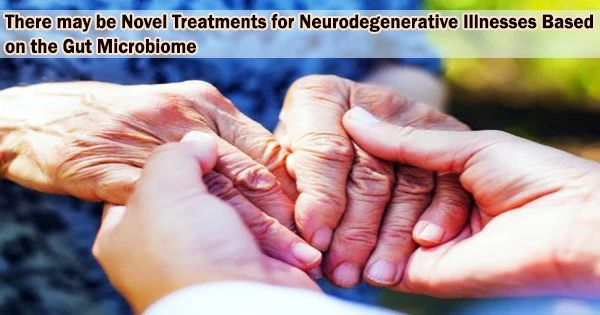
Studies have found that individuals with Parkinson’s disease have different gut bacteria compared to healthy individuals. Further research is needed to understand the specific mechanisms by which the gut microbiome may be involved in Parkinson’s disease and to determine if manipulating the gut microbiome could be a potential treatment for the disease.
Bowels don’t readily come to mind when talking about a neurological disorder. But for James Parkinson, they did.
Parkinson identified a syndrome that would ultimately be named after him in his 1817 essay on shaking palsy. A surprising symptom, constipation, was also described by the English physician and apothecary.
“The bowels, which had been all along torpid, now, in most cases, demand stimulating medicines of very considerable power,” he wrote, “the expulsion of the feces from the rectum sometimes requiring mechanical aid.”
Even though the brain’s nerve cells are most affected by Parkinson’s disease, the majority of patients also have symptoms connected to their gut. Up until the past ten years, only scientists paid them little attention.
That changed after Heiko Braak, a neuroanatomist at the University of Ulm in Germany, discovered ɑ-synuclein aggregate in 2003. Both the brain and the gastrointestinal nervous system of Parkinson’s patients have this protein clump. In light of these findings, Braak hypothesized that the sickness might start in the gut rather than the brain.
The gut is also involved in various neurological illnesses, according to further investigations. The trillions of bacteria that exist in the intestinal system have been altered or restored as a result, leading researchers to create new therapeutic possibilities.
Parkinson’s Disease May Originate in the Gut
During the last decade, Braak’s theory got support from several studies on rodents and humans. These investigations suggested that the vagus nerve, which connects the stomach to the brain, may be the route taken by synuclein aggregation. Parkinson’s risk could be decreased by cutting that nerve using a procedure known as a vagotomy, which was formerly widely performed to treat ulcers.
We don’t have any good treatments for Alzheimer’s. Haven’t had a new FDA-approved treatment for Alzheimer’s disease in over 15 years. So if you found something that was even modestly beneficial, it seems like it would be worth pursuing.
Barbara Bendlin
Despite all the indications, there has only recently been concrete scientific proof that there is a link between gut and brain disorders. In April 2020, a Sweden-based group demonstrated a causal genetic link between the gut and Parkinson’s disease in humans for the very first time.
The team sought to identify which cell types in Parkinson’s patients were contributing to the condition. Using the largest genomic database ever assembled from patient data, which was donated by the genomics business 23andMe, scientists first determined the genes that raise the risk for the condition. The corresponding cell types were then determined by mapping these genes to the known genes in the mouse nervous system.
“For all the genes that increase the risk of Parkinson’s, we found the cells that express those genes,” explained Jens Hjerling-Leffler, an assistant professor from Karolinska Institute and one of the principal investigators of the study. “If you disrupt these genes, you will disrupt the symptoms. That is the risk for the disorder.”
The group found three cell types that were involved with the disease. One was dopaminergic neurons, the nerve cells that synthesize dopamine often thought of as a “feel-good” neurotransmitter that is released when we do pleasant things or expect a reward. This was anticipated because Parkinson’s illness kills dopamine-producing nerve cells.
The discovery of the other two types of cells linked to Parkinson’s, however, astonished the researchers. The central nervous system’s insulating non-neuronal cells known as oligodendrocytes were one. The other one was nerve cells in the gut. According to Hjerling-Leffler, these nerve cells are involved very early in the disease, possibly causing it.
The Gut Microbiome Is Linked to Other Neurological Diseases
Could the gut be involved in other diseases where nerve cells are destroyed?
This was the question that Barbara Bendlin, an associate professor at the University of Wisconsin-Madison, set out to tackle. No one had studied the whole gut microbiome of human Alzheimer’s patients. Bendlin’s group did a comprehensive survey and identified that patients with Alzheimer’s had fewer types of microbes in their gut than healthy people.
The scientists found that some healthy people with comparable low levels of microbiome diversity in their stomachs also exhibited early warning signs of Alzheimer’s disease in their brains before they displayed any behavioral changes like memory loss.
Several researchers looked for answers to the same question in the field of Amyotrophic lateral sclerosis (ALS). The skeletal muscle-controlling nerve cells in the brain and spinal cord are impacted by this neurodegenerative illness. An ALS mouse model study revealed that altering the mice’s gut microbiomes altered the course of the disease.
Other studies on ALS patients found that there are changes in the microbial content of patients’ feces, as well as in their gut microbiota composition, during the course of the disease. Similarly, in a study published in 2020, researchers found that during active multiple sclerosis, immune cells unique to the gut microbiome move to the central nervous system.
All of these data point to a potential involvement for the gut in these illnesses, but they do not offer convincing proof unlike Parkinson’s disease that alterations in the gut are the direct cause of neurodegenerative illnesses. At least not yet.
“It may be that gut changes are leading to brain changes, but it could also be the case that brain changes then, in turn, affect the composition of the gut, “ explained Bendlin.
In other words, the gut may contribute to these diseases not necessarily directly but as a facilitator potentially through inflammation and other disease mechanisms.
“It sort of adds fuel to the fire,” said Nicholas Vogt, an MD/Ph.D. student from Bendlin’s group who was one of the leading scientists behind the study.
Whatever the method, figuring out the precise part played by the gut microbiota in these disorders will create new opportunities for employing the gut microbiome in treatment. Probiotics, fecal transplants, and anti-inflammatory therapies are a few choices.
Neurodegenerative diseases are devastating. From slowly losing memory in Alzheimer’s to being unable to perform basic physical tasks due to tremors in Parkinson’s, they rob patients of their bodies and their lives. These incurable disorders also cause an immense economic and social burden on patients’ families, caregivers, and society.
However, thanks to recent developments in biomedical research, experts now believe that we may be able to prevent certain brain disorders in the future by ensuring that the microorganisms in the gut remain content and healthy.
“We don’t have any good treatments for Alzheimer’s. Haven’t had a new FDA-approved treatment for Alzheimer’s disease in over 15 years,” said Bendlin. “So if you found something that was even modestly beneficial, it seems like it would be worth pursuing.”