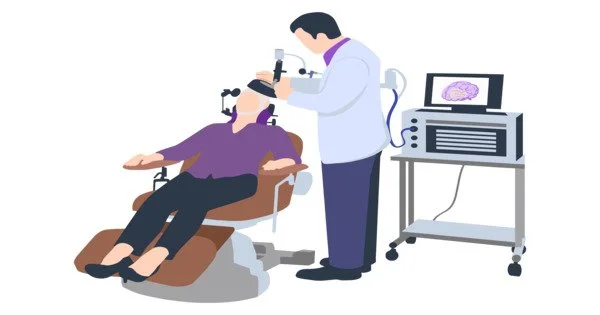
Transcranial magnetic stimulation (TMS) is a non-invasive technique used to stimulate the brain using magnetic fields. It is a treatment technique that uses a magnetic field to influence brain activity. The procedure involves placing an electromagnetic coil over a specific area of the scalp, which produces magnetic fields that penetrate the skull and stimulate the underlying brain tissue. It can be used to treat depression, obsessive-compulsive disorder, and other brain-related disorders. It is non-invasive and can be useful when other treatment options are ineffective. The side effects are usually minor and only last a short time.
It is a non-invasive treatment that involves using a magnetic coil to influence the natural electrical activity of your brain. This treatment, which was first developed in 1985, is now widely used to treat a variety of mental health and brain-related conditions. TMS has demonstrated diagnostic and therapeutic potential in the central nervous system with a wide range of disease states in neurology and mental health, and research is ongoing.
TMS is commonly used for research purposes to study brain function, and is also used clinically as a treatment for a variety of conditions, including depression, chronic pain, and neurological disorders such as Parkinson’s disease and migraine headaches.
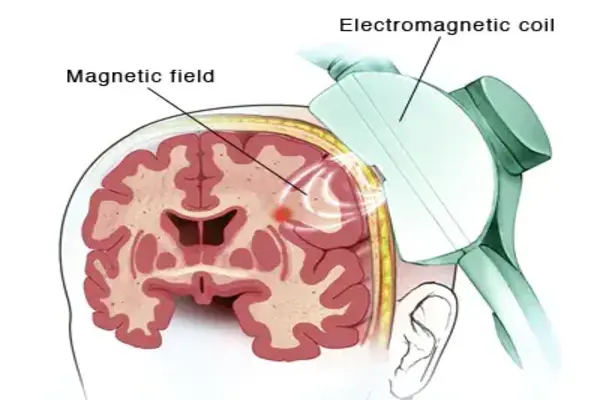
How it works?
Transcranial magnetic stimulation is based on two fundamental physics principles: electricity and magnetism. These two principles can also work together, and TMS is dependent on their ability to do so.
The space around a magnet is magnetically active, and the influence of the magnet in that space is known as the magnetic field. Even though you can’t see it, that space still exhibits the effects of the magnet at its center. When a magnet is brought close to something that conducts electricity, the interaction between the conductive item and the magnetic field produces electricity.
TMS is considered safe, with few side effects. Some people may experience headache or scalp discomfort during or after a TMS session, but these side effects are usually mild and short-lived.
Adverse effects
TMS side effects are uncommon and include fainting and seizures. Discomfort, pain, hypomania, cognitive change, hearing loss, and inadvertent current induction in implanted devices such as pacemakers or defibrillators are all potential issues. A number of reports detail other serious adverse events, such as new seizures, psychotic symptoms, and other side effects.
Although TMS is generally thought to be safe, the risks of therapeutic rTMS are higher than those of single or paired diagnostic TMS. Higher frequency stimulation generally causes more adverse effects.
The greatest immediate risk from TMS is fainting, though this is uncommon. Seizures have been reported, but are rare. Other adverse effects include short term discomfort, pain, brief episodes of hypomania, cognitive change, hearing loss, impaired working memory, and the induction of electrical currents in implanted devices such as cardiac pacemakers.
It’s important to note that TMS is not a cure for any condition and its effects can vary from person to person. Further research is needed to fully understand the potential benefits and limitations of TMS as a treatment option.