HIV treatment (antiretroviral therapy, or ART) entails taking medication as directed by a doctor. HIV treatment helps you stay healthy by reducing the amount of HIV in your body. HIV treatment presents a number of challenges and barriers, including high treatment costs, access to care, retention in care, and transition from inpatient to outpatient care.
While standard HIV treatment can keep the virus at bay, a new study shows how experimental drugs can boost the body’s own ability to suppress the virus. According to the study’s researchers, this is an important step toward a cure.
For nearly 40 years, scientists all over the world have been unsuccessfully attempting to find a cure for HIV, but now a team of Aarhus University and Aarhus University Hospital researchers appears to have discovered an important component in the equation. So says Dr. Ole Schmeltz Sgaard, Professor of Translational Viral Research at Aarhus University and senior author of a groundbreaking study published in the journal Nature Medicine.
“This study is one of the first to be carried out on human beings in which we have demonstrated a way to strengthen the body’s own ability to fight HIV – even when today’s standard treatment is paused. We thus regard the study as an important step in the direction of a cure,” he says.
I conducted the study in close collaboration with researchers from the UK, USA, Spain, and Canada.
This study is one of the first to be carried out on human beings in which we have demonstrated a way to strengthen the body’s own ability to fight HIV – even when today’s standard treatment is paused. We thus regard the study as an important step in the direction of a cure.
Dr. Ole Schmeltz Sgaard
Virus in hiding
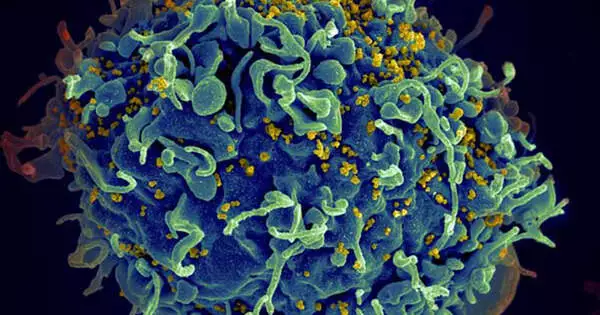
While no cure or protective vaccine for HIV has been discovered, today’s standard treatment is very effective at keeping the disease at bay. People with HIV are now given antiretroviral therapy, which reduces the amount of virus in their blood and partially restores their immune system. However, if the standard treatment is stopped, the amount of virus in the blood returns to pre-treatment levels within weeks, regardless of whether the patient is 10 or 20 years into the course of treatment.
This is because HIV hides in the genome of some of the body’s immune cells, and it is precisely these cells that the intervention is targeting in the Danish-led research project. In the study, the researchers studied the effects of two types of experimental medicine on people recently diagnosed with HIV.
Antibodies restore immunity
Participants from Denmark and the United Kingdom were randomly assigned to one of four groups, each of which received the standard treatment. Some of them were also given the drug Romidepsin, which was designed to keep the virus from hiding in the body’s immune cells, while others were given monoclonal antibodies against HIV, which may kill infected cells while also strengthening the immune system. One group received only the standard treatment, while the other received a combination of the standard treatment and both types of experimental medicine.
The results of the study are very encouraging, says Dr. Jesper Damsgaard Gunst from Aarhus University Hospital — lead author and another of the main driving forces behind the trial.
“Our study shows that newly diagnosed people with HIV who are given monoclonal antibodies together with their usual HIV medicine show a faster decrease in the amount of virus after the treatment starts and develop better immunity against HIV, and their immune system can partially or completely suppress the virus if they are taking a break from their usual HIV medicine,” he explains.
First successful clinical trial
The experiment’s theory is that the monoclonal antibodies aid the immune system in recognizing and killing infected cells. Furthermore, the antibodies bind to viruses in large complexes, which end up in lymph nodes, where they, among other things, stimulate the ability of certain immune cells to develop HIV immunity. The body may be able to control the spread of the virus and “protect” itself from the harm caused by HIV infection in this manner.
Previous clinical trials with experimental medicines have revealed no significant effects on people’s immunity to HIV or the immune system’s ability to suppress the infection if standard treatment is discontinued.
Need to optimise treatment
Despite the remarkable results, however, there is still some way to go before we will see a cure for HIV, emphasises Dr. Søgaard. First, the researchers need to find a way to optimise the treatment and amplify its effect. The Danish study has already attracted considerable attention abroad and has boosted interest in experimental trials in people with a newly diagnosed HIV infection.
The US Department of Health, for example, recently set aside a large sum of money for research in this area. Furthermore, the Bill and Melinda Gates Foundation and a large research network have taken the initiative to carry out a follow-up study in Africa to the Danish study.
Dr. Sgaard’s research group is currently working on a large study that will be conducted across Europe to optimize the new experimental treatment. “We anticipate that the improved treatment will have a greater impact on both the virus and the participants’ immunity. We hope that by doing so, we can improve the immune system’s ability to permanently suppress the remaining virus.”