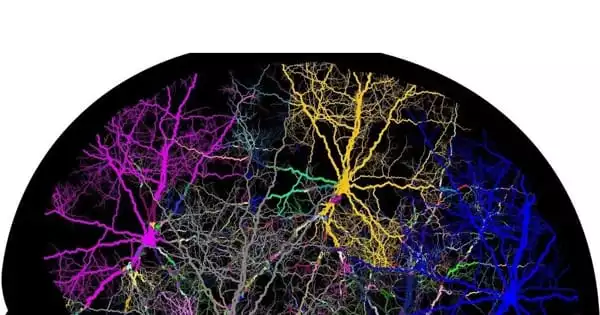
When a heavy alcoholic drinker tries to take a night off, their body protests with shaky hands, heart palpitations, anxiety, and headaches. These immediate symptoms of alcohol withdrawal, but perhaps more so the lingering emotional pain that comes with protracted abstinence, are one of the reasons people with alcohol use disorders struggle to quit. Scientists at Scripps Research have made significant progress in understanding the neural basis of alcohol withdrawal.
Previously, a signaling molecule known as corticotropin-releasing factor (CRF) was associated to alcohol withdrawal; when researchers blocked CRF in alcohol-addicted rats or mice, the animals drank less. The suspicious CRF, according to scientists, is created by neurons in a brain location known as the central nucleus of the amygdala. However, in a new study published in the journal Molecular Psychiatry, the researchers discovered that, at least in mice, these cells aren’t essential for alcohol withdrawal or dependency.
“Understanding the basis of withdrawal is incredibly important for treating alcohol addiction in humans, because this is one of the motivational drivers of excessive alcohol drinking,” says Candice Contet, Ph.D., associate professor in the Department of Molecular Medicine at Scripps Research. “These findings weren’t what we expected, but help us get closer to understanding alcohol addiction and the role of CRF.”
We basically discovered that stimulating these neurons within the central amygdala is neither sufficient nor necessary for the escalation of drinking in mice. This suggests that the CRF is flowing from somewhere else in the brain to the central amygdala.
Candice Contet
Numerous studies have shown that CRF levels rise in the central nucleus of the amygdala of rats and mice after alcohol withdrawal and in response to other psychological stressors. Pharmaceutical companies are working hard to figure out how to target CRF signaling to treat a range of psychological illnesses, including alcoholism. However, human studies have yielded conflicting results, and scientists have been unable to pinpoint which cells in the brain generate CRF during alcohol withdrawal.
Contet’s team intended to see if cells in the central amygdala create the CRF required for alcohol withdrawal. In the latest study, the researchers stimulated and deactivated these amygdala-resident neurons in alcohol-dependent mice. First, scientists triggered the neurons in a variety of ways intended to mimic cycles of recurrent drinking and withdrawal. Activating these CRF-producing neurons, however, had no effect on the drinking behavior of the mice, despite the fact that previous trials revealed that CRF was produced in the central amygdala.
The researchers next demonstrated that inhibiting these neurons had no effect on the behavior of mice with alcoholism, which was surprising because it meant that the CRF, which is known to signal in the amygdala to increase alcohol consumption, was not being created in that location.
“We basically discovered that stimulating these neurons within the central amygdala is neither sufficient nor necessary for the escalation of drinking in mice,” Contet explains. “This suggests that the CRF is flowing from somewhere else in the brain to the central amygdala.” Other neurons in the brain are known to make CRF, but the researchers aren’t sure which ones are implicated in alcoholism.
“These findings were surprising, but they illustrate the intricacy of the CRF system and the alterations in brain circuitry that occur with persistent alcohol exposure,” says Melissa Herman, co-first author of the current work and a former Scripps Research postdoctoral research associate.
When the researchers examined the spatial patterns of organization of the amygdala neurons they were researching, they discovered that the CRF neurons were not structured in the same manner in mice brains as they are in rat brains. According to Contet, the observation implies that CRF may differ between species. This could also explain why the amygdala neurons in question have been discovered to be required for alcohol withdrawal in rats but not in mice, according to the new study.
“When it comes to human implications, our statistics should be taken with a grain of salt,” she says. “Because there is such a significant difference between rats and mice, more research is undoubtedly required to determine the applicability to humans.”
The researchers are planning trials to learn more about the changes in CRF between rats and mice, as well as which other neurons in the brain may be involved in its creation during alcohol withdrawal.