Every year, 14,000 women in the United States die from ovarian cancer. It’s the fifth-highest cause of cancer death in women, and it’s especially lethal because it’s difficult to detect early on. Patients frequently don’t notice symptoms until cancer has spread, and there are no viable early detection tests available.
A group of scientists is striving to fix this. Memorial Sloan Kettering Cancer Center, Weill Cornell Medicine, the University of Maryland, the National Institutes of Standards and Technology, and Lehigh University are among the researchers in the organization.
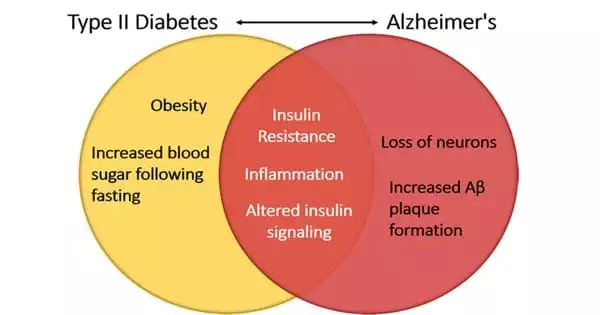
Ovarian cancer is a cancerous development of cells in the ovaries. The cells reproduce rapidly and have the ability to infiltrate and kill healthy body tissue. Bloating, for example, is not usually a symptom of ovarian cancer. Ovarian cancer is frequently discovered late, although early detection can make it easier to cure.
Two recent studies explain their progress toward a new ovarian cancer screening tool. Machine learning techniques are used to efficiently evaluate spectral fingerprints of carbon nanotubes in order to discover disease biomarkers and recognize cancer itself.
The first paper appeared in Science Advances in November.
“We demonstrated that a perception-based nanosensor platform could detect ovarian cancer biomarkers using machine learning,” says Yoona Yang, a postdoctoral research associate in Lehigh’s Department of Chemical and Biomolecular Engineering and co-first author of the paper along with Zvi Yaari, postdoctoral research fellow at Memorial Sloan Kettering Cancer Center in New York.
Ming Zheng, a research chemist at the National Institute of Standards and Technology, Anand Jagota, a professor of bioengineering and chemical and biomolecular engineering at Lehigh University, and Daniel Heller, associate member and head of the Memorial Sloan Kettering Cancer Center’s Cancer Nanotechnology Laboratory, were also among the authors.
Jagota, who also serves as associate dean of research for Lehigh’s College of Health, and Yang are members of Lehigh’s Nano | Human Interfaces Presidential Initiative, a multidisciplinary research initiative that aims to change the way we work with data and the sophisticated instruments of scientific discovery.
Perception-based sensing functions like the human brain. The system consists of a sensing array that captures a certain feature of the analytes in a specific way, and then the ensemble response from the array is analyzed by the computational perceptive model. It can detect various analytes at once, which makes it much more efficient.
Yoona Yang
Detecting illness biomarkers has traditionally required matching each marker with a molecular recognition molecule such as an antibody. However, there is no one biomarker or analyte that can detect the existence of ovarian cancer.
When many analytes must be assessed in a single sample to improve a test’s accuracy, more antibodies are required, which raises the test’s cost and turnaround time.
“Perception-based sensing functions like the human brain,” says Yang. “The system consists of a sensing array that captures a certain feature of the analytes in a specific way, and then the ensemble response from the array is analyzed by the computational perceptive model. It can detect various analytes at once, which makes it much more efficient.”
The array used in this work consisted of single-wall carbon nanotubes wrapped in DNA strands. The many ways the DNA was wrapped, as well as the different DNA sequences used, resulted in a range of surfaces on the nanotubes. The various surfaces, in turn, attracted a variety of proteins in a uterine lavage sample enriched with ovarian cancer biomarkers at varied amounts.
“Carbon nanotubes have interesting electronic properties,” says Heller. “If you shoot light at them, they emit a different color of light, and that light’s color and intensity can change based on what’s sticking to the nanotube. We were able to harness the complexity of so many potential binding interactions by using a range of nanotubes with various wrappings. And that gave us a range of different sensors that could all detect slightly different things, and it turned out they responded differently to different proteins.”
The machine-learning algorithm was trained to recognize the pattern of emission that denoted the presence and concentration of each biomarker using data from nanotube emission spectral signatures.
“The mental breakthrough here is that these nanotubes are nonspecific sensors,” says Jagota. “They don’t know anything about biomarkers, meaning they aren’t programmed to bind to anything specific. All we knew is that they can be exposed to an aqueous medium, and whatever they’re exposed to within that medium will produce spectral shifts and changes in magnitude. And using a combination of these sensors, we were able to train the algorithm to mathematically transform these inputs to outputs with high accuracy. It’s like having 20 sets of eyes that all see overlapping things. No single eye is that good, but as a collection, they can be trained to perform better than the existing detection methods for ovarian cancer.”
Many of the same researchers contributed to the second publication, which was published in March in Nature Biomedical Engineering. YuHuang Wang, a professor in the University of Maryland’s department of chemistry and biochemistry, and Mijin Kim, a postdoctoral research fellow at Memorial Sloan Kettering Cancer Center and the study’s lead author, were also among the authors.
“In this paper, we weren’t looking at biomarkers any longer, we were looking at the disease itself,” says Heller. “We wanted to know, could this technology differentiate a blood sample from a patient with ovarian cancer from a patient without ovarian cancer?”
Patients who did not have ovarian cancer included both healthy people and those who had other illnesses.
The nanotubes in this work were functionalized with quantum defects, which expanded the variety of responses that the nanotubes might produce.
“The nanotubes had a certain molecule bound to it that gave it an extra signal in terms of data,” says Jagota. “So richer data came from every nanotube-DNA combination. And the model was trained not on the biomarker, but on the disease state.”
The spectrum emissions of the nanotubes were used to create a “disease fingerprint” in the model. The model’s specificity in predicting ovarian cancer and sensitivity in detecting both known and undiscovered biomarkers of the disease were both statistically significant.
The human nose, according to Heller, is an analogue for how the machine learning model operates in both studies. There isn’t a single olfactory receptor for every smell, for example.
“Instead, there’s a bunch of different odor receptors that bind to certain molecules and create a pattern or a fingerprint of sorts,” he says.
“And that pattern gets processed by your brain, which in turn, tells you what you’re smelling. So here, there’s not one particular sensor that responds to one particular thing. But, based on the pattern of different sensors responding with various changes in color and wavelength intensity, the algorithm is able to interpret what’s a biomarker and what’s not, or what’s disease and what’s not disease.”
The team has demonstrated that their technology can diagnose ovarian cancer more accurately than current methods, although it is still unable to detect the disease in its early stages. Part of the problem, according to Heller, is obtaining enough samples to train the algorithm because so few people are diagnosed at those times.
“We’re working on determining how we can actually detect this disease at the earliest possible stages,” he says.
According to Jagota, the next steps could include branching out to develop the technology for a variety of ailments and establishing if it can be optimized to operate in clinical settings.
“And this is a technique that can be applied in a range of areas,” he says. “We’re focused on health, but it could be used to identify pollutants in the air, for example. There’s the potential to go after many different diseases and conditions, and I find that fascinating.”