect the secrets which are confided in me even the patient has died
- I will maintain by all means in my power, the honor and noble traditions of the medical profession
- My colleagues will be my brothers and sisters
- I will not permit consideration of religion, nationality, race, party politics, or social standing to intervene between my duty and my patient
- I will maintain the utmost respect for human life from the time of conception & even under threat; I will not use my medical knowledge contrary to the laws of humanity
10. I make these promises solemnly, freely and upon my honor.
Codes of medical ethics:
- Duties of physician in general
- Duties of physician to the sick
- Duties of physician to each other
BMDC:
Bangladesh medical and dental council is a statutory body form under medical act 1973 by act on CCC of 1973, to look after the medical profession of the country so that public can identify who is qualified or who is not. The statutory body adopted an ethical code for registered medical practitioner of Bangladesh. It is governing body consisting of 54 members, some are elected & some are nominated. The members hold the office for 5 years. They elect one President & one Member Secretary
Functions of BMDC:
- Maintenance of a register of qualified medical practitioners
- Regulation of the standard of both undergraduate & postgraduate medical education & examination all over the country
- Recognize the medical & dental qualification both from home & abroad.
- Adopts code & ethics for the guidance of its member
- Have disciplinary control to issue warning notice for professional infamous conduct.
- Advise the government when necessary
- Empowered to enter into the negotiation with foreign authorities for setting up a scheme of reciprocity for the recognition of local medical qualifications
Punishment imposed by BMDC:
Disciplinary control:
- Issuance of warning notice
- Erasure of name from register either for temporary period or permanently
The name of the doctor is removed from the medical register under the following circumstances:
- Entries which are made in error or as a result of fraud
- Penal erasure
- i. Issuing a false medical certificate
- ii. Criminal abortion
- iii. Dichotomy
- iv. Covering
- v. Violating the provision of drug
- vi. After the death of the doctor
Criteria of getting BMDC Registration:
- MBBS certificate from an institution recognized by BMDC
- A period of compulsory internship training for a period of minimum one year in an institution approved by BMDC
- One year internship training certificate
- Application form, code of medical ethics
- Nominal fees to BMDC
- Registration has top be renewed every 5 years
Difference between BMDC & BMA
BMDC | BMA |
| Abbreviation is Bangladesh medical and dental council | Abbreviation is Bangladesh medical association |
| Located at 86, Bijoynagar, Dhaka | Situated in BMA Bhaban(in front of National Press club) |
| Giving registration to the doctor | Giving no certificate |
| It is a statutory body | It is a voluntary organization of doctors |
| Provides the course & curriculum of medical education | Cannot provide course & curriculum |
Rights & Privileges of Registered Medical Practitioner:
Right to —
- Choose patient
- Add title, description etc to the name
- Practice medicine
- Dispense medicine
- Posses & supply dangerous drug to patient
- Recovery of fees
- Get appointed at public & local hospital
- Issue medical certificate
- Give evidence as an expert
- Remove eyes of deceased person
- To do justifiable abortion
When a doctor can discontinue treatment?
- When the patient wants to change doctor
- When patient does not follow his instructions about medicine
- When he is not paid
- When the doctor is convinced that patient feigning illness
- When practitioner himself became sick
- When another practitioner is also attending the patient
- When the patient persists in the use of intoxications
Professional Secrecy:
It is an implied term of contract between the doctor and his patient. The doctor is obliged to keep secret all that he comes to know concerning the patient in the course of his professional work. Its disclosure would be a failure of trust and confidence.
A doctor should not discuss the illness of his patient with others without the consent of patient. A doctor should not answer any enquiry by 3rd parties even by near relatives of the patient, either to the nature of illness or to any subsequent effect of such illness on the patient.
Privileged Communication:
It is defined as a statement made by a doctor to the authorities concerned in the interests of the community or the public towards whom who he has a legal, social or moral duty, although such communication under normal conditions contravenes the general rule of professional secrecy.
Justifiable Privileged Communication:
- When doctor is called a witness in a court & judge asks him to make a statement
- When the doctor has a moral or social duty to do so
- To safe guard the doctors own interest
- When it becomes his duty of a doctor as a citizen to help in capture a culprit who has committed a serious come outweigh his obligation to his patient
Examples of Privileged Communication:
- Infectious disease:
If patient suffering from infectious disease is employed as cook, waiter or food handler with enteric infection, or teacher with TB or other disease or as nurse etc, he should be persuaded to leave the job until he becomes non infectious.
- Servants & employees:
An engine driver, bus driver or ships officer may be suffering from epilepsy, high blood pressure, alcoholism, drug addiction or color blindness. Doctor should persuade him to change his employment.
- Venereal disease:
If person is suffering from syphilis & about to marry, it is doctor’s duty to advice him not to marry until cured.
- Suspected crime:
If doctor learns of serious crime e.g. murder, assault, rape by treating victim or assailant, he is bound to give information to the police.
- Self interest:
Both in civil & criminal suits by patient against the doctor, evidence about patient’s condition may be given.
- Patients own interest:
The doctor may disclose patient’s condition to some other person so that he may be properly treated, e.g. to warn the parents or guardians of signs in the patient of melancholia, suicidal tendencies etc.
- Negligence suits
When physician is employed by opposite party to examine patient who has filed suit for negligence, information thus acquired is not privileged & the doctor may testify to such information.
- Courts of law:.
In a court of law, a doctor cannot be privileged concerning the facts about the illness of his patient, if it is relevant to the inquiry before the court. The doctor should protest to the court if he is asked to reveal any professional secret.
Professional Negligence:
Professional negligence is defined as absence of reasonable care & skill or willful negligence of a medical practitioner in the treatment of his patient, which causes bodily injury, or death of patient.
Civil Negligence:
It is a form of negligence in which a patient brings an action for damages in civil court against his medical attendant who owed him a duty of care if he had suffered injury in consequence of negligence or unskilled treatment.
Example of civil negligence:
- Failure to suggest consultation
- Failure to warn of side effects
- Negligent management of procedures
- Experimenting on patient without consent
- Not ordering x-ray examination
- Failure to provide substitute during his absent
- Giving overdose of medicine & poisonous substances carelessly
Criminal negligence:
It occurs when the doctor shows gross lack of competence, gross in attention, gross negligence towards patient. These cases are dealt with in the criminal court
Example of criminal negligence:
- Most cases are associated with drunkenness or impaired efficiency due the use of drug by the doctor
- Amputation of wrong finger or operation on wrong limb or wrong patient
- Leaving instrument, tubes, sponges etc
- Gross mismanagement of the delivery of a woman
- Give wrong or infected blood
- Injecting basal anesthetics n a fetal dosage or in wrong tissue
Contributory Negligence:
Concurrent negligence by the patient & doctor resulting in delayed recovery or hare to the patient
Corporate Negligence: occur when
- Hospital provide defective equipments or drug
- Incompetent employees
- Fails to meet accepted standard of care
Vicarious Liability:
An employer is responsible not only for his own negligence but also for the negligence of his employees (subordinate).
Conditions:
- Employer –employee relationship must be present
- Conduct occur within the scope
- Must occur while on job
- Example-during operation the principle surgeon is not only responsible for his act but also the act of nurse, assistant
Product liability:
The manufactures of drug & medical equipments have legal duty to protect the public against risk of injury associated with their patients. Any deviation from this may result in injury or death of the patient
Doctrine Res-ipsa Loquitor:
The Latin phase meaning ‘the facts speak for themselves’. Generally, the burden of proving negligence lies with the plaintiff only exception is when facts are obvious the defendant is forced to provide an explanation
Example:
- Patient goes to OT for amputation of right Leg but comes out with left leg amputated.
- Failure to remove swab, instrument during operation
- Prescribing overdose of medicine
Conditions invoking res-ipsa loquitor:
- The nature of injury suggests that without negligence it cannot occur
- The plaintiff must not contribute to his own injury
- The defendant must be in exclusive control of the instrument
Professional Infamous Conduct:
It is as conduct on the part of a medical practitioner during the practice of his profession, which would be reasonably regarded as dishonorable or disgraceful by his professional brethren of good repute and competency.
Examples of professional infamous conduct:
- Adultery
- Abortion (performing criminal abortion)
- Alcohol
- Addiction of drugs
- Association for mare countenance of practice
- Advertisement to promote practice
- Avoiding consultation
- Attending a patient who is under care of another practitioner
- Covering
- Contravention of drug law
- Conviction for offences of moral turpitude
- Commercialization of secret remedy
- Dichotomy
- Disregard of personal responsibilities to patients.
- Issuing false certificate
- Running open shop
- Refusing to give professional service on religious ground
- Talking disparately about other colleague
- Prescribing in a secrete formulae
Dichotomy:
Receiving or giving commission or other benefits to a professional colleagues, or manufacturer or trader in drugs or appliances or a chemist, dentist etc.
Medico legal importance:
- It is unethical
- Erasure of name from registration
Fee sharing:
Sharing of fee generally received by a combined operation case among surgeon, his assistants, nurses & bearers
Medico legal importance:
- It is ethical
- No question of erasure of name from registration
Covering:
This means assisting someone who has no medical qualification to attend, treat or perform an operation on some person in cases requiring professional discretion & skill.
Novus Actus Interveniens:
The principle of novus actus interveniens starts that –a person responsible not only for his actions for the legal consequences of that action. According to this theory- a doctor is not responsible for the damage caused by any intervening activity done by a third person during the treatment.
Euthanasia:
Euthanasia means producing painless death of a person suffering from hopelessly incurable with painful disease. It is also known as mercy killing. Practiced in Netherlands, Columbia, Oregon state of USA
It is not possible in Bangladesh- as there is no prevailing law, social &religious factor, and ethical background of a doctor.
Procedure:
- Lethal doses of opium or other narcotic drugs is administer OR
- Withdrawal of all the life saving apparatus
Types:
- Active or positive
- Passive or negative
- Voluntary
- Involuntary
- Non-voluntary
Consent:
Consent means free, voluntary agreement, compliance or permission, which is legally valid. It must be given after understanding what it is given for, and of risks involved.
Implied consent:
When the conduct of a person is very much indicative that he is agreeable to some act or he desires the act to be done then it is implied that he has given consent for the act, even though he has not expressed his consent in words or letters.
Criteria of implied consent:
- Not written
- Proved by the demeanor of the patient
- Limited unto inspection, palpation, percussion & auscultation
- Legally effective or valid where proof is difficult.
Example:
- When a patient goes to a hospital or chamber to see a doctor
- When patient holds out his hand for an injection when doctors asks
Expressed consent:
Expressed consent is one, which is specifically stated in verbal or written manner –“I with my full consent want to undergo medical examination along with my private part, the results of which may go envious or against me”.
Consent becomes invalid when in the following cases:-
- The act is unlawful –criminal abortion
- Consent of minor less than 12 years
- consent of insane (mentally ill), intoxicated or if consent is taken under threat (section 90 bpc)
- Not informed consent
- Obtained by misinterpretation
- Consent of a female for sexual intercourse is invalid:-
- If the age of the girl is below 16 yrs
- Mentally retarded person
- Intoxicated person
- Obtained by fraud, force or fear of death
- Obtained after the act
- Necessary in an emergency treatment operation if no guardian is available or the patient is unable to give consent. (Section 92 BPC)
Consent related to age:
- If age is less than 12 years, consent should be taken from guardians
- If age is less than 16 years a girl cannot give consent for sexual intercourse
- If age is more than 12 years but less than 18 years, consent should be taken from both guardian and patient
- If age is more than 18 years, one can give valid consent for suffering any harm, which is done for benefit for him. (Sec-87 BPC)
Consent must be taken:
- Medico legal examination of the victim
- Before surgical operation
- Before giving anesthesia
- Before blood transfusion
- Before contraceptive sterilization
- Before radiotherapy
- Before any risky investigation for disclosing professional secrecy
- Clinical autopsy
- Human experimentation of drug
Consent is not needed:
- Medico legal autopsy
- Examination of the accused
- Compulsory vaccination
- Before any emergency operation
- Prevailed communication
- Manor-children less than 12 years
- Mentally ill person
- Comatose patient
- Loco Parentis
In emergency involving children, when their parents / guardians are not available, consent is taken from the person in charge. E.g. School teacher can give consent for treating a child who becomes sick during picnic away from home. Headmaster of a residential school
Legal procedure
There are 2 distinct aspect of law medicine relationship
- Forensic medicine
- Medical jurisprudence
Forensic Medicine:
It is a branch of medical science, which deals with the application of knowledge of all branches of medical science, whenever and wherever required for the purpose of law in both civil and criminal cases.
Medical Jurisprudence:
It medical jurisprudence can be defined as a science, which deals with the application of knowledge of law for the guidance of medical profession.
Aim – To find out the truth, help in justice and save the doctor.
Branches of forensic medicine:
- Forensic toxicology-deals with legal aspect of harmful effect of poisons
- Forensic pathology-deals with the dead body and fatal trauma to determine the cause and manner of death in case of sudden, suspicious, unexplained death
- Forensic dactylography-deals with fingerprint for the establishment of identity of individual
- Forensic radiology-deals with x-ray examination for determination age in various criminal cases, detection of cases, detection of fetus, diagnosis of head injury, etc.
- Forensic odontology-deals with teeth
- Forensic serology-deals of examination of blood and seminal staining
- Forensic thanatology-deals with medical and legal aspect of death
- Forensic psychiatry-deals with application of psychiatry for evolution in legal purpose
- Forensic ballistic-deals with the investigation of fire arms, ammunitions
- Forensic criminology-deals with crimes and criminals
- Forensic obstetrics-deals with normal and abnormal delivery
- Forensic osteology-deals with bones
The Legal System:
- Criminal law
It deals with offences, which are considered to be against the public interest, such as offences against the person, property, public safety, security of the state etc
- Civil law
It deals with disputes between 2 individual or parties.
Courts of Bangladesh:
It consists of –
- Supreme Court
Composed of
- Appellate division
- High court division
- Subordinate judiciary / district court
Appellate Division:
It has jurisdiction to hear and determine, appeal from judgments, decrees, order or sentence of high court division. It has rule making power for regulating the practice and procedure of each division and any court subordinate to it.
High court Division:
Though a division of Supreme Court, it is an independent court with its powers, functions and jurisdiction according to constitution.
Divided into three broad division—
- Civil court
- Criminal court
- Tribunal court
- Juvenile
- Nari-shishu
- Droto-bichar
- Administrative
- Labor
Civil Court:
The civil court system is more popularly known as subordinate judiciary. It is created under civil court act, 1887. It consists of
- District judge court
- Additional district judge court
- Sub-judge court
- Assistant judge court
Criminal Court:
- District session court
- Additional session court
- Assistant session court
- Courts of magistrate
- Specially empowered magistrate (1st class magistrate)
- 1st class magistrate
- 2nd class magistrate
- 3rd class magistrate
Powers are:
| 1st class magistrate: | Imprisonment not > 5 yearsSolitary confinement | Fine not > 10,000 taka |
| 2nd class magistrate: | Imprisonment for 3 years | Fine not >5,000 taka |
| 3rd class magistrate: | Imprisonment for 2 years | Fine less or equal to 2000 taka |
Punishment:
According to section 53 of BPC punishments are:
- Death sentence
- Imprisonment for life
- Imprisonment-
– Rigorous
– Simple
- Forfeiture of property
- Fine
Inquest:
An inquest is an inquiry or investigation into the cause of death. It is conducted in case of suicide, murder, killing by an animal or machinery, accidents, suspicious death and death due to anesthesia or operation.
Types of inquest:
- The police inquest:
This is the preliminary inquiry or investigation into the cause of all kinds of unnatural deaths by a police officer not below the rank of sub-inspector.
- The magistrate’s inquest:
This is preliminary inquiry or investigation conducted by a district magistrate, thana magistrate, magistrate of first class or any empowered magistrate to ascertain certain matters of fact
- Coroner’s inquest:
This is an inquiry conducted by coroner into the cause of any unnatural death within his territorial limits. In Bangladesh, it is invalid, in India this system is in force only in Mumbai.
Summons / Subpoena:
Summon is a document compelling the attendance in a court of law under penalty, on a particular day, time and place, for the purpose of giving evide
If the witness fails to attend the court:
- In a civil case, he will be liable to pay damages
- In criminal cases, fine or imprisonment
Conduct Money:
It is the fee offered or paid to a witness in civil cases at the time of serving the summons, to meet the expenses for attending the court.
Evidence:
Evidence may be defined all legal means which help to prove or disprove any matter in question in the court of law.
Types:
- Documentary
- Oral
- Documentary evidences
- Documentary evidence includes
- All the statements, which the court permits/requires to be made before it by witness, in relation to matter of fact under inquiry.
- Medical certificate includes ill health, insanity, age, death etc.
Medical certificate accepted in the court only when issued by registered medical practitioner.
Medico legal Reports:
It is a report prepared by doctor usually in criminal cases on requisition of law enforcement authorities. It consists of facts observed on examination & the opinion drawn from the facts. It is not accepted as evidence unless testified by doctor under oath. It is open for scrutiny of defense lawyers. Careless statement, superlative, exaggerated terms must be avoided.
Dying Declaration:
It is a written / oral statement of a person who is dying as a result of some unlawful act relating to the material factors of cause of his death on bearing on the circumstances.
Dying Deposition:
Is a statement of a person at oath, recorded by magistrate in presence of accused or his lawyer, who is allowed to cross-examine the witness.
Difference between dying declaration and dying deposition:
Dying declaration | Dying deposition |
Recorded by doctor | Recorded by magistrate |
No oath is necessary | Oath taking must |
Presence of accused or his lawyer is not necessary | Is necessary |
Inferior to dying deposition | Superior to dying declaration |
Oral Evidence:
It includes all statements, which the court permits / requires to be made before it by witness in relation to matters of fact under inquiry.
Types:
- Direct evidence
- Indirect evidence
- Hearsay evidence
Witness:
It is a person who gives evidence in the court of law, which helps to prove and disprove any matter in question.
Common witness:
It is a person who gives the evidence about the facts observed or perceived by him.
E.g. – In case of traffic accident, the person who witnessed the accident becomes the common witness.
Expert witness:
It is a person who has been trained or skilled in the technical or scientific subject and capable of drawing opinions and conclusion from the facts observed by him or noticed by others.
E.g. Doctor, firearm experts, finger print experts, hand writing experts etc.
Hostile witness:
Hostile witness is one who is supposed to have some interests or motive for concealing part of the truth or for giving completely false evidence.
Conduct of a doctor in a witness box:
In the court of law a doctor or a medical witness would be –
- Well prepared and take all records or relevant documents
- Well dressed and modest
- Stand up straight, relaxed or calm.
- Be confident , but not over confident or arrogant
- Use simple language, avoid superlative term
- Speak slowly, distinctly and audibly
Identification
Identification:
It is the determination of the individuality of a person based on certain physical characteristics which is unique to that individual.
It is necessary in case of:
- Living persons
- Recently dead persons
- Decomposed bodies
- Mutilated bodies
- Skeleton
- Criminal cases like murder, assault, rape.
- Civil cases like inheritance, passport, insurance claims.
Identification Data:
Includes-
- Age
- Race
- Sex
- Stature and general development
- External peculiarities such as moles, birthmarks, malformations, scars, tattoos, wounds, occupation marks
- Anthropometric measurements
- Fingerprints and footprints
- Teeth
- Dress, ornaments and other belongings in clothing, pockets or purse articles like diary, passport and letter.
Some criteria are used for identification of living person along with others.
They are-
- Handwriting
- Speech and voice
- Gait, tricks of manner and habit
- Memory and education
Corpus Delicti:
It is also known as the body of offence or the essence of crime. It means the facts of criminal offence, which establish that unlawful act in that place. The main part of corpus delicti is-
- the establishment of identity of the dead body
- infliction of violence
- in a particular way
- at a particular time and place
- by the person or persons charged with the crime
Sydney Shark Case:
In 08-April-1935, James Smith disappeared. After 14 days of his disappearance a shark was caught alive from aquarium where it vomited a human arm. Medical examination revealed that arm was severed from a dead body by sharp weapon. That arm was identified as Smith’s by a tattoo mark showing two men boxing.
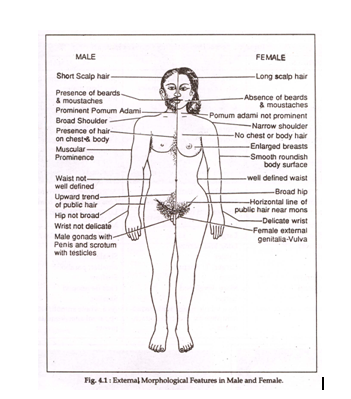
AGE:
Age of an individual can be determined from:
- Ossification of bone
- Teeth
- Secondary sexual characters
- General development in case of children
Secondary sexual characteristics:
Male:
- 14 yrs old – Pubic hair grows testis and penis enlarges
- 15 yrs old – Axillary hair grows
- 16 yrs old – External genitalia have an adult appearance
- 16-18 yrs – Facial hair begins to appear and voice becomes hoarse.
Female:
- 13-14 yrs – Pubic hair grows, labia develops and menstruation begins
- 14-15 yrs – Axillary hair grows
- 12-20 yrs – Breast development
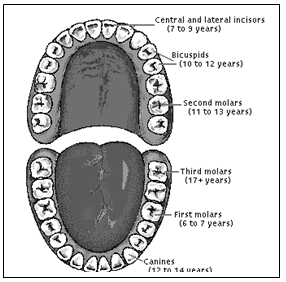
Teeth:
There are two sets of teeth:
- Temporary/Deciduous/Milk teeth – 20 in number
2i/1c/2m
- Permanent teeth – 32 in number
2i/1c/2pm/3m
| Features | Temporary teeth | Permanent teeth |
| Size and weight | Small in size and light in weight | Larger and heavier |
| Colour | China white | Ivory white |
| Incisors | Vertical | Slightly projected forward |
| Neck | More constricted | Less constricted |
| Ridge | Present in between neck and body | No ridge |
| Roots of molar | Smaller and more divergent | Larger and less divergent |
| Replacement | By permanent teeth | None |
Criminal responsibilityMedico-legal importance of Age
- Consent
- Competency as a witness
- Judicial punishment
- Rape
- Kidnapping
- Employment
- Marriage
- Attainment of majority
- Criminal abortion
- Impotence & sterility
- Identification
RACE:
Race may be defined as a biophysical concept denoting species or subspecies of human being usually united by a common heritage.
Types:
- Caucasian
- Mongoloid
- Negroid
Racial Difference:
| Trait | Caucasian | Mongoloid | Negroid |
| Skull | Rounded, medium headed | Square, short headed | Narrow & elongated, long headed |
| Cephalic index | 75-80 | 80-85 | 70-75 |
| Orbit | Triangular | Rounded | Square |
| Nasal Aperture | Elongated | Rounded | Broad |
| Palate | Triangular | Rounded | Rectangular |
| Limbs in proportion to body | Normal | Smaller | Longer |
| Complexion | White | Yellow | Black |
| Eye | Blue or grey | Black | Black |
| Teeth | Poorly spaced | Evenly spaced | Less parallel to each other |
| Hair | Straight or wavy hair coloured brown or reddish. | Dark, flat and course. | Black and woolly arranged in tight spirals. |
SEX:
Sex is one of the most important identification points of an individual. Sex can be determined from:
- Physical morphology, especially secondary sexual characteristics
- Bones
- Microscopic study of sex chromatins in cells
- Gonadal biopsy
- Hormonal study
Traits from skeleton:
The degree of accuracy in sexing adult skeletal remains is:
Entire skeleton – 100%
Pelvis alone – 95%
Skull alone – 90%
Pelvis + skull – 98%
Long bones – 80%
GENERAL:
| Trait | Male | Female |
| General size | Larger, more massive | Smaller and more slender |
| Long bones | Ridges, depressions and processes more prominent | Less prominent |
| Shaft | Rougher | Smoother, thinner and wider marrow cavity |
| Articular surface | Larger | Smaller |
| Weight | 4.5kg | 2.75kg |
PELVIS & HIP BONE:
| Trait | Male | Female |
| Pelvic brim | Heart | Circular |
| Shape of true pelvis | Conical | Cylindrical |
| Sub pubic angle | 50-60 | 80-90 |
| Obturator foramen | Large, oval | Small, triangular |
| Pre-auricular sulcus | Infrequent | Frequently deep |
| Acetabulum | Larger | Smaller |
| Ischio-pubic rami | Everted | Inverted |
| Ischial spine | Inverted | Everted |
| Sacral curvature | Uniformly curved anteriorly | Abruptly curved at last 2 segments |
| Sacral promontory | More projected anteriorly | Less projected |
| Sacral index | <114 | >114 |
Medico-legal Importance:
- Identification of a living or dead person
- Skeleton or isolated bones
- Hermaphrodites
- Concealed sex
- Heir ship
- Marriage
- Divorce
- Legitimacy
- Impotence
- Rape
- Paternity
Intersexes:
Intersexes means intermingling of features of both sexes in varying degrees in one individual stating conditions in which male and female characters such as gonads, physical form and sexual behaviours co-exist in various proportions. It results from some defect in the embryonic development.
Types:
- Gonadal agenesis
- Gonadal dysgenesis
– Turner syndrome
– Klinefelter’s syndrome
- True and Pseudo hermaphroditism
Medico-legal importance of intersex:
- Sports
- Service
- Admission to a school
- Medical negligence cases
- Inheritance or succession of property cases
- Nullity of marriage
- Very rarely with rape and other sexual offences
TATTOOS:
Tattoo marks are designs elicited by multiple small puncture wounds made through the skin with needle or similar presenting tools dipped in a dye.
Most common sites where tattoos are present: Arm, Forearm, Chest
Medico-legal importance of tattoo
- The identity of a person can be determined.
- Profession/occupation maybe determined.
- Social status also maybe determined.
HAIR:
Trichology is the subject that deals with the study of hair.
Parts: Hair consists of 2 parts
- Bulb/Root
- Shaft
Layers: Have 3 well defined layers
- Cuticle
- Cortex
- Medulla
Information can be derived from hair:
- Human or animal
- From what part of body derived
- Sex
- Accused hair /victim hair
- Cause of injury
- Age
Medico-legal importance of hair:
- Identification of the person involved in crime investigation
- Nature of weapon can be identified from the injury to the hair
- Age of person maybe determined from the growth of hair
- Sex maybe determined
- It helps in differentiating scalds from burns
- Poison can be detected in hair in case of arsenic poisoning
- Time of death can be determined
Dactylography:
Synonyms:
- Fingerprints
- Dermatoglyphics
- Dactyloscopy
- Henry-Galton system
Fingerprints are the impressions of patters formed by the papillary or epidermal ridges of the fingertips. One’s fingerprint is unique to that individual and it has been speculated that there is one chance in 64 billions of 2 persons having identical fingerprints. Further study of fingerprint is known as poroscopy.
Classification:
1. Loops – 67%
Radial
Ulnar
2. Whorls – 25%
Concentric
Spiral
Double spiral
Almond shaped
3. Arches – 6-7%
Plain
Tented
Exceptional
4. Composite – 1-2%
Central pocket loops
Lateral Pocket loops
Twinned loops
Accident
Medico-legal importance:
- Impressions left at the site of crime establish the identity of criminals
- Identification of suicides, deserters, persons suffering from loss of memory
- Identification in case of accidental exchanged of Newborn infants
- Prevention of impersonation
- To maintain identity of records
- Cheques, bank notes and other legal documents can bear a fingerprint
Superimposition:
It is the technique applied to determine whether the skull is of the person in photograph.
Points that are compared are-
- Eyes within orbital plate
- Nasion
- Prosthion
- Nasal spine
- Lower border of nose
- Jaws
- Zygomas below eyes
- Teeth
Other methods of identification:
- Palate print
- Lip prints
- Nose prints
- Congenital deformities
- Birth marks
- Occupation marks
- Pocket contents
Death:
Irreversible or permanent cessations of the three interlinked vital functions of the body are called death. Vital functions are-
- Circulatory system
- Respiratory system
- Nervous system
Together they are called – Tripod of life
Types of Death:
- Somatic Death:
Three functions are lost and life is still present in the component of body. Tissue is still responding to chemical and electrical stimuli. In short, somatic death is complete and irreversible stoppage of the vital functions.
- Molecular Death:
This is the death where life is not present in the component of the body. It means cessation of respiration and metabolism of body tissue, which is soon followed by autolysis and decay.
Medico legal Importance of Somatic Death:
- Issue death certificate
- Withdraw artificial maintenance
- Remove the organ for transplantation
- Dispose the body for disposal
BRAIN DEATH:
Means the patients is died, whether or not the function of some organs such as a heart beat is maintained by artificial means, and all the functions of the brain must have permanently and irreversibly ceased.
Types of Brain Death:
- Cortical or cerebral brain death:
This produces a vegetative state in which respiration continues, but there is total loss of power of perception by the sense. This state of deep coma can be produced by cerebral hypoxia, toxic conditions or widespread brain injury.
- Brain stem death:
Where the cerebrum may be intact, through it has been cut off functionally by the stem lesion. This can be produced by raised intracranial pressure, cerebral edema, intracranial hemorrhage etc.
Brain stem death consist of –
- Deep unconsciousness with no response to external stimuli or internal need
- No movements, no spontaneous breathing
- Cessation of spontaneous cardiac rhythm without assistance
- No reflex
- Bilateral dilatation and fixation of pupils
- Flat iso-electric EEG
Cause of Death:
- Immediate Cause: The pathological process which lead to death The diseases or injury responsible starting the sequence of events, which are brief or prolonged that lead to death
- Basic Cause: Pathological process responsible for death at the time of terminal event or prior to or leading to the event
- Contributory Cause
Manner of Death:
Manner of death is the way in which cause of death was produce. The manner of death can be
- Natural: If the death occurs exclusively from disease
- Unnatural or violent: If the death occur exclusively by injury or is hastened due to injury in a person suffering from natural disease
Agonal Period: It is a time between a lethal occurrence and death.
Mode of Death:
According to Bichat, there are 3 modes of death, depending on whether death beginning one or other of the 3 system, irrespective of what the remote cause of death. These modes are-
- COMA- Failure of the nervous system
- SYNCOPE- Failure of the circulatory system
- ASPHYXIA- Failure of the respiratory system
Coma:
It is a state of unarguable unconsciousness determine by the absence of psychologically understandable response to external stimuli or inner need.
Cause:
- Compression of the brain
- Drugs
- Metabolic disorder and infection etc
Autopsy: Injuries or disease of the brain may be present. The lungs, brain & the meanings are congested, splanchnic pooling of the blood occurs
Syncope:
Syncope is silent stoppage of action of heart, which may prove fatal.
Cause:
- Anemia due to sudden and excessive hemorrhage
- Asthenia
- Vagal inhibition
- Exhausting disease
Autopsy: The heart is contracted and the chambers are empty when death has occurred from anemia, but chambers contain blood when death occurs due to asthenia
Asphyxia:
Asphyxia is a condition caused by interference with respiration or due to lack of oxygen is respired air, due to which the organs & tissues are deprived of oxygen, causing unconsciousness or death.
Type and cause:
- Mechanical: In this the air passage are block mechanically.
- Pathological: Infective condition & new growth of the lungs or in the respiratory tract
- Toxic condition
- Trauma
- Postural asphyxia
- Iatrogenic
Symptoms of asphyxia:
- Stage of dyspnoea: increased carbon dioxide in the blood causing respiratory stimulation
- Stage of convulsion: carbon dioxide level further increased
- Stage of respiratory exhaustion: the respiratory centre is depressed.
Asphyxial stigmata
Asphyxia is not a pathological entity and can not be clearly recognized from morbid anatomical findings along the triad of:
- Cyanosis
- Facial, palpebral, bulbar, sub pleural & subepicardial petechae
- Visceral congestion
All are due to raised venous pressure.
Autopsy:
- External:
- Post-mortem lividity is marked
- Face is cyanosed
- Tongue is protruded
- Frothy & bloody mucus escapes from the mouth & nostrils
- Pupils dilated
- Tardieus spot
- The blood is dark & fluid
- The right side of the heart is full whereas the left side is empty
- The larynx & trachea are congested.
- Lungs congested & edematous
- Tardieus spot under the mucus membrane of organ
- Internal:
CHANGES AFTER DEATH:
- Immediate Changes (somatic death)
- Insensibility & loss of voluntary power
- Cessation of respiration
- Cessation of circulation
- Insensibility & loss of voluntary power
- Early changes (cellular death)
- Changes in the skin
- Changes in the eye
- Primary flaccidity of muscles
- Cooling of the body
- Post-mortem lividity
- Rigor mortis
Post mortem Caloricity:
The post mortem rise of temperature in certain cases is known as post mortem caloricity.
Due to – septicemia condition, Cholera, Heat stroke
Post-mortem Lividity:
It is also called
- Post mortem staining
- Subcutaneous hypostasis
- Livor mortis
- Cadaveric lividity
Medicolegal importance of PM Hypostasis:
- It is a reliable sign of death
- Helps in estimation of the time since death
- It indicates the posture of the body at the time of death and any movement after death
- It may indicate cause of death from its color
- In asphyxial death: Bluish, violet, purple
- In CO poisoning: cherry red
- In burn: bright red
- In phosphorus poisoning: dark brown
- Exposure to cold water: pink red
- In hemorrhage, anemia, wasting disease: very slight staining due to reduced amount of blood pigment
Rigor Mortis:
Rigor mortis is the state of stiffening of muscle with slight shortening of muscle fiber. It is also known as death stiffening, cadaveric rigidity. Individual cell death occurs in this stage.
It begins 1-2 hrs after death and takes further 1-2 hrs to develop. It may also begin in 3-6 hrs. Usually it lasts for 24-48 hrs in winter and 18-36 hrs in summer.
Condition altering the onset & duration:
- Age
- Nature of death
- Muscular state
- Atmospheric condition
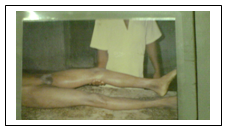
Conditions Simulating Rigor Mortis:
- Heat stiffening: When body is exposing to temperature 65° C, it is seen in death from burning, high voltage electric shock and from falling into hot liquid
- Cold stiffening: When body is exposing to freezing temperature
Medicolegal Importance of Rigor Mortis:
- It is the sign of death.
- It extent help in estimating time of death, which is not reliable
- It indicates the position of the body at the time of death.
Cadaveric spasm: It occurs specially in cases of sudden death, excitement, fear, severe pain, exhaustion, cerebral hemorrhage, injury to nervous system, firearm wound of the head, conversant, poison etc.
LATE CHANGES OF DEATH:
- Putrefaction (decomposing)
- Adipocere formation
- Mummification

PUTREFACTION:
It is the process by which the complex nitrogenous substances in the body are converted into simpler one by the action of photolytic enzymes of the tissue and living saprophytic microorganisms. It is the surest sign of death.
Causes of putrefaction:
- Autolysis
- Living saprophytic micro-organisms
Organisms involved in putrefaction:
- Clostridium welchii
- Streptococcus
- Staphylococcus
- E.coli
They are mostly anaerobic and live in the intestine.
Characteristics features of putrefaction :
- Color change
- Development of foul smelling gasses
- Liquefaction of tissue
Medico Legal Importance of Putrefaction:
- It is the surest sign of death
- The different stage of putrefaction indicates the time since death
- Advance putrefaction obliterates the identity of deceased and the cause of deceased
ADIPOCERE:
It is the modification of putrefaction in which the body fat is converted into a brown waxy like substance occurs in bodies submerged under the water or buried in a moist grave or water lodged soil
Properties:
- Offensive
- Sweetish smell
- Ammonia like odor
- Olfactory adaptation occurs within two minutes
Medico legal Importance:
- The features of adipocere in face are well preserved that helps to establish the identity
- The cause of death can be determined because injuries are recognized
- The time since death can be estimated
Mummification:
It is the drying of the body tissue due to rapid dehydration of the body in a dry or hot climate preserving the natural appearance of the body
Factors necessary for Mummification:
- Absence of moisture in the air
- Continuous action of the dry and warm air
- Characteristics of Mummification
- Loss of weight
- Thin
- Stiff
- Brittle
- Odorless
Medico legal Importance of Mummification:
- The features in face are well preserved that helps to establish the identity
- The cause of death can be determined because injuries are recognized
- The time since death can be estimated
- Estimation of Time of Death
- Time since death condition of the body
SUDDEN DEATH:
Death is said to be sudden or unexpected when a person not known to have been suffering from any dangerous disease , injury or poisoning is found dead or dies within 24 hrs after the onset of terminal illness.
Causes:
- Disease of CVS
- Disease of Respiratory system
- Disease of CNS, GIT, genitourinary system
- Miscellaneous –Addison’s disease, DM etc
Exhumation:
It is the digging out of an already buried body from the grave.
Autopsies are performed on exhumed bodies:
- In criminal cases, such as homicide, suspected homicide distinguished as suicide, suspicious poisoning, and criminal negligence.
- In civil cases, such as accidental death claim, insurance, workmen’s compensation claim, liability for professional negligence, survivorship & inheritance claims or disputed identify.
Mechanical injury:
Wound:
It may be defined as disruption or dissolution of the anatomical continuity of the tissue out of the body irrespective of breach of continuity of skin because of blunt trauma.
Injury:
It is defined as any harm what so ever illegally cause to any person in body, mind, reputation or property.
MECHANICAL INJURIES are injuries produced by physical violence.
TYPES: a) Due to blunt force>1. Abrasion
2. Bruise
3. Laceration
4. Fracture & Dislocation
b) Due to sharp force>1. Incised wound
2. Chop wound
3. Penetrating wound
c) Firearms & bomb blast injuries
Abrasions:
It is a destruction of the skin, which usually involves the superficial layers of the epidermis only.
Character:
- Bleeds slightly
- Heals rapidly
- Leaves no scar
- Have 2 dimensions – length, breadth, no depth
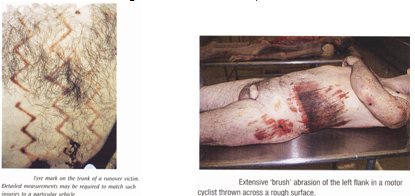
Types:
- Scratches -very superficial. I.e. by nails, pins etc.
- Grazes -common in RTA.
- Pressure -I.e. strangulation mark, bite mark.
- Impact -caused by impact to any rough surface.
Age of abrasion:
- Fresh : bright red
- 12 to 24 hours : lymph and blood dries up leaving a bright scab
- 2 to 3 days : reddish brown scab
- 4 to 7 days : epithelium grows and covers defects under the scab
- After 7 days : scab dries
Medico legal importance:
- Site of impacts
- Identification of object
- Time of injury
- Cause of injury
- An abrasion on the neck may indicate throttling, hanging or strangulation.
- An abrasion around the nose and mouth indicate smothering.
- If found on the breast genitals inside of the thigh and around the anus indicate sexual assault.
Bruises:
It is defined as subcutaneous rupture of blood vessels and effusion of blood into the tissue, caused by blunt trauma.
Factors modify the appearance of bruise:
- Site of injury – bruising occurs more easily in areas overlying bone where the tissue is lax
- Vascularity – greater the vascularity, greater the bruising
- Age – children and old people bruise more easily
- Sex – in obese women bruise is most easily
- Natural disease – diseased vessels
- Shifting – bruise does not always appear at the site of impact
Age of the bruise:
- Initially : reddish
- Few hours to 3 days : blue (due to haemosiderin)
- 4 to 6 days : become greenish (due to haematoidin)
- 7 to 12 days : yellowish (due to bilirubin)
- 2 weeks : normal
Medico legal importance:
- Patterned bruises may connect the victim and the object or weapon
- Age of the injury can be determined by color change
- Degree of violence may be determined from the size
- Character and manner of injury may be known
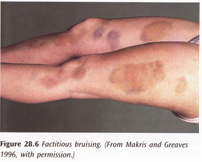
DIFFERENCES BETWEEN HYPOSTASIS & BRUISE:
| Trait | Hypostasis | Bruise |
| Cause | Distension of vessel with blood in the dermis | Effusion of blood due to rupture of blood vessels |
| Site | Dependent parts of the body | Anywhere of the body |
| Appearance | No elevation | Often swollen |
| Epidermis | Not abraded | May be abraded |
| Margins | Clearly defined | Merge with surrounding area |
| Color | Uniform bluish purple | Old bruises are of different color |
| Incision | Shows no extravasated or clotted blood | Shows extravasated or clotted blood |
| Pressure effect | Absent | Present |
Laceration:
It is the splitting or tearing of the skin by blunt impact and occurs most commonly over bony prominences where the skin is crushed and split against the bone.
Types:
- Split/incised looking wounds – It occurs usually when the impact is perpendicular. Sites are-Flexed elbow, knee lateral and medial malleolus, sacral region and ankle
- Scratch – This is occurred due to angulated impact. It produces a flap indicating the direction of force.
- Avulsion – When horizontal impact is done the skin is separated from the depart tissues and this is called degloving injury. Sites are-Scalp, Lower and upper limb
- Tear – It is due to impact against irregular object.
Characteristics of Laceration:
The edges are irregular ragged and uneven
- The deeper tissues are unevenly divided
- If there are any hair bulbs, they will be crashed
- Blood vessels are crashed also. These resulting less external hemorrhage
- Foreign material is usually found in the wound – so preservation of wound is very important
- Generally there is no relationship between the shape and size of the wound and the weapon producing it
Medico legal Importance:
- The type of laceration may indicate the cause of injury and the shape of blunt weapon
- The age of injury can be determined
- Foreign body found in the injury indicate the circumstances in which the crime has been committed
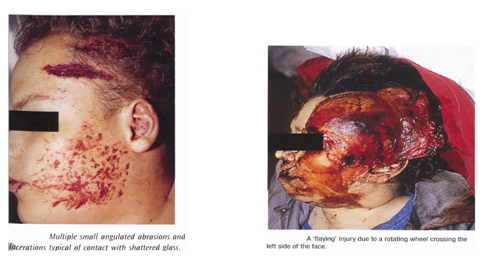
Incised wound:
It is a clean cut through the tissue caused by a weapon with a sharp cutting edge and its length is greater than the depth.
Characteristics:
- Edge is clean cut, well defined and usually averted
- There are some exceptions in the scrotum and neck where there is inverted the wound. Because muscles are inserted into the skin so inversion occur (plasma and dartos muscle)
- Length is greater than depth
- There is no busing inside the edge of wound
- Blood vessels are cut across
- Bleeding is profuse
- There is a tendency to gape due to retraction of muscle fibers
Age of incised wound:
- Fresh : hematoma formation
- 12 hours : the edges are red, swollen and adherent with blood and lymph;
leucocytic infiltration
- 24 hours : a continuous layer of endothelial cells covers the surface
- 36 hours : the capillary network is complete
- 48 to72 hours : epidermal cells invade the space where connective tissue has finally
developed.
- 3 to 5 days : definite fibrils running parallel to the vessels are seen
- 1 to 2 weeks : scar tissue is formed.
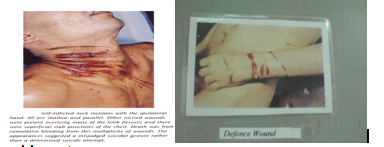
Medico-legal importance:
- They indicate the nature of weapon (sharp-edged)
- They give an idea about the direction of the force
- The age of the injury can be determined
- Position and character of wounds may indicate mode of production i.e., suicide, accident, homicide.
DIFFERENCES BETWEEN Laceration (Incised looking wound) & Incised wound
| Trait | Laceration (Incised looking wound) | Incised wound |
| Production | Blunt objects | Object with sharp cutting edge |
| Site | Usually over bony prominences | Anywhere |
| Shape | Usually regular | Linear or spindle shaped |
| Margins | Irregular | Clean cut and everted |
| Dimensions | Variable | Longer than deep but often gaping |
| Hair and blood vessels | Crushed | Clean cut |
| Hemorrhage | Not pronounced. Exception scalp. | Usually profuse |
| Surroundings | Abrasion and bruising usually present. | Abrasion and bruising not present |
| Foreign bodies | Frequently present | Normally free from foreign bodies |
Hurt:
It is whatever the causes bodily pain, disease on infirmity is said to cause hurt.
Types– Simple and Grievous
Simple hurt:
It is neither serious nor complicated and heals up easily without leaving permanent disfiguration or deformity.
Grievous Hurt:
- Deprivation of the male from masculine vigor- It generally means cutting of the male organ
- Permanent privation of the sight of either eye
- Permanent privation of the hearing of either ear
- Privation of any member (functional unit) or joint
- Destruction or permanent impairing of the power of any member or joint
- Permanent disfiguration of the head or face
- Fracture or dislocation of any bone or tooth
- Any hurt which endangers life or which cause the sufferer to be during the space of 20 days in severe bodily pain or unable to follow his/her ordinary pursuits
Stab or punctured wound:
Produced from penetration of pointed instrument such as knife, dagger etc
Type : – Penetrating wound (depth > length)
– perforating wound
Other wounds:
Concealed puncture wounds: Occurs in concealed part of the body such as nostrils,
fontanella, fornix of the upper eyelids, axilla
Defense wounds: Reaction of the victims to save him (by raising arm &
grasping weapon)
Self inflicted wounds: – By a person in his own body
– Motive to draw attention
Fabricated or false wounds: – By a person in his own body or by another person with his
consent
– Motive to implicate someone
Cause of death
* Homicide
* Suicide
* Accident
REGIONAL INJURIES:
Injuries occur at various parts of the body. So they are classified as regional injuries according to site of injuries for better investigation and description.
Sites of regional injuries:
- Head and Spine
- Chest
- Abdomen
- Limb
Head Injuries:
Head is the most vulnerable site of injury because –
- It is the heaviest part of the relative to its size.
- It is poised on the spine in a rather unstable position.
Sites:
- Scalp
- Face
- Skull
- Intracranial
- Brain
- Blood vessels
- Meninges
Scalp Injuries:
Layers: Superficial to deep → Skin, connective tissue, Galea aponeurotica, loose connective tissue, pericranium
Injuries may occur –
- Abrasion – But due to presence of hair on the scalp, abrasions may not be well observed.
- Bruise – Bruises over the scalp are associated with prominent edema. They are better felt than seen.
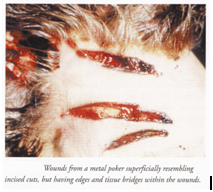
- Laceration – Laceration over the scalp is associated with localized swelling and extensive bleeding, hematoma formation beneath the scalp. It resembles incised looking wound.
- Incised wound – The appearance of laceration on scalp and on incised wound can be distinguished during observation by a magnifying glass.
- Avulsion – Avulsion of a large area of scalp can occur e.g. In road traffic accident, if hairs become entangled in machinery
Face Injuries
Types :
- Abrasion
- Bruise
- Laceration
- Incised wound
Periorbital Bruising: It is also known as ‘Black Eye’ or, ‘Spectacle Bruise’. Fracture of facial bones can also occur, e.g. – fracture of Periorbital bones by a blow or punch.
Cause:
- Direct Trauma
- Injuries to the front of the scalp
- A fracture of the base of the scalp
Skull Injuries:
Fracture: May be simple or compound fracture
Types:
- Fissured fracture
- Comminuted fracture
- Depressed fracture
- Pond fracture
- Gutter fracture
- Ring fracture
- Perforating fracture
- Sutural fracture
- Crush fracture
- Coup fracture
- Contre-coup fracture
All these fractures are generally caused by –
- An object in motion striking the head
- Head in the motion striking the object
- Fall from a considerable height on feet or buttock
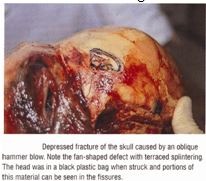
Intracranial Injuries:
- Intra-cranial hemorrhages
- Injury to brain
Complications of Intracranial Injuries
- Meningitis
- Subdural Abscess
- Cerebral abscess
- Delayed meningitis
- Cerebral softening
- Dissecting aneurysm
- Arteriovenous fistula
- Post traumatic epilepsy
- Post traumatic encephalopathy
- Post traumatic tumor (Meningioma)
- Physical, psychic and circumstantial disability
Intracranial Hemorrhages
Epidural hemorrhages:
- Nature: Traumatic
- Vessels involved: Middle meningeal artery.
- Associated fracture: Seen in 85% cases
- Importance
It is a space occupying lesion. The blood is not encapsulated & may not be absorbed for a long period
↓
Thus a chronic state is developed
↓
The patient / injured person may experience a temporary concussion
↓
Recovery (Lucid state)
↓
Raised intracranial pressure due to bleeding
↓
Patient become unconscious again
Subdural hemorrhage:
- Nature: Traumatic
- Vessels involved: Communicating veins in Subdural space, cortical veins & venous sinuses
- Type: a) Acute
b) Sub acute
c) Chronic
- Associated fracture: May not be found
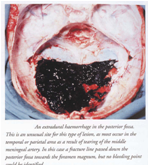
Subarachnoid hemorrhage:
- Natural:
a)Due to rupture of Berry aneurism of circle of Willis in young individual
b)Due to degenerative change of blood vessels in old individuals
- Traumatic:
a)Asphyxia
b)A heavy blow on the side of the neck below the ear causing rupture of vertebral artery in posterior cranial fossa. This responsible for ‘Punch-drunk Syndrome’
Intracerebral hemorrhage:
- Nature: a) Pathological
b) Traumatic
- Cause:
a)Degenerative changes to blood vessels
b)Blood dyscrasias
c) Neoplasm
d)Hypertension
e) Blow on the head
Apoplexy:
Continuous intracranial hemorrhage is known as apoplexy. It is generally found in pathological states.
E.g. – HTN, atherosclerosis, aneurysm
Injuries to Brain:
- 1. Cerebral contusion: If cerebral cortex still remains in its shape but is bruise and swollen, it is called cerebral contusion. It may occur with or without any injury.
- 2. Cerebral Laceration: When the mechanical separation of brain tissue is seen in naked eye
- 3. Coup Lesion: When mobile head is struck with object, the site of maximum cortical contusion is most likely to be beneath the site or at least at the same site of the blow.
- 4. Contrecoup lesion: When a moving head is suddenly decelerated, as in a fall on the back of the head, there is often cortical damage on the opposite side of the brain. This is known as Contrecoup lesion.
- 5. Concussion of Brain: Concussion is a state of temporary unconsciousness due to partial/ complete paralysis of cerebral function, due to head injury, is always followed by amnesia & tends to spontaneous recovery
Medico legal relevance: Concussion may be followed post-concuss ional state like headache, dizziness, nervousness, retrograde amnesia, nausea, vomiting, insomnia, mental irritability and automatism.
Diffuse Axonal Injury:
It is a clinical condition, in which there is diffuse injury of the axons with immediate loss of consciousness and coma for more than 6 hours.
Features of DAI:
- A focal lesion in corpus callosum and mother midline structures
- A focal lesion on rostral brainstem
- Microscopic evidence of numerous axonal swellings and axonal bulbs, after 12 hours if injury.
Cerebral Edema: This is most common cause of raised intracranial pressure. It is found in intracranial injuries.
Cause of death in brain injury:
- Raised intracranial pressure hematoma, contusion, laceration, infarction or swelling
- Diffuse axonal injury
- Ischemic brain damage
- Fat embolism
Chest Injuries:
- Non-penetrating injuries
- Penetrating injuries
- Rib fracture: Multiple rib fracture resulting in ‘Flail Chest’ which is characterized by paradoxical respiration.
- Stab wounds to heart, lungs, pleura, and other thoracic viscera
- Gun shot injuries
- Penetrating injuries to thoracic viscera by fractured ribs
Complications of chest injury:
- Pneumothorax
- Haemothorax
- Chylothorax
- Interstitial emphysema
- Cardiac temponade
- Air embolism
- Intraparebchymal hemorrhage
- Infection
- Death
Injuries to Vertebral Column & Spinal Cord:
Vertebral Column:
- Vertebral dislocation
- Fracture of spines, transverse processes and laminas
- Rupture of intervertebral disc
Spinal Cord injuries:
- Contusion
- Laceration
- Compression
- Complete section
Complications:
- Temporary and permanent paralysis of limbs & other parts of body
- Alterations of sensations
- Headache, dizziness, restlessness, insomnia
- Death
Abdominal Injuries:
- Non-penetrating or closed
Cause:
- Blunt force injury
- Falling from a considerable height
- Traffic accident
Structure involved:
- Liver
- Spleen
- Kidney
- Intestine
- Abdominal wall
- Mesentery
- Pancreas
- The Diaphragm
- Penetrating or open
Cause:
- By cutting or stabbing weapon
- by firearm
- by horns or claws of animals
- By falling on sharp projecting object
Structure involved:
- The diaphragm
- Spleen
- Liver
- Stomach
- Intestine
- Abdominal muscles
Type of Injury:
- Bruise
- Laceration
- Tearing of hollow viscera
- Rupture of viscera like liver, kidney, adrenal gland
Injury to Genitalia:
Female:
- Laceration of vulva or vagina due to assault or during delivery
- Gravid uterus may be ruptured by blow, kick, trampling on the abdominal wall
Male:
- Penis may be injured by a squeeze or crush
- Penile amputation
- Crushing of testes
Limb Injury:
Types:
- Abrasion
- Contusion
- Deep lacerated wound
- Fracture or dislocation of joints
- Complete amputation
Cause:
- Road traffic accident
- Falling from height
- Violence
FIREARM INJURIES
FIREARM: A firearm is an instrument or device with which it is possible to propel a projectile by the expensive force of gases generated as a result of combustion of the propellant in a closed space.
CLASSIFICATION:
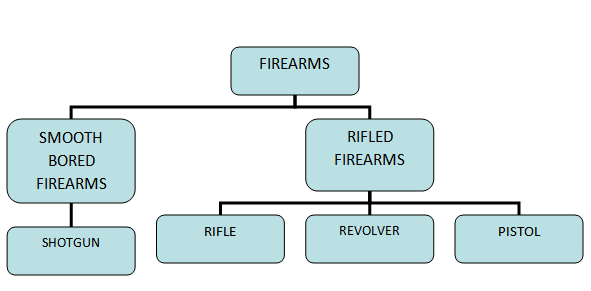
Parts of a Firearm:
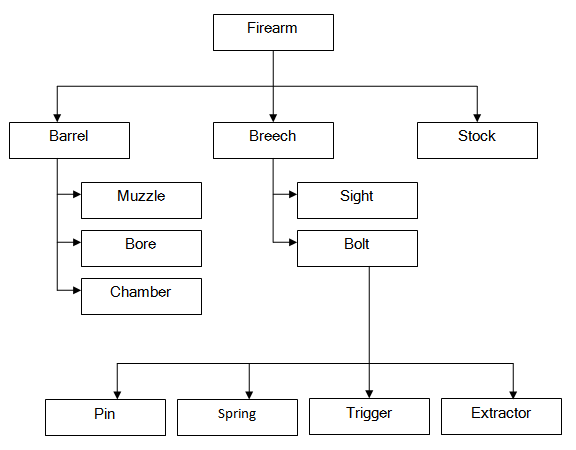

Cartridge:
A shotgun cartridge contains
- A case
- Primer cap
- Primer
- Gunpowder
- Card disc
- Felt wad
- Card disc
- Shot
- Card disc
A rifle cartridge has:
- Case
- Primer
- Gunpowder
- Shot/bullet
- Jacket
Primer: Chemical mixture used for detonation of the gunpowder
Gunpowder
Black
Smokeless
Semi-smokeless
Rifling:
Narrow spiral grooves running through whole length of the barrel. It provides the bullets spinning motion. This spiral motion helps bullet to overcome the air resistance and as well as more penetrating power.
Choking:
Some smooth barreled guns have narrowing at the distal end of their barrel near the muzzle. This is called choking. This prevents spreading of pellets as they leave the barrel.
Mechanism of Bullet Wound Production:
- Bullet velocity – a bullet ability to wound is directly proportional to its kinetic energy at the moment of impact
- Type of tissue density
- Hydrostatic force
Factors which Modify the Characteristic of Firearm wound:
- The range of firing from which the weapon is discharged
- The size of the shot
- The nature of the explosives
- Type of gun
Types of wounds:
- Contact wound / shot
- Close range wound / shot
- Intermediate range wound / shot
- Distance range wound / shot
Shot Gun:
- Flame extend up to15-20 cm (5”-7”)
- Smoke up to- 30cm
- Unburnt / partially burnt powder grain up to- 60 to 90cm
- Cards travel 2 meters
- Wad travels2-5 meters; wadding produce minor injury up to 3 meters
- At about 30 meters pellet only penetrate skin or muscle
- Death beyond 30 meters is rare
Contact wound:
Single, round or oval; often ragged
Margin of the skin-charred; abraded border usually soiled with powder residue
Muzzle impression found
Close range:
Up to 30cm
Hair are singed
Blackening; tattooing; Smudging / fouling
Wound –single, circular or oval; skin margins-clean cut / ragged; annular bruising
Felt/wad or plastic cups found in the depth of the wound
Deeper tissue show marked disruption
Up to 60-90cm:
Single irregular circular aperture (2.5cmor less) with irregular lacerated edges
No burning/blackening; slight tattooing may present
Scorching
Shot are scattered after entering & causing much damage to the internal tissue
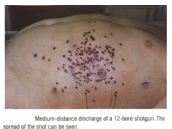
Rifled Firearm:
- Flame extend up to- 8cm (revolver/pistol); 15-20 cm (rifle)
- Smoke up to- 30cm
- Unburnt / partially burnt powder grain up to- 60 to 70cm
- At about 200- 300 meters explosive effect (spin effect with intense liberation of energy is similar to that of an explosion) & severe lacerated exit wound (2.5cm to palm size)
- In wounds in head within 300meters: Brain pulped & greater part of cranium slashed into fragments
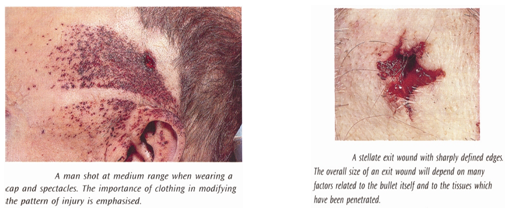
Bomb explosion wounds:
Bomb: It is container filled with explosive mixture and missiles, which is fired by either detonator or fuse.Effects of bomb blast
- Disruptive effect
- Burns
- Air blast
- Flying missiles
- Falling masonry
- Fumes
Investigation of a bomb blast case:
- Whether the explosion was caused by a bomb
- Identification of death
- Number of dead person
- Cause of death
- Circumstances of death
SEXUAL OFFENCE:
DEFINITION: Sexual offences are sexual intercourse or sex related act performed in a way that is against the provisions of the laws of the land. These are acts of illegal intercourse with a second person or with an animal to obtain sexual gratification.
CLASSIFICATION:
- Natural sexual offences
- Unnatural sexual offences
- Sex linked offences
RAPE:
Unlawful sexual act by a man with a woman with or without her consent when she is below 16 years , without her consent at and above 16 years, against her will or with her consent when it has been obtained by unlawful means- putting her in the fear of death or hurt, fraud(misinterpretation of fact),impersonation, intoxication, or mentally impaired.(Section 375, Penal code).
EXAMINATION OF A RAPE VICTIM
PREREQUISITES:
- Requisition from a police officer not below the rank of sub-inspector or the magistrate
- Identification of the victim by accompanying constable
- Three copies of attested photograph
- Informed written consent of the victim(Major) or her legal guardian(Minor)
- A female attendant
HISTORY:
- History of occurrence of rape(date, hour, place, name of accused, capacity to resist, level of consciousness)
- History of menstruation, marital status, previous sexual intercourse.
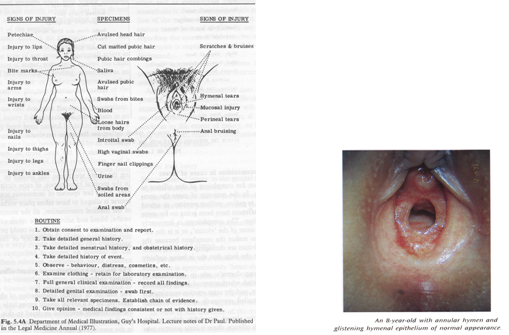
EXAMINATION:
- Examination of clothing
- General examination of the victim
- Examination of private parts of the victim; i.e.-vulva, hymen, fourchette, vagina
- Mental status of the victim
- X-ray of joints to determine the age of the victim
INVESTIGATION: Chemical examination of semen to detect the accused.
REPORT PREPARATION: Report about any recent violence and sexual intercourse.
SODOMY:
It is the anal intercourse between two males or between a male and a female. It is also called buggery.
It can be homosexual or heterosexual in nature and any degree of penetration just into the anal margin is punishable by law and proof of Emission Is not required.
When the act is performed with the consent of the passive agent, both are liable for punishment, but only the active agent is punished when the offence is committed without consent.
General Procedure of Passive agent examination:
The routine medical examination of the passive agent of sodomy should be carried out as is done in an alleged case of rape. The specific history of the passive agent should include:
- The date, time and place of alleged act.
- The position in which sodomy was performed.
- Details of struggle or resistance.
- Use of any lubricants.
- Degree of penetration and ejaculation during the act.
- Any pain or bleeding during or after the act.
- Whether the anal area was washed or bathed after the act.
TRIBADISM: Female homosexuality is known as tribadism.
BESTIALITY: It is the sexual intercourse by a man being with a lower animal.
SEXUAL PERVERSION:
Sexual Perversions are persistently indulged sexual acts or fantasies in which complete satisfaction is sought and obtained without sexual intercourse.
The perverted behavior is usually a repulsive and cruel form of tension release under the act of compulsion.
Mental state of the accused should be determined in all such cases by a psychiatrist
SADISM :
Sexual gratification is obtained or increased from the acts of physical cruelty or infliction of pain upon ones’ partner.
LUST MURDER :
Here murder serves as stimulus for the sexual act, the act being accompanied by erection, ejaculation and orgasm.
FETISHISM :
This is the use of objects to obtain an orgasm; the object being a part of the body of a woman or some article belonging to her such as thongs, underwear, brassiere, G-strings, etc. This behavior is seen almost exclusively in males.
URANISM :
Sexual gratification by fingering, fondling, licking, nibbling, etc.
PARAPHILIAS :
Unorthodox sexplay by using objects or parts of the body.
STUDY OF DATURA:
Datura is a stupefying poison.

ACTIVE PRINCIPLES: It includes alkaloids like-
1. Hyoscine
2. Hyoscyamine
3. Atropine
FATAL DOSE: 100-125 crushed Datura seeds
FATAL PERIOD: 24 hours

SIGNS & SYMPTOMS: According to Morton-
- Dry as a bone: Dryness of mouth, dysphagia, difficulty in talking.
- Red as a beat: Flushing of face.
- Blind as a bat: Dilated pupils, loss of accomodation, blurring of vision
- Hot as a hare: Dry, hot skin, lack of sweating
- Mad as a wet hen: drunken gait, delirium, drowsiness.
Ludiculous movement: The patient picks at his clothes, pulls imaginary thread from his nail & threads imaginary needle.
MEDICOLEGAL IMPORTANCE:
- It is a deliriant poison.
- It is also known as street poison as it is used by criminals to stupify a person prior to robbery, rape or kidnapping.
- It is rarely used for homicidal purpose.
- It is not used for suicidal purpose.
- Accidental poisoning may occur in children.
Study of Cannabis:
It is also known as Indian hemp, Hashish, Marihuana, Pot, Dope, Grass, Weed, Hash, Mary jone, M.J., Bhang. All parts of the plant, male or female, contain the active material, except stem, root and seeds.
FORMS:
1) Bhang (siddhi. Sabji)
2) Majoon.
3) Ganja.
4) Charas and
Hashish

Signs & Symptoms:
In small dose:
1) Euphoria
2) Followed by narcosis
3) patient is pleased with himself
4) felling of cheerfulness and wellbeing
5) Increase talkativeness
6) Increase appetite.
Larger dose:
a) Loss of perception of time & place.
b) Visual hallucination of erotic nature.
c) person will see beautiful nude women dancing and singing.
d) stage of narcosis:
- i. Gidines
- ii. Confusion
- iii. Ataxia
- iv. Tingling and numbness of extremities
Fatal dose: Charas 2 g. ganja 8 g.; bhang 10g./ kilo bofy weight. THC 30 mg/kg.
TREATMENT
1) Stomach wash
2) Mixture injection IV containing glucose and sodium.
3) Usual diazepum
4) Assurance of patient
5) Angiolytic drugs
6) Psychotic drug.
STUDY OF OPIUM
Opium (afim) is the dried juice of unripe poppy capsule.
How opium is collected?
The unripe capsule is incised and the white juice which exudes is collected and allowed to evaporate to obtain crude opium.

Alkaloids:
- The phenanthrenes: Morphine (10%), Codeine (0.5%), Thebaine (0.3%)
- The isoquinoline group: papaverine (1%), narcotine (6%)
Classification:
- Natural : Morphine, Codeine
- Semi-synthetic: Heroin, Oxymorphone
- Synthetic: Meperidine, Methadone
Fatal Dose: Opium 2 g morphine 0.2 g; codeine half g.
Signs and symptoms:
Stage of Excitement: Increase sense of well-being, increased mental activity, freedom from anxiety, talkativeness, restlessness, hallucinations.
Stage of stupor: Headache, vomiting, incapacity of exertion, giddiness and drowsiness.
Stage of coma: Deep coma, muscles are flaccid and relaxed and all reflexes are abolished. pale face, and conjunctivae congested, pinpoint pupil.
DIFFERENTIAL DIAGNOSSIS:
| (1) OPIUM POISONING | (2) ACUTE ALCOHOLIC POISONING |
| (3) BARBITURATE POISONIG | (4) CARBOLIC ACID POISONING |
| (5) CARBON MONOXIDE POISONING | (6) EPILEPTIC COMA |
| (7) URAEMIC COMA | (8) DIABETIC COMA |
| (9) HYSTERICAL COMA | (10) CEREBRAL COMA |
MEDICO-LEGAL IMPORTANCE:
(1) suicides because death is painless
(2) poisoning may occur in addicts
(3) cattle poisoning
(4) it is sometimes used for doping race horses
(5) Sometimes opium is used to steady the nerves for doing some hold act requiring special courage.
Study of Strychnus Nux Vomica:
Strychnine (Kuchila) is a powerful alkaloid obtained from the seeds of strychnous nux vomica and other species of strychnous. Fruit is round, hard, slightly rough, glossy arrange with jelly white or pale yellow pulp. It has 3-5 seeds. The seeds contain two principal alkaloids- strychnine and brucine. Strychnine occurs on colorless, odorless, poison having an intensely bitter taste.

Action : It competitively blocks ventral horn motor neuron post ganglionic receptor sites in the spinal cord and prevents the effects of glycine. Wide spread inhibition in the spinal cord results in `release’ excitation.
Fatal dose : 50 to 100mg; one crusted seed
Fatal period : One to two hours.
Sign & Symptoms :
- Onset of symptoms usually occur immediately on within 5 of 10 minutes after swallowing.
- An intense bitter taste immediately on swallowing
- An chocking sensation of throat stiffening of the neck and face and twiching of group of muscles follow.
- Convulsion occur affecting all the muscles at a time. The conulsion are first clonic affecting all muscle & relaxation in between contraction.
- During paroxysm face become cyanosed. The eyes are starring, the eye ball prominent & pupil dilated.
- Constriction of facial muscle controls the face into a horrible resemblance risus sardonicus.
- The body is arched back in the position of opisthotonos.
- Spasm of respiratory muscle may produce a sense of suffocation, which may end in asphyxia.
- Vomitting is readiuy induced.
- The mind is usully clear at the end of the life and the patient is conscious of the pain.
Treatment :
Principle: (a) Elimination of & neutralization of poison.
(b) Control of Spasm.
- The patient should be placed in a quite dark room free from noise.
- Convulsion may be controlled by Diazepam 0.1 to 0.5 mg/kg 1/v slowly and thus Phenobarbital.
- Antidote to strychnineis short acting barbiturate like betrothal sodium of sodium amytal given in dose of 0.3 to 0.6 mg 1/v.
- Wash the stomach with warm water and dilute solution of potassium permanganet.
- Acidifging urine will increase excretion of strychnine
- Symptomatic treatment.
Study of Oleander
Nerium odorum:
Nerium odorum (white oleander, kaner) grows wild in India. Flowers usually fragment. All parts of the plant including the nectar is poisonous, containing severalcardiac glycosides. primarily oleandroside (oleandrin), and nerioside (nerin), which resemble digitalis in action and folinerin and rosagenin. The nector yields poisonous honey.

Signs and symptoms:
The plant is occasionally a source of contact dermatitis. Emanations from flowers, especially when fading cause headache, dizziness, respiratory difficulty and nausea. Ingestion causes ingestion causes difficulty in swallowing and articulation, abdominal pain, vomiting, profuse forthy salivation diarrhoea. Pulse is first slow and later rapid and weak, blood pressure falls, pupils are dilated.
Fatal dose: 15 to 20 g. of the root; 5 to 15 leaves.
Treatment: (1) Stomach wash
(2) Symptomatic.
Medico-legal importance:
(1) The root, leaves or fruit are often used a paste or decoction for suicidal purposes
(2) As an abortifacient
(3) treating venereal diseases
(4) root is used for treating cancers and ulcers in the form of paste
(5) As a cattle poison
(6) Smoke from the burning plant is toxic.
Cerbera Thevetia:
All parts of cerbera thevetia (yellow oleander; pila kaner) are poisonous. The flowers are large and bell-shaped and yellow. Fruit is globular, contains a single nut. Each nut contains five pale yellow seeds. All active principles are glycosides. Milky juice exudes from all parts of the plant.

Sings and symptoms:
the sap of the plant may cause inflammation in sensitive individuals. Chewing the bark or seed kernel causes a slight numbing sensation and feeling of heat in the mouth and purging. Ingestion causes pain in the mouth, dryness of throat, tingling and numbness of tongue, vomiting, diarrhoea, headache, giddiness, dilated pupil.
Fatal dose: 8 to 10 seeds: 15 to 20 g, of roots 5 to 10 leaves.
Treatment: (1) wash out the stomach.
(2) Sodium molar lactate transfusion wit h glucose.
(3) Symptomatic.
Medico-legal importance:
(1) The roots and seeds are used sometimes for suicide or homicide.
(2) For cattle poisoning, the seeds are crushed and fed to the animal with corn and bread.
STUDY OF SNAKE:

NAMES OF POISONOUS SNAKES: Vipers, Cobras, Kraits& Sea snakes
FATAL DOSES: Cobra venom-15mg
Viper venom-20mg
FATAL PERIOD: Cobra-0.5-6hours
Viper-1-2hours
MANAGEMENT: Management of snake bites includes certain principles-
1. Prevention of spread of venom
2. Use of antivenin and other antitoxic therapy
3. General measures
1. Prevention of spread of venom:
a. Immobilization
b. Application of tourniquet or firm pressure over the bitten area
c. Cleaning the wound
2. Antitoxic therapy:
a. Use of antivenin
b. Use of adrenaline, antihistamines& corticosteroids to prevent serum sickness
3. General measures:
a. Central nervous system stimulants
b. Artificial respiration
c. Blood transfusion
d. Steroids
e. Short acting barbiturates
f. Antibiotics
STUDY OF PUFFER FISH
Synonyms of puffer fish are blow fish, swellfish, ballonfish, bubblefish, potkafish, fugu.
Scientific name is tetraodon.

TOXIN:
Puffer fish contains tetrodotoxin. Tetrodotoxin is one of the most powerful neurotoxin to man. Toxin blocks the sodium channels in the nervous tissue, ultimately paralyzing the muscle tissue.
POISONOUS PARTS:
The eyes, skin, ovaries, liver &internal organs of most puffer fish are highly toxic.
SIGNS & SYMPTOMS:
1. Onset within half an hour of ingestion.
2. Paresthesia around mouth, throat & tongue, later spread to extremities.
3. Peculiar taste & hypersalivation.
4. Headache, dysphagia, dysarthia, vomiting
5. Abdominal pain, diaphoresis, general malaise, weakness, hypotension, cardiac arrhythmia, cranial nerve dysfunction.
6. Muscle fasciculation & paralysis develops in 24 hours.
7. Consciousness may be retained throughout the illness.
8. Death may occur due to respiratory paralysis or cardiovascular collapse.
TREATMENT:
1.No definite treatment is known.
2. Main approach is supportive&symptomatic.
3.Emesis,gastric lavage,activated charcoal.
4.Anticholinesterases such as endrophonium may be effective.
MEDICOLEGAL IMPORTANCE:
1.Mainly accidental.
2.Rarely suisidal or homicidal.