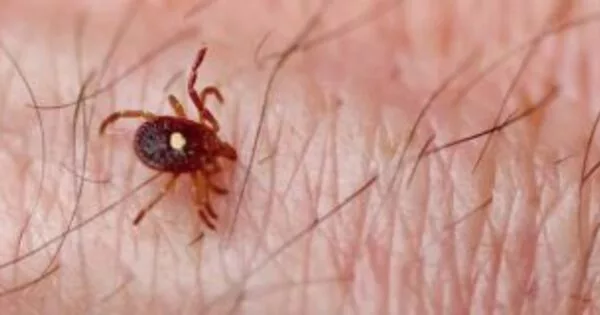
Meat allergy is a condition that occurs when the immune system reacts to proteins found in certain meats, such as beef, pork, and lamb. In some cases, a person may develop a meat allergy as a result of being bitten by a tick. This type of allergy is known as alpha-gal allergy, and it is caused by a type of sugar called alpha-gal that is found in the saliva of certain ticks.
Recent research has provided insights into the genetic and molecular basis of alpha-gal allergy. For example, studies have shown that the allergy is caused by an immune system response to alpha-gal that is triggered by the bite of a tick. The immune system produces antibodies to the alpha-gal sugar, which can then lead to an allergic reaction when a person eats meat that contains alpha-gal.
Other research has focused on understanding the molecular mechanisms that underlie the development of alpha-gal allergy. For example, studies have shown that the immune system response to alpha-gal involves the activation of certain immune cells and the release of inflammatory chemicals called cytokines.
Scientists have discovered the genetic and molecular structure of key molecules linked to the potentially fatal mammalian-meat allergy caused by tick bites.
The study, led by Garvan Institute of Medical Research researchers, examines how antibodies interact with the sugar molecule galactose-α-1,3-galactose (alpha-gal/-gal), which is produced by all mammals except humans and higher primates. It supports the role of -gal as the key molecule in this rare allergy.
We have more than 70 types of antibodies and this one is significantly overrepresented with α-gal recognition. We seem to be genetically predisposed to being sensitive to this sugar.
Professor Christ
When humans are exposed to -gal through tick bites, such as the paralysis tick Ixodes holocyclus, which is endemic to Eastern Australia, the immune system can recognize it as harmful and initiate an allergic response, which can be fatal.
Lead author Professor Daniel Christ, Head of Antibody Therapeutics and Director of the Centre for Targeted Therapy at Garvan, says the molecular analysis showed that a particular antibody type (3-7) has a natural pocket into which α-gal snugly fits.
“We have more than 70 types of antibodies and this one is significantly overrepresented with α-gal recognition. We seem to be genetically predisposed to being sensitive to this sugar,” Professor Christ says.
The new study, published this week in the journal Proceedings of the National Academy of Sciences (PNAS), paves the way for potential therapeutic candidates for treating the rare allergic response.

Evolutionary benefit to immune reaction to α-gal
Scientists analyzed the blood of patients with mammalian-meat allergy to determine which antibodies were produced: the 3-7 type was found frequently in response to α-gal.
The data points to an evolutionary benefit of having an antibody response that can mobilize against α-gal.
“Humans lost the capacity to produce α-gal throughout evolution, but we don’t know why,” says Associate Professor Joanne Reed, co-senior author of this study, from the Westmead Institute. “The suspicion is that it has to do with protection against infectious disease.”
Professor Christ points to recent research on malaria, which shows the Plasmodium parasite has an α-gal coating on its surface. A rapid immune response to α-gal could destroy the parasite before it takes hold, protecting a person from malaria.
NSW is a global hotspot for tick-induced mammalian-meat allergy
Sydney’s northern region is a global hot spot for mammalian-meat allergy, with more than 1800 cases reported and the highest prevalence in the world. The Sunshine Coast hinterland around Maleny in Queensland is also another hot spot. The paralysis tick (Ixodes holocyclus) is found in those areas.
Professor Sheryl van Nunen, an allergy specialist at Sydney’s Northern Beaches Hospital, and a co-author on the paper, was the first clinician to link tick bites with mammalian-meat allergy. “There isn’t a week go by that I wouldn’t see two people with this allergy,” she says.
Why some people develop anaphylaxis and others never respond is unknown. Professor van Nunen says it could be related to the number of tick bites, how much saliva is injected or genetic sensitivity.
Exposure happens when α-gal, present in the saliva of certain tick species, is injected during a bite, says Professor van Nunen. About one-third of people who have developed a sensitivity to α-gal will exhibit symptoms of an allergy to mammalian meat, she says. And another bite can more than double the allergic response. Some people with a severe allergy can be affected by the presence of meat products in food, like beef broth, soft cheeses such as feta or goat’s cheese, or even gelatin.