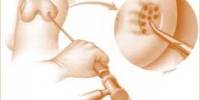
Scientists have identified specific areas in the human nose where the SARS-CoV-2 virus is likely to enter and exit the body.
Somebody just coughed on you. On a plane. At a dinner party. In a supermarket line.
If only there were a “morning after” nasal spray that could knock out respiratory viruses’ ability to colonize your nose and throat.
In a study published January 5 in the print issue of Cell, Peter Jackson, Ph.D., a Stanford Medicine professor of pathology and of microbiology and immunology, and his colleagues brought that possibility closer to reality by pinpointing the routes that SARS-CoV-2, the COVID-19 virus, takes to enter and exit cells in our nasal cavity.
“Our upper airways are the launchpad not only for infection of our lungs but for transmission to others,” Jackson said.
The virus is thought to primarily enter through the olfactory epithelium, a specialized region in the upper part of the nasal cavity that is responsible for sensing odors. It is also believed to exit through the nasal-associated lymphoid tissue (NALT) and the nasopharynx, which are located at the back of the nasal cavity.
Jackson shares senior authorship of the study the first to describe COVID-19 nasal infection in molecular detail with Raul Andino, Ph.D., professor of microbiology and immunology at UC San Francisco. The lead authors are former Stanford Medicine postdoctoral scholar Chien-ting Wu, Ph.D., and graduate student Ran Cheng, along with UCSF postdoctoral scholars Peter Lidsky, Ph.D., and Yinghong Xiao, Ph.D.
A river runs through it
Basal cells, goblet cells, and multiciliated cells, which account for around 80% of all the cells in the nasal epithelium, line the inside of the nose and the airway. A barrier made of multiciliated cells blocks the entry of viruses into the airway.
Jackson and his colleagues zoomed in on two structures found on multiciliated epithelial cells: cilia and microvilli. Although both are well known, neither structure has previously been implicated in how the virus enters or exits the cells lining the airway.
Cilia are spaghetti-like protrusions from various cell surfaces that face outward. As many as 400 of these whip-like strands may be present on the nasal cavity-facing surface of a single nasal epithelial cell, and they are all continuously beating in unison. They have a thin coating of mucin, a protein that is related to the main mucus protein, and then a mucus coat on top of that.
“Mucin molecules can hook up with one another to form a mesh akin to an elastic, three-dimensional chain-link fence, preventing larger viruses such as SARS-CoV-2 from getting into upper-airway cells,” Jackson said. The mucus coat catches bacteria, viruses, environmental debris, and cell-degradation waste while also keeping the underlying cells wet.
Through this mucus layer, upper-airway epithelial cilia protrude, and their coordinated beat creates a wave that moves the mucus and its entrapped particles like a slow-moving river to where they can be expectorated or, alternatively, swallowed and digested.
Microvilli, which look like little fingers protruding from the cell surface and are smaller spikes, are another characteristic shared by almost all animal cells. Microvilli can grab and transport subcellular particles and vesicles.
You say goodbye, and I say hello
Jackson and his colleagues developed what they call airway epithelial organoids, which resemble normal airways, using a sophisticated tissue culture technique to study what transpires during a nascent viral infection up close. These organoids completely mimic the structure of the nasal epithelium, including a whole mucus-mucin layer and well-developed multiciliated cells, while lacking blood vessels and immune cells.
The scientists inoculated the cultures by incubating them in the same dish with SARS-CoV-2. They observed the entry, multiplication, and exit of viruses in the epithelial cells using optical and electron microscopy as well as immunochemical labeling.
Only ciliated cells became infected. According to electron microscopy, the virus only first adheres to cilia. Organoids infected with SARS-CoV-2 six hours later had a large number of virus particles covering the sides of the cilia from the tips down. Only a few cells were experiencing viral replication even 24 hours after the inoculation. It took 48 hours for massive replication to occur.
SARS-CoV-2 needs a full day or two to start replicating full-tilt in real life, too.
Depleting the cilia, by knocking down levels of a protein critical to cilia formation in nasal epithelial cells, severely slowed down SARS-CoV-2 infection.
“It’s clear that human ciliated nasal epithelial cells are the primary entry site for SARS-CoV-2 in nasal epithelial tissue,” Jackson said.
The researchers treated the airway organoids with a mucin-selective enzyme that dissolves the mucin-network mesh because they hypothesized that the airway mucus-mucin barrier the virus must pass is the cause of the delayed infection. It sped up virus entry at 24 hours from “barely detectable to easily detectable,” said Jackson, who concludes that eliminating mucin from this mesh prevented the mesh from blocking SARS-CoV-2 infection of the organoids.
Mucus flow loses directionality in people with primary ciliary dyskinesia, a very uncommon condition in which the ability of the cilia to beat in sync is impaired or lost.
The viral attachment to cilia in airway organoids made from these individuals was similar to that in healthy cells. Cell-infection rates were comparable to those of typically infected cells 24 hours after immunization. Normal-looking microvilli bristled on cell surfaces.
SARS-CoV-2, however, was infecting significantly fewer cells overall at 48 hours; it could only spread to the cells that were right next to it, indicating that once the virus has begun to replicate within infected cells, it depends on a sufficient flow of mucus to spread throughout the upper airways.
Jackson co-authored a paper published in Nature Communications in May 2020 that demonstrated the concentration of ACE2, the traditional SARS-CoV-2-binding cell-surface molecule or receptor, on the cilia of nasal epithelial cells. According to a recent Cell study, this receptor allowed SARS-CoV-2 to bind to epithelial cilia.
From there, Jackson said, the virus might slip past the mucus-mucin barrier in one of two ways: either by skipping down the side of cilia, hopscotch-style, from one ACE2 molecule to the next until it reaches the cell’s main body, fusing with the cell membrane there and climbing in; or by wedging its way into the cilium and riding an internal freight elevator down to the cell body.
“Once the virus gets through that barrier,” he said, “it can replicate freely in underlying cells.”
The researchers also discovered that SARS-CoV-2 causes intracellular enzymes to become active after it enters the cell, which causes microvilli to grow and branch out like crazy cactus plants until their tips protrude over the mucus barrier. Their numbers increase.
Within 24 hours after vaccination, many altered microvilli, which are typically less than half the length of cilia, have transformed into enormous, branching, tree-like structures that are the size of cilia or larger. These structures are embellished with viral particles that can protrude into the mucus-mucin layer, where they can float down the mucus river and infect other, farther away cells.
The enzymes in the cell that were triggering the alteration of the microvilli were identified by the researchers as being massively turned on by SARS-CoV-2 infection. These enzymes’ inhibition stopped that aberration and significantly reduced the virus’s ability to infect other cells.
One spray to bind them all?
Jackson and his colleagues had similar results when they incubated airway organoids with either of two other respiratory viruses the now-surging respiratory syncytial virus and the less-common parainfluenza virus as well as with BA.1, a variant of the omicron strain.
Omicron is more contagious than the older strain employed in the other SARS-CoV-2 trials, and as would be predicted, it infected airway-organoid multiciliated cells more quickly. However, even for this highly contagious variety, blocking viral entry or exit in airway cells was effective.
These viral entry mechanisms may be a general property of many respiratory viruses, Jackson said.
The research identifies novel targets for a nasally administered medication that, by limiting ciliary motion or microvilli gigantism, could stop even unknown respiratory viruses, such as those you could encounter during a pandemic, from colonizing your nose or throat.
According to Jackson, the chemicals utilized in these tests may be improved for use in, say, nasal sprays administered immediately following a respiratory viral exposure or as preventatives.
“Delaying viral entry, exit or spread with a locally applied, short-duration drug would help our immune systems catch up and arrive in time to stop full-blown infection and hopefully limit future pandemics,” he said.